Other Types Of Eczema
Eczema is the name for a group of skin conditions that cause dry, irritated skin.
Other types of eczema include:
- discoid eczema a type of eczema that occurs in circular or oval patches on the skin
- contact dermatitis a type of eczema that occurs when the body comes into contact with a particular substance
- varicose eczema a type of eczema that most often affects the lower legs and is caused by problems with the flow of blood through the leg veins
- seborrhoeic eczema a type of eczema where red, scaly patches develop on the sides of the nose, eyebrows, ears and scalp
- dyshidrotic eczema a type of eczema that causes tiny blisters to erupt across the palms of the hands
Page last reviewed: 05 December 2019 Next review due: 05 December 2022
Foods That May Trigger Eczema
Any food may act as a trigger food for eczema, but some foods are more commonly responsible than others. These include
- cows milk and dairy products
- eggs
- tropical fruits
- some additives
If you are thinking about introducing solid foods to your baby and he has eczema or is at an increased risk of developing eczema, then you should avoid these foods until your baby is AT LEAST one year of age . You should also discuss the introduction of these foods with your childs doctor.
If your baby is already enjoying solids then it is worth trying to establish whether or not any of the foods listed above are making his eczema worse.
In some cases, food sensitivity can occur within 2 hours of eating the trigger food and you may notice that your babys itching and scratching increases.
More commonly, food sensitivity is delayed and the worsening symptoms dont become obvious until between 6 and 24 hours after the food is eaten.
Keep a food diary, noting foods given and the symptoms experienced and discuss them with your doctor.
Dont try eliminating foods without supervision a dietitian may be needed to advise you about the best way to keep your babys diet nutritionally balanced when certain foods are removed.
Atopic Dermatitis Asthma And Allergies
Atopic dermatitis can exist with other known medical conditions. These other conditions are called comorbidities.
Atopic dermatitis is part of a group of allergic conditions. In fact, atopic means allergy. These include, asthma, hay fever and food allergies. If a child has one of these conditions, the likelihood of developing another atopic condition is increased. Contact dermatitis is also considered atopic, though its connection to asthma and hay fever is unknown.
About 50 percent of children with moderate to severe atopic dermatitis develop allergic asthma. Symptoms of allergic asthma include:
- Coughing
Recommended Reading: What Is The Medicine For Eczema
What Causes Eczema In Children
Researchers dont know exactly what causes baby eczema, but they believe its most likely due to a combination of genetic and environmental factors. Eczema is not contagious.
Infants are more likely to develop eczema if family members have a history of eczema, hay fever, or asthma.
While these conditions don’t cause one another, infants are more likely to develop hay fever or asthma if they already have baby eczema.
Scientists believe eczema results from an immune-system dysfunction that affects the skin barrier and its ability to hold in moisture.
Eczema is a general term to describe a number of inflammatory skin conditions. Aside from atopic dermatitis, other types of eczema that commonly affect children include contact dermatitis, dyshidrotic eczema , and seborrheic dermatitis, or scalp eczema .
The Atopic March Food Allergies And Eczema

Eczema and food allergies are very closely related. They are both considered allergic conditions, and they are both part of a progression known as the atopic march.
What is the atopic march? According to the atopic march, children with one allergic condition are at increased risk for others, and allergic conditions often appear in a certain order. In other words, one condition usually marches in front of the other, in a fairly predictable lineup.
Eczema comes before food allergies in the atopic march. This means babies usually develop eczema before food allergies, and babies with eczema are at the highest risk for food allergies.
But even though food allergies and eczema are closely related, and even though some symptoms may look similar, eczema rash is not the same as a food allergy reaction.
Food allergy rashes appear as raised bumps, which look different from the red, scaly rash of eczema. Learn more about how to tell the difference between a food allergy reaction and an eczema flare-up.
You May Like: Eczema And Pimples On Face
What Are Other Ways To Help Prevent Food Allergy
Many health professionals now think there are two steps parents can take to help prevent food allergy.
Health Canada recommends introducing solid foods to babies starting at six months of age. Babies with eczema should also be offered solid foods starting at six months.
You can introduce boneless fish, egg, peanuts, tree nuts, and sesame seeds in age appropriate forms starting at six months of age if you wish. Whole tree nuts and big globs of peanut butter are choking hazards. You can start by offering peanut, tree nut and sesame seed butters mixed into infant cereal.
When your baby is ready for finger foods, you can offer these foods spread thinly on small strips of toast. For more information about introducing solid foods to babies, see “Baby’s First Foods” and “Reducing Risk of Food Allergy in Your Baby“.
Since 2008, the American Academy of Pediatrics no longer recommends delaying the introduction of foods such as fish, eggs and foods that contain peanut protein beyond 4 to 6 months of age to babies at increased risk for allergy.
Is Your Baby At A High Risk Of Developing Eczema
Around 10-20% of babies have eczema during their first year of life. Some babies are affected by it very early, whereas others develop it later on. There are certain factors that mean your baby may be at an increased risk of developing eczema
- If you have another child with an atopic condition*, then your baby is considered to be at a low risk of developing eczema.
- If you or your partner have an atopic condition*, then your baby is at a moderate risk of developing eczema.
- If you AND your partner have an atopic condition* , then your baby is at a high risk of developing eczema.
*Atopic conditions include asthma, eczema, hay fever and food allergy.
But some babies do develop eczema even when no family members suffer from any kind of atopic condition.
Recommended Reading: How Do You Stop Eczema Flare Ups
Taming The Immune Response
Prescription skin meds that calm an overactive immune system can treat eczema from atopic dermatitis. Doctors generally prescribe them only for short-term use in people whoâve tried other treatments that havenât helped. They have a “black box” warning due to a higher cancer risk. So ask your doctor about the pros and cons. A biologic medication called Dupixent, given as a shot, works on the immune system to treat atopic dermatitis.
Can Food Allergy Cause Eczema
Although food allergy is more common in children who have eczema, they are separate conditions.
Food allergy does not normally cause eczema, but having eczema may increase the chance that a food allergy develops. For a description of how eczema may increase the risk of food allergy, please refer to the section on the next page called: How can good eczema control help prevent food allergy?
You May Like: How To Heal Eczema Without Steroids
The Link Between Diet And Eczema
Some children with atopic eczema may have a food allergy that can worsen their symptoms.
In fact, eczema in babies is often the first sign that a food allergy exists and it is usually babies with severe eczema for whom food allergy is the most likely culprit.
Although sensitivity to certain foods is a trigger for eczema in around 30% of children, it is only the main or sole trigger in around 10% of cases.
This means that identifying the problem foods can certainly help your baby, but it may not eradicate the eczema altogether.
Foods that act as a trigger for eczema may cause other typical food allergy reactions, too.
There is some research that shows that children with atopic eczema may absorb food in their gut differently to other children. This is why some may experience reactions to foods and is another good reason to delay the introduction of solids until at least 6 months of age.
When To Call A Doctor
Make the call if your babys eczema doesnt begin to get better within a week of starting over-the-counter hydrocortisone creams. It may be time for a prescription medicine.
Also check with your doctor if yellow or light brown crust or pus-filled blisters appear on top of the eczema. This could be the sign of a bacterial infection that needs antibiotics.
You should call your doctor if your baby is around anyone who has cold sores or genital herpes. Eczema can make your little one more likely to pick up those germs.
Don’t Miss: Does Hydrocortisone Cream Help Eczema
Use Skin Medications When Needed
For some babies and children with eczema, daily bathing and moisturizing is not enough for good control. These children also need a medical treatment plan, which often includes medicated creams or ointments that calm the immune system in the skin and control irritation. Medical treatment plans also include instructions on how often and when to apply the cream or ointment.
There are a variety of skin medications available for eczema, each with a different strength. The strength of the medication prescribed should be right for the area of the body that needs medication. For example, a child may have one medication prescribed for the face and another one for the elbows and knees. Do not use the percent on the label to judge the strength of your child’s medication. Speak to your child’s doctor or pharmacist if you have questions about medication strength.
Follow the treatment plan provided by your child’s doctor, so your child gets the most possible benefit from the medication. It is especially important to follow your doctor’s advice about how much of the medication to apply, so you do not use too little or too much. Some doctors recommend applying a layer of medication to eczema patches every day for about two to four weeks. The medication is more effective if you apply it to skin immediately after the bath, while the skin is still damp.
Treatment Options For Eczema
The most effective way to prevent and minimize flare-ups is to keep the childs skin moisturized, treat inflammation and identify and remove irritating substances from the childs environment. The doctor can prescribe a cortisone-containing cream to relieve itching and inflammation. Once the rash is under control, treatment usually is switched to nonmedicated moisturizers to soothe the childs skin. The pediatrician also may prescribe an antihistamine to control itching. If the skin is broken and infected, a course of antibiotics may be necessary.
You May Like: Google How Do You Spell Eczema
Does My Child Have Eczema
Eczema can look different at different ages:
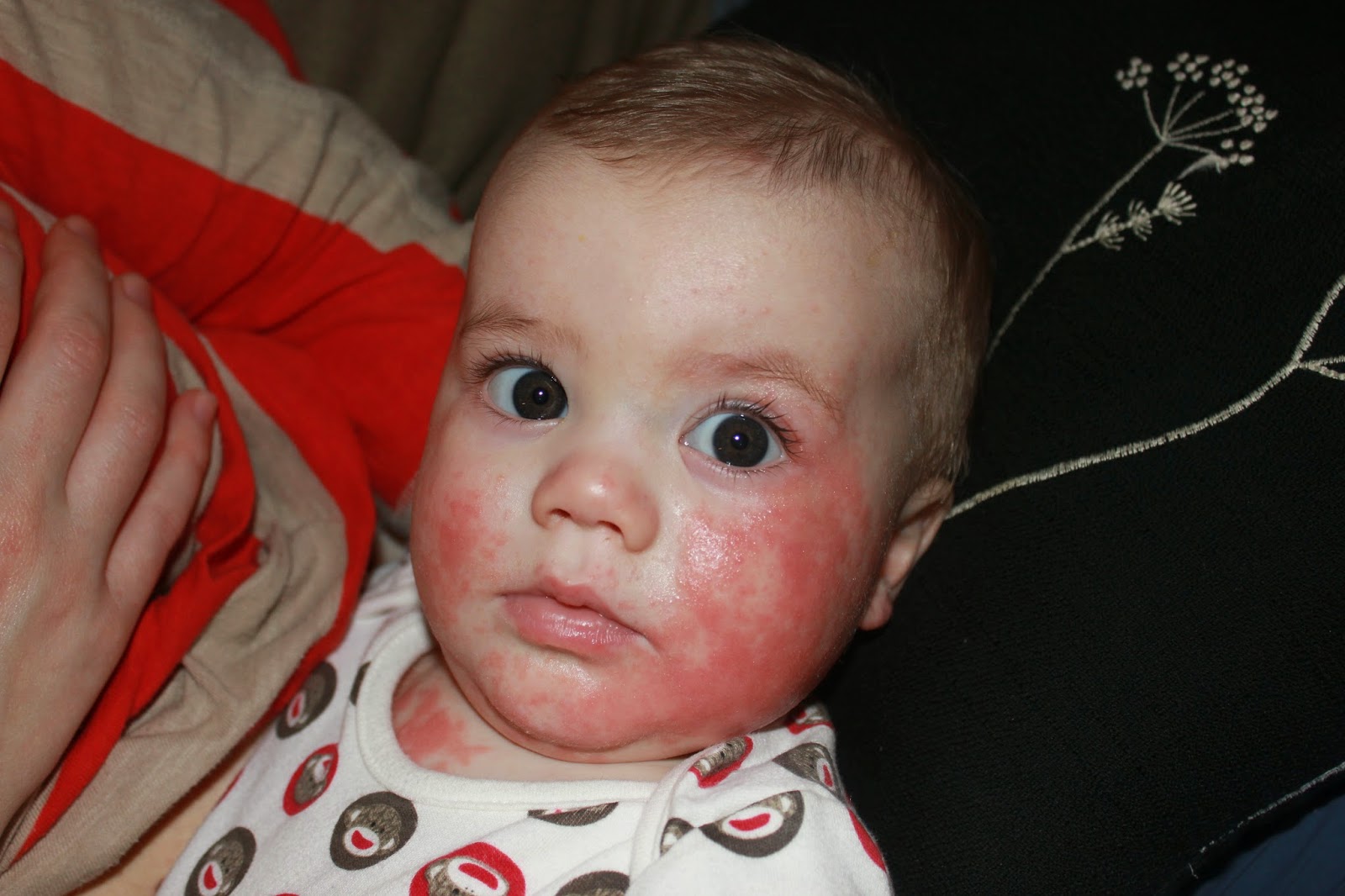
- Babies usually have a rash on their face and neck which may weep and crust.
- Children often have a dry rash, characteristically in the creases of knees and elbows, around the mouth, neck, wrists and ankles.
- From age 12, the it may be more widespread and severe.
When the skin is red, dry and itchy, it is known as a ‘flare-up’. It is common for the severity of eczema to change, sometimes it is very mild and other times it gets worse. Between flare-ups, people with eczema tend to have dry sensitive skin.
See your doctor to diagnose your child’s rash, as other skin conditions can look similar to eczema. Your doctor will examine the rash, ask you about how and when it began, and ask whether other family members have noticed a similar rash. This is because while not contagious, eczema may have a genetic basis and does tend to run in families. A child with eczema often has one or more relative with eczema or a related condition, such as asthma, hay fever or allergic conjunctivitis.
Causes Of Atopic Eczema
The exact cause of atopic eczema is unknown, but it’s clear it is not down to one single thing.
Atopic eczema often occurs in people who get allergies. “Atopic” means sensitivity to allergens.
It can run in families, and often develops alongside other conditions, such as asthma and hay fever.
The symptoms of atopic eczema often have certain triggers, such as soaps, detergents, stress and the weather.
Sometimes food allergies can play a part, especially in young children with severe eczema.
You may be asked to keep a food diary to try to determine whether a specific food makes your symptoms worse.
Allergy tests are not usually needed, although they’re sometimes helpful in identifying whether a food allergy may be triggering symptoms.
Read Also: Peaceful Mountain Eczema Rescue Reviews
Why Did My Child Develop Eczema
The exact cause of eczema is unknown. Researchers do know that children who develop eczema do so because of a combination of genes and environmental triggers. When something outside the body switches on the immune system, skin cells dont behave as they should causing flare ups.
We also know that children who come from families with a history of atopic dermatitis, asthma, or hay fever are more likely to develop atopic dermatitis.
What Causes Eczema To Wax To Flare
Different “triggers” can make eczema worse. For infants, these can be irritants such as wool, certain detergents or extreme temperatures, or other immune triggers, such as food allergies and asthma, and even pet dander.
Most kids with the condition have the hardest time in winter, when the air is cold and dry. A small percentage has a harder time in the summer, when it is hot and humid.
Read Also: Best Cream For Eczema Around Eyes
What Causes Eczema
Some children are more prone to eczema due to differences in their skin and their immune systems:
When it is red and itchy, it is even harder for skin to be a good barrier, so it lets in even more irritants. This leads to a cycle of itching, scratching and more irritation, which makes eczema worse.
Eczema belongs to a group of allergic conditions including asthma, hay fever, and food allergy. Allergic conditions tend to run in families. Genetics has a major role in determining who will get eczema. Eczema is not caused by a single gene, rather many genes act together to increase the chance of eczema developing.
An example of one gene that has a role is called filaggrin . It is responsible for making the skin protein filaggrin. When this gene is not working properly, the barrier function of the skin does not work as well. Many, but not all, children with eczema have a problem with this particular gene.
What is food allergy?
What You Can Do
You can help reduce your child’s discomfort by:
- keeping their fingernails short to reduce the damage to their skin from scratching
- washing them with aqueous cream instead of soap – ask your pharmacist about aqueous creams and always follow the instructions on the product
- using non-biological detergent and a double rinse cycle when washing their clothes or bedding
- avoiding herbal, ‘natural’ or alternative creams – these can make eczema worse, as they may contain bacteria or high doses of steroids
- rinsing and drying them well after swimming
- dressing them in cool, breathable fabrics like cotton
- keeping them away from anyone with a cold sore – as the cold sore virus can cause eczema to become infected
- using extra moisturiser on areas your child scratches a lot
- avoiding anything you know that causes your childs eczema to get worse
Around 6 out of 10 children with eczema will grow out of it by the time they’re teenagers.
Also Check: Best Diaper Rash Cream For Eczema
Baby Eczema Risk Factors And The Environment
While baby eczema is the result of immune-system dysfunction, likely from a genetic predisposition, studies have found a number of risk factors.
For example, a study published in February 2018 in the International Journal of Environmental Research and Public Health suggested that children have a higher risk of developing eczema if their mothers experienced high-stress situations during pregnancy.
In a study published in May 2018 in the Journal of Allergy and Clinical Immunology, researchers in the United Kingdom analyzed the sociodemographic characteristics of about 675,000 children in a primary-care database. They found that the children were more likely to be diagnosed with eczema if they fit one of the following descriptions:
- Male
- Black Caribbean
- Of high socioeconomic status
Another study, published in May 2018 in the Journal of the European Academy of Dermatology and Venereology, looked at how the outdoor environment specifically air pollutants and meteorological conditions affected eczema risk in children of both sexes. The researchers concluded that high levels of carbon monoxide, ammonia, formaldehyde, lead, particulate matter, and ozone levels may all influence the development of infantile eczema.