How Is Eczema Treated What Medications Are Used
Treating eczema can be difficult if the cause is something you cant control, like genetics. Fortunately, you may have some influence over your environment and stress levels. Do your best to figure out what triggers or worsens your eczema, and then avoid it. The goal is to reduce itching and discomfort and prevent infection and additional flare-ups.
Consider these treatment tips:
If your child has skin problems, such as eczema, you can:
- Avoid long, hot baths, which can dry the skin. Use lukewarm water instead and give your child sponge baths.
- Apply lotion immediately after bathing while the skin is still moist. This will help trap moisture in the skin.
- Keep the room temperature as regular as possible. Changes in room temperature and humidity can dry the skin.
- Keep your child dressed in cotton. Wool, silk and manmade fabrics such as polyester can irritate the skin.
- Use mild laundry soap and make sure that clothes are well rinsed.
- Watch for skin infections. Contact your healthcare provider if you notice an infection.
- Help them avoid rubbing or scratching the rash.
- Use moisturizers several times daily. In infants with eczema, moisturizing on a regular basis is extremely helpful.
Autoreactive T Cells As A Result Of Crossreactivity Or De Novo Sensitization
T helper cells of the Th2 subtype are capable of initiating the class switch in B cells to induce the production of antigen-specific IgE. In AD, the T cell response is together with skin barrier disturbance regarded as the central disease mechanism. T cells home to the skin in AD patients , and those isolated from the inflamed, lesional AD skin have been shown to react to environmental allergens . It has been observed that during an ongoing acute or chronic AD inflammation, skin-infiltrating T cells are mostly T helper cells. Nevertheless, CD8+ T cells are also present and furthermore, these have been described to be crucial in initiating the skin inflammation . Regarding T cell polarizations, first of all Th2, but also Th1, Th17, and Th22 T cells have been described to contribute to the pathogenesis of AD . These appear to be a result of the allergen, the inflammatory milieu, and/or the disease progression. To explain this heterogeneity, it has been proposed that the Th1-predominance in chronic AD lesions might be a result of T cell responses to non-classical allergens like autoallergens. However, analyzes of autoallergen-specific T cell responses confirm this theory only partially.
The identification of autoreactive T cells homing to / infiltrating in the skin clearly indicates that these promote the pro-inflammatory milieu in the inflammatory response in affected patients. However, relatively low numbers of participants narrow the impact of these experiments.
For The First Time A Team Led By Researchers At The Icahn School Of Medicine At Mount Sinai Has Proven That Atopic Dermatitis Also Known As Eczema Is An Immune
- New York
For the first time, a team led by researchers at the Icahn School of Medicine at Mount Sinai has proven that atopic dermatitis, also known as eczema, is an immune-driven disease at the molecular level. The study, a collaboration with Regeneron Pharmaceuticals, Sanofi and Rockefeller University, was published online earlier this month in the Journal of Allergy and Clinical Immunology.
Past studies had shown that drugs which broadly suppress the immune system reduce symptoms in patients with the disease, but the field had not described in detail the molecular mechanisms involved. Some researchers had argued in the past that genetic or environmental factors were the greater contributors to risk.
In the current study, Emma Guttman-Yassky, MD, PhD, Associate Professor of Dermatology at the Icahn School of Medicine at Mount Sinai and her team of researchers found that dupilumab, a monoclonal antibody treatment that blocks the action of two key signaling proteins, interleukin -4 and -13,reversed disease processes seen in the skin of patients at the molecular level. Dupilumab is an experimental drug being development by study partner Regeneron Pharmaceuticals that is currently in clinical trials for several conditions with immune or autoimmune mechanisms.
About the Mount Sinai Health System
For more information, visit or find Mount Sinai on , and .
Don’t Miss: Why Has My Eczema Returned
What Questions Might My Healthcare Provider Ask To Diagnose Eczema
The conversation with your healthcare provider will need to cover a lot of information. Be sure to be specific about your symptoms.
- Where is your eczema located?
- What have you used to try to treat your eczema?
- What medical conditions do you have? Allergies? Asthma?
- Is there a history of eczema in your family?
- How long have you had symptoms of eczema?
- Do you take hot showers?
- Is there anything that makes your symptoms worse?
- Have you noticed that something triggers or worsens your eczema? Soaps? Detergents? Cigarette smoke?
- Is there so much itchiness that you have trouble sleeping? Working? Living your normal life?
What Are The Symptoms Of Dyshidrotic Eczema
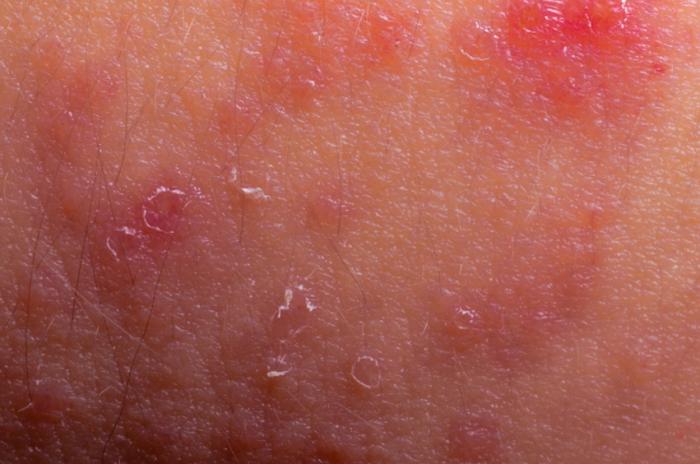
Often, the first symptom is sudden itching on the palms, the sides of your fingers, or the soles of the feet. Next, small fluid-filled blisters may start to appear. These cause more intense itching and pain. These blisters may get bigger. In some people, these symptoms can cause a lot of problems with daily activities. The blisters often last for a few weeks before they dry up and flake away.
Dyshidrotic eczema is more likely to affect the hands than the feet. In most cases, the symptoms happen on both hands or both feet.
Some people have symptoms in frequent episodes. The episodes may happen every month or so for months or years. Over time, this may cause chronic hand dermatitis and lead to more symptoms, such as:
- Reddened, hard skin
- Color changes in your nails
Recommended Reading: How To Deal With Eczema
How Is Psoriasis Diagnosed And Treated
Psoriasis often has a typical appearance that a primary care doctor can recognize, but it can be confused with other skin diseases , so a dermatologist is often the best doctor to diagnose it. The treatment of psoriasis usually depends on how much skin is affected, how bad the disease is , or the location . Treatments range from creams and ointments applied to the affected areas to ultraviolet light therapy to drugs . Many people who have psoriasis also have serious health conditions such as diabetes, heart disease, and depression. Some people with psoriasis also have an inflammatory condition which affects their joints, called psoriatic arthritis.
Psoriatic arthritis has many of the same symptoms as other types of arthritis, so a rheumatologist is often the best doctor to diagnose it. The treatment of psoriatic arthritis usually involves the use of drugs .
Psoriatic disease may be treated with drugs or a combination of drugs and creams or ointments.
Having More Than One Immune Problem
Unfortunately, some people have more than one kind of problem with their immune system. For example, people with one kind of autoimmune disease have an increased chance of getting another kind of autoimmune disease.
The same is true for people with atopic types of immune problems, who often have more than one kind. And some people with primary immune system problems have problems with autoimmune-related diseases.
Additionally, some treatments used for atopic immune disease and for autoimmune problems are immunosuppressants. That means that your immune system may not fight off certain infections as well as normal while you are taking them.
Don’t Miss: How To Stop Eczema Inflammation
How Common Is Eczema
Eczema affects up to 15 million Americans. Infants are prone to eczema and 10% to 20% will have it. However, nearly half outgrow the condition or have significant improvement as they get older.
Eczema affects males and females equally and is more common in people who have a personal or family history of asthma, environmental allergies and/or food allergies.
How Soon Will We See New Eczema Treatments
Guttman-Yasskys study shows that abnormalities in the skin and the immune system in people with atopic dermatitis can be reversed by drugs that target just IL-4 and IL-13.
As a result of this new research, in November, the Food and Drug Administration granted dupilumab a breakthrough therapy designation. This designation may speed up the FDAs approval of the drug as a treatment for moderate-to-severe AD in adults.
Guttman-Yassky noted that its difficult to say how long phase III, or late stage, studies will take to complete. However, she said, We will probably see new drugs available to treat atopic dermatitis in the next few years.
Current treatments for AD include topical moisturizers, creams, soaps, and steroid ointments. Sunlight and even ultraviolet light therapy may also help.
Dr. Daniel Aires, director of dermatology at the University of Kansas Hospital, gave his thumbs-up to the new study. Aires told Healthline, The new drug appears to help normalize the atopic molecular signature Extremely severe disease can require systemic treatment, but these often bring risk of serious side effects. Dupilumab may be an important new modality for treating these patients. Longer term studies and aftermarket evaluation will be needed to assess longer term safety issues.
Also Check: Best Shampoo For Eczema Itchy Scalp
How Are These Autoimmune Diseases Diagnosed
Because conditions such as lupus and scleroderma have symptoms that can resemble many other diseases, they can be difficult to diagnose initially. Lupus, for instance, can have symptoms that include fatigue and fever. Symptoms of scleroderma can include heartburn.
When you notice the first symptomsgenerally some form of skin rash that doesnt go away or that worsens over timeyou may seek treatment from a primary care doctor or dermatologist. An examination with a doctor can include discussion of symptoms, personal medical history and family history, as well as blood and other laboratory tests . The patient may then consult with a rheumatologist, who will have more experience working with the internal symptoms of the disease. Over time and depending on his or her symptoms, a patient may work with either a dermatologist or a rheumatologist, or both.
Whats The Difference Between Dermatitis And Psoriasis
Psoriasis and dermatitis can appear similar. Both cause patches of red skin. However, in psoriasis, the scales are thick and the edges of those scales are well-defined.
Discuss with your healthcare provider your questions about which type of skin condition you have. You can have more than one skin condition at a time. Treatments for one may not work for the other.
Also Check: Does Coffee Make Eczema Worse
Are Autoimmune Diseases Linked
An accurate medical history often grants doctors insights into a specific case or problem. Many conditions and diseases, including autoimmune diseases, have a genetic component. Atopic dermatitis appears to be one of these conditions. And considering that 25 percent of people who suffer from one autoimmune disorder end up having another, its also a condition worth mentioning to all of your doctors not just your dermatologist or PCP.5 An entirely different diagnosis might come easier to you or someone you love because you did.
Eczema And Autoimmune Disease
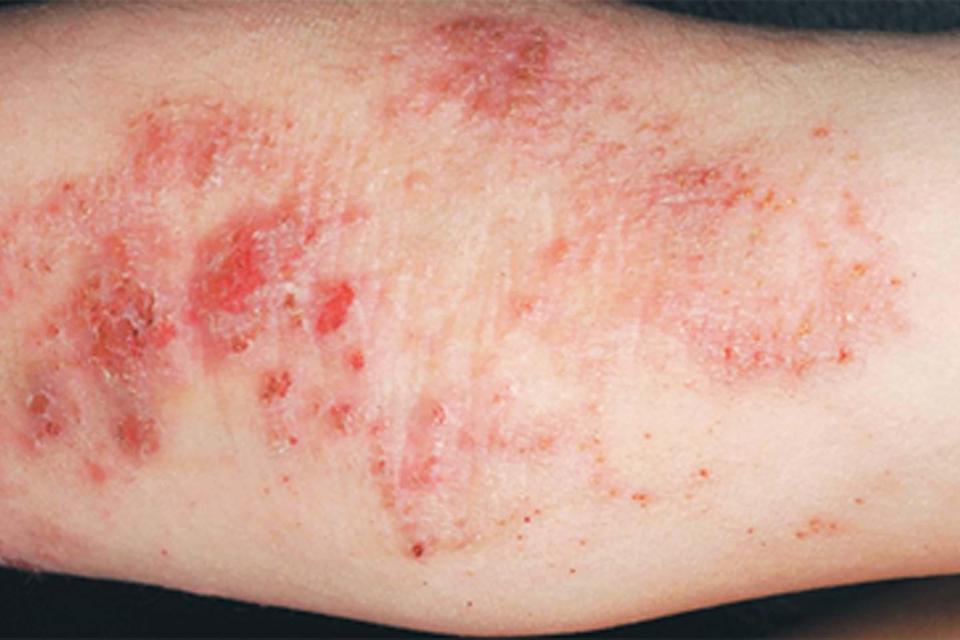
Its becoming more widely accepted that eczema, including discoid eczema, isnt just associated with various autoimmune diseases, but counts as one itself. It is characterised by inflammation, by damage to an organ , and by an inappropriately reactive immune system response.
So, in conclusion, although not everyone would acknowledge it as such, it does seem that discoid eczema, as a chronic inflammatory skin condition, is autoimmune in nature. It cant be cured, but can be managed, and the severity and frequency of flares reduced.
How Do You Get Rid Of Discoid Eczema?
Also Check: Best Treatment For Severe Eczema
How Is Eczema Diagnosed What Tests Are Done
Your healthcare provider will take a close look at your skin. They will look for classic signs of eczema such as a redness and dryness. They will ask about the symptoms youre experiencing.
Usually your healthcare provider will be able to diagnose eczema based on examining your skin. However, when there is doubt, they may perform the following tests:
- An allergy skin test.
- Blood tests to check for causes of the rash that might be unrelated to dermatitis.
- A skin biopsy to distinguish one type of dermatitis from another.
What Are Some Of The Autoimmune Diseases That Affect The Skin
When a persons immune system starts fighting against the cells its supposed to protect, it can lead to autoimmune diseases, several of which affect the skin and internal organs. In most of these skin-involved diseases, symptoms can vary greatly from person to person. Two of the most common such conditions are lupus and scleroderma.
- Lupus: A disease called lupus leads to a wide variety of symptoms, many of which can resemble other skin diseases. When it affects the skin, the condition is known as cutaneous lupus . It can come in many form most commonly, patients will see a butterfly-shaped rash, often on the face. When it spreads beyond the skin, its known as systemic lupus erythematosus , and the inflammation can affect the joints, the kidneys and other organs.
- Scleroderma: Like lupus, scleroderma can affect the skin, or it can become systemic. In this case, the immune system produces too much collagen, causing the skin to tighten and become tough and hard. When scleroderma is localized, or mainly affecting the skin, it can either be morphea, which manifests as oval patches, or linear, which shows up as streaks of hard patches. When scleroderma is systemic, it can develop slowly or quickly, affecting internal organs such as the lungs, heart and kidneys.
Don’t Miss: What To Do When You Have Eczema On Your Face
Connection Between Allergic Diseases And Autoimmune Diseases
- Date:
- Children’s Hospital and Regional Medical Center of Seattle
- Summary:
- A new study identifies a connection between allergic diseases such as atopic dermatitis, also known as eczema, and autoimmune diseases.
A new study by researchers at Childrens and the University of Washington identifies a connection between allergic diseases such as atopic dermatitis, also known as eczema, and autoimmune diseases. The study was published in the April 1 edition of Nature Immunology.
Approximately 75 percent of autoimmune diseases occur in women, most frequently during the childbearing years. These diseases also comprise a significant portion of chronic childhood disorders. Autoimmune disease refers to a group of more than 80 serious, chronic illnesses including diseases of the nervous, gastrointestinal, and endocrine systems as well as skin and other connective tissues, eyes, blood, and blood vessel. In all of these diseases, the underlying problem is similarthe bodys immune system becomes misdirected, attacking the very organs it was designed to protect.
Our study implies that allergic and inflammatory diseases may actually trigger autoimmune diseases by relaxing the controls that normally eliminate newly produced, self-reactive B cells. This is important because many autoimmune diseases are caused by self-reactive antibodies produced by such B cells said Dr. David Rawlings lead researcher and section head of Immunology at Childrens Hospital and the UW.
Story Source:
What About The Impact Of Eczema
The impact of eczema/allergies on individuals and families in Australia is often misunderstood, lacking in support and vastly underrated. Skin conditions, primarily eczema, are rated in the top 5 non fatal burden of diseases according to the World Health Organisation. This means that the impact on quality of life is significant. It affects people physically, financially, socially and psychologically.
Many individuals and their families are experiencing social isolation, anxiety, confusion and deteriorating health due to the lack of social support services specifically targeting those with complex and chronic allergic/skin diseases.
All our information about eczema has been reviewed by The Australasian College of Dermatologists.
You May Like: Eczema Itching All Over Body
What Can I Expect If Ive Been Diagnosed With Eczema
Nearly half of children with eczema will outgrow the condition or experience great improvement by the time they reach puberty. Others will continue to have some form of the disease. For adults with eczema, the disease can be generally well-managed with good skin care and treatment, although flare-ups of symptoms can occur throughout life.
What Makes Yale Medicines Approach To Treating These Autoimmune Diseases Unique
At Yale Medicine, we get together to discuss complicated cases to try to give the patients an interdisciplinary approach to their care, says Dr. Ramachandran. Theres definitely an advantage to have everyone on the same page,” she says.
Yale Medicine dermatologists also receive many referrals from doctors throughout the region.
“Through referrals, we see some of the more complicated cases, Dr. Ramachandran says. The doctors here truly care about their patients and try to come up with the best possible treatment regimens, working together to help patients with more challenging conditions.
Recommended Reading: Ringworm Vs Eczema In Toddlers
Association Between Ad And Celiac Disease
Prevalence of celiac disease in AD and controls was reported in four studies . Meta-analysis showed a higher prevalence of celiac disease in AD compared to controls. The synthesized OR was 1.98 with high heterogeneity . Only one cohort reported an increased incidence of celiac disease in AD, with a RR of 1.41 .
Talk With Others Who Understand

On MyEczemaTeam, the social network for people with eczema and their loved ones, more than 41,000 members come together to ask questions, give advice, and share their stories with others who understand life with eczema.
Are you living with eczema? Share your experience in the comments below, or start a conversation by posting on your Activities page.
Don’t Miss: Cortizone 10 Eczema Side Effects