Who Might Get Contact Dermatitis
Irritant reactions can occur after a single exposure or after repeated exposures over time, whereas it takes multiple exposures to the same chemical to develop an allergy. People who work in certain professions have a higher risk of developing contact dermatitis. You might repeatedly encounter irritating chemicals or allergens in these professions:
- Construction workers.
What Causes A Rash In Rheumatoid Arthritis
Eczema, Sweet’s syndrome, and pyoderma gangrenosum are all related to autoimmune problems. Both Sweets syndrome and pyoderma gangrenosum are neutrophilic dermatoses, inflammatory skin conditions related to an overload of a type of white blood cell called neutrophils. Neutrophils naturally produce an inflammatory response to infection. In an autoimmune condition, the skin may be attacked as foreign by the immune system, leading to neutrophils overwhelming the skin and causing inflammation as if the skin was infected.
While the precise cause of eczema is not known, it is generally considered to be an autoimmune response that causes inflammation of the skin. Other autoimmune conditions besides RA have been associated with eczema, including Crohns disease and ulcerative colitis.
Rheumatoid vasculitis is caused by inflammation of both small- and medium-sized blood vessels, often as part of an RA flare-up. It usually occurs in people who have had severe RA for more than 10 years. Certain factors play a part in those who are at higher risk for this complication. Most people who develop rheumatoid vasculitis have a high rheumatoid factor in their blood and many smoke cigarettes.
Palmar erythema, reddening in the palms, has a wide variety of causes. When someone with RA experiences red palms, however, it is most likely to be as a result of an autoimmune response. It can also be caused by medication taken to treat RA.
Eczema Or Herpes: How Can You Tell The Difference
Its often easy to distinguish between eczema and herpes because of their distinctly different symptoms. While herpes triggers defined blisters that burst and scab over, usually around the mouth or genitals, eczema causes rough, dry rashes in other areas of the body.
To distinguish between herpes and severe eczema that has produced open sores, consider the symptoms that occurred before the sores appeared and the location of the sores.
You May Like: Pediatric Dermatologist Specializing In Eczema
The 8 Types Of Rash To Be Aware Of
1. COVID Digits
The skin changes are known as chilblains and were relatively rare before Covid-19 because they are typically seen during cold spells and in people who are likely to have problems with circulation in the fingers or toes
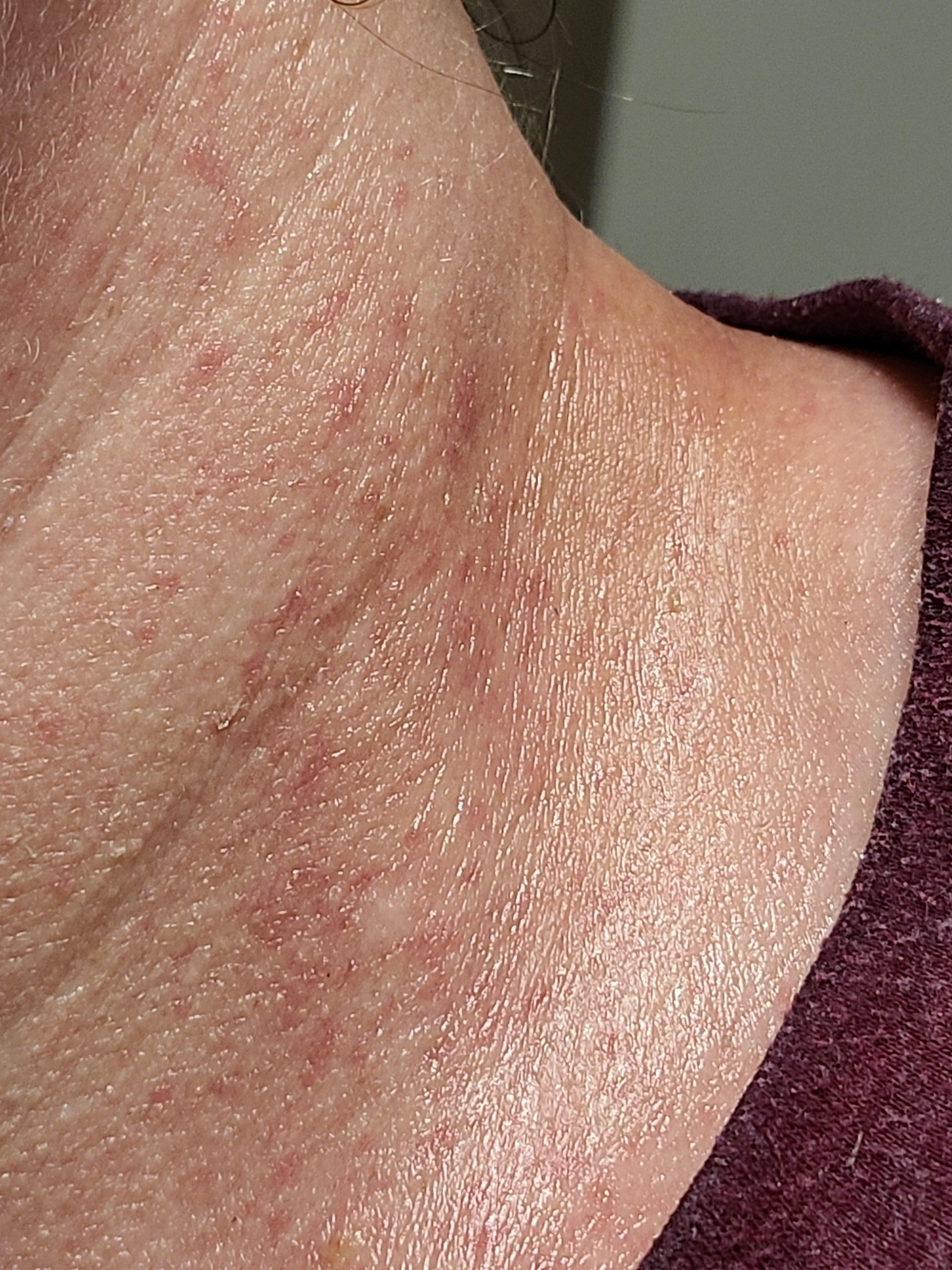
2. Neck & exposed chest eczema
This rash appears on the neck and on the anterior part of the chest at sites exposed to sunlight. It is usually quite pink and is very itchy.
3. Oral
Lips may feel sore and can become dry and scaly as they recover. Soreness inside the mouth can also occur.
4. Papular and vesicular
This rash appears as red and bumpy areas which may occur anywhere on the body, such as the elbows and knees as well as the back of the hands and feet. It can resemble bad prickly heat.
5. Pityriasis rosea
Pityriasis rosea is thought to be viral in origin, although never proven. It usually affects young individuals. More reports of this pattern during the pandemic have been reported which first present with an initial large herald patch, followed a few days later by multiple smaller patches on the torso or proximal limbs. It can last several months before clearing.
6. Purpuric
This pattern is easily recognisable as it presents with multiple deep red or purplish spots. It can cause bruise-like patches.
7. Urticarial
8. Viral exanthem
This is a common pattern seen in viral infections with a symmetrical rash comprising numerous reddish blotches or bumps over the body.
What Are The At
There some treatments you can do at home, but you should only do them with instructions and permission from your healthcare provider:
- Ultraviolet light. Ultraviolet A or B light waves can help your skin.
- Wet wrap therapy. This therapy increases moisture in your skin.
- Bleach baths. The amount of bleach is diluted. You shouldnt do this more than twice a week. Check with your healthcare provider before you try this therapy.
There are some other treatments you can do at home with no supervision:
- Use moisturizer. Right after you shower or bathe, apply moisturizer to your skin. This helps keep your skin hydrated.
- Dont overheat. Keep your space at a cool temperature and avoid high humidity.
- Protect your skin. Stay away from anything that could irritate it. This includes rough clothing like wool.
- Take steps to keep your stress levels down. If you need to, see a therapist for counseling and a psychiatrist for medication.
- Bathe in lukewarm water. Be sure to use lukewarm water instead of hot. Take no more than one bath or shower per day.
- Use a mild soap. Use soap or cleanser that is unscented.
- Avoid scratching. Scratching at your dermatitis irritates it. You could break the skin, risking infection.
Your healthcare provider may prescribe one or more of the following medications:
You May Like: Best Topical Cream For Eczema
How Is Contact Dermatitis Diagnosed
Clinical examination can reveal clues to the underlying diagnosis of irritant or allergic contact dermatitis. A careful history can uncover clues as to the offending agent.
With either type of contact dermatitis, you can avoid the substance for a while to see if the rash goes away. If avoidance is not possible or not sustainable, further diagnostic testing may be indicated.
For suspected cases of allergic contact dermatitis, a series of tests called patch testing can identify the underlying cause of allergic contact dermatitis.
With a patch test, you wear adhesive patches on your skin. The patches contain chemicals known to commonly trigger allergic reactions. After 48 hours, your healthcare provider checks your skin for reactions. Youll see your provider again in another 48-96 hours for one last skin check.
There isnt a test for irritant contact dermatitis. Your healthcare provider may be able to determine whats causing the rash based on the types of irritants or chemicals youre exposed to regularly.
Natural Treatments At Home
Aside from moisturizing your skin, some natural treatments may help heal your skin.
Oatmeal baths are one type of natural treatment that can soothe the itchiness and discomfort of eczema rashes. Be sure to use lukewarm water and follow up with a moisturizer immediately after.
Theres some evidence that both probiotics and prebiotics may stabilize your microbiome to help treat inflammation. However, more research is needed to support this approach in eczema treatment.
Recommended Reading: Does Water Help With Eczema
What Other Questions Might My Healthcare Provider Ask To Diagnose Dermatitis
The conversation with your healthcare provider will need to cover a lot of information. Be sure to be specific about your symptoms.
- Where is your dermatitis located?
- What have you used to try to treat your dermatitis?
- What medical conditions do you have? Allergies? Asthma? Celiac disease?
- How long have you had symptoms of dermatitis?
- Do you take hot showers?
- Is there anything that makes your symptoms worse?
- Are you around chemicals?
- Have you noticed that something triggers or worsens your dermatitis? Soaps? Detergents? Cigarette smoke?
- Is there so much pain or itchiness that you have trouble sleeping? Working? Just living your normal life?
Use A Moisturizer On Your Skin Every Day
Moisturizers help keep your skin soft and flexible. They prevent skin cracks. A plain moisturizer is best. Avoid moisturizers with fragrances and a lot of extra ingredients. A good, cheap moisturizer is plain petroleum jelly . Use moisturizers that are more greasy than creamy because creams usually have more preservatives in them.
Regular use of a moisturizer can help prevent the dry skin that is common in winter.
Don’t Miss: How Do You Treat Eczema On Your Face
What Is The Prognosis For People With Contact Dermatitis
If youve reacted to an allergen or irritant, you will continue to do so every time youre exposed to it again. You can prevent flare-ups by avoiding that substance.
Most people who have occupational contact dermatitis can find ways to reduce exposure so they can continue their work without breaking out in a rash.
How Can I Deal With Eczema
You may need a moisturizer to control the dryness and itchiness. Some people need stronger medicines called corticosteroids. Steroid ointment or cream rubbed on skin can help calm the inflammation .
Your doctor might suggest you try an antihistamine, a medicine that’s either a pill to swallow or a liquid. It can help control the itching and help you sleep at night. If all that scratching leads to an infection, you may need an antibiotic. None of these eczema medicines will cure you forever, but they can help make your skin more comfortable and less red.
Here are some other important steps to take:
You May Like: Skinfix Eczema+ Foaming Oil Body Wash
Can You Have Eczema Without A Rash
Harsh chemicals can cause a rash in anyone, but people with eczema may be sensitive to mild irritants, such as wool and synthetic fabrics, detergents, soaps, perfumes, and cosmetics. Stress or anxiety can cause a flare-up, too. So can sweating, along with wetting and drying your skin a lot, such as when you wash your hands.
What Questions Should I Ask My Doctor
If youre experiencing signs of contact dermatitis, talk to your healthcare provider. You may want to ask:
- Why do I have a skin rash ?
- Should I get an allergy test?
- What steps can I take to prevent contact dermatitis?
- What are the best treatments for contact dermatitis?
- What are the best treatments for a painful or itchy skin rash?
- What over-the-counter cleansers and moisturizers do you recommend?
- What signs of complications should I look out for?
Contact dermatitis is uncomfortable and can be painful or itchy. Talk to your healthcare provider about how you can find out whats causing it, reduce your exposure and prevent reactions. You might develop contact dermatitis from working with irritants or chemicals. Ask your employer about how you can minimize rashes while remaining on the job.
Last reviewed by a Cleveland Clinic medical professional on 10/10/2019.
References
Read Also: What Is The New Drug For Eczema
Pruritus With No Rash
What is pruritus with no rash?
Pruritus means itch.
Itch is a very common symptom of skin disorders such as eczema, scabies, insect bites and hives. These skin disorders are characterised by the presence of a rash.
Some people will have pruritus without a skin disorder. These individuals are often referred to as having pruritus with no rash.
What causes pruritus with no rash?
Pruritus with no rash may be due to:
- Systemic disorders these are conditions that affect internal organs including:
- Kidney failure especially in individuals on dialysis
- Liver disease such as primary biliary cirrhosis
- Blood disorders such as iron deficiency, polycythaemia rubra vera, lymphoma and myeloma
- Hormonal dysfunction especially over- or under-active thyroid
- Infections such as HIV infection
- Advanced cancer.
What does pruritus with no rash look like?
The natural human response to itch is to scratch the skin. The act of scratching at the skin unfortunately causes more itch, which is then followed by more scratching and further itch. This vicious cycle is known as the itch-scratch cycle.
How Is Dermatitis Treated What Medications Are Used
The type of treatment depends on the type of dermatitis and its location. Step number one is to avoid whatever triggers the dermatitis. That may be stress, a chemical, tobacco smoke and/or a number of other irritants that cause or worsen your dermatitis. Step number two is to try remedies on your own. Step number three is medication prescribed by your healthcare provider.
Don’t Miss: How To Treat Eczema Symptoms
Watch Out For These Common Eczema Triggers
- Dry skin can easily become brittle, scaly, rough and tight.
- Chemical irritants are everyday products or substances that can cause your skin to burn and itch.
- Stress can cause a persons atopic dermatitis to flare or worsen.
- Hot/cold temps and sweating can lead to itchy skin or prickly heat symptoms can develop during the cold winter months.
- Infection from bacteria and viruses that live in your environment can lead to a flare.
- Allergens wreak havoc on our lives and come from everyday materials in the environment like seasonal pollen, dust mites, pet dander and mold.
- Hormones: Flares may happen, especially in women, when certain hormones in the body increase or decrease.
Conditions That Can Look Like Eczema But Arent
Evan Starkman Brunilda Nazario, MD
Eczema is the name for a group of conditions that can make your skin irritated, inflamed, and itchy. Your doctor may call it atopic dermatitis, which is also the most common type of eczema. Youâre more likely to get eczema when youâre a child, but adults can get it, too.
The symptoms you have and where they show up on your body vary from person to person. You might have one or more of these signs:
- Red patches on white skin
- Gray or violet-brown patches on dark skin
- Oozing or crusty skin from scratching
- Swelling
Several health problems can bring on similar symptoms, so itâs important to talk to your doctor, a dermatologist, or an allergist to find out whatâs going on with your skin. They might tell you that you have one of these conditions that looks like eczema but isnât:
Psoriasis. This long-term condition is partly due to your immune system attacking your skin by mistake. Both psoriasis and eczema can bring on symptoms like:
- Red, scaly patches
- Dry, cracked skin
- Itching
Eczema patches tend to be thinner than psoriasis patches. Another difference: Fluid can ooze from your skin with eczema.
Scabies. This contagious condition happens when tiny bugs called mites burrow into the top layer of your skin and lay eggs. You might have symptoms like bad itching and a rash that looks like pimples. Like eczema, you could also get scaly-looking patches.
Acne. This skin condition can take several forms, including:
Read Also: How To Treat Ear Eczema
What Is Dermatitis And What Does It Look Like
Dermatitis is a word used to describe a number of skin irritations and rashes caused by genetics, an overactive immune system, infections, allergies, irritating substances and more. Common symptoms include dry skin, redness and itchiness.
In the word dermatitis, derm means skin and itis means inflammation. The word as a whole means inflammation of the skin. The rashes range from mild to severe and can cause a variety of problems, depending on their cause.
Dermatitis causes no serious harm to your body. It is not contagious, and it does not mean that your skin is unclean or infected. There are treatment methods and medications that can manage your symptoms.
How Is Dermatitis Diagnosed
Your healthcare provider will take a close look at your skin. They will look for classic signs of dermatitis such as a rash, redness, scales, dryness and more. They will ask about the symptoms youre experiencing. Are you itchy? Does your skin feel like its burning? Is your skin dry? Have you come into contact with anything that might irritate your skin?
Recommended Reading: How To Get Rid Of Black Eczema Marks
What Are The Complications Of Contact Dermatitis
Allergic contact dermatitis is a Type IV hypersensitivity reaction, caused by a different immunologic mechanism than hives, angioedema, or anaphylaxis. However, very rarely, patients may have immunologic dysfunction which results in multiple types of concurrent hypersensitivity reactions. Thus, it is possible that people with contact dermatitis can develop hives and swelling after coming into contact with an allergen. Hives are red, raised, itchy skin welts. Angioedema is swelling deep under the skin.
Extremely rare, allergic contact dermatitis can overlap with a severe, life-threatening allergic reaction called anaphylaxis that can swell airways and close them. If you think you are experiencing anaphylaxis, call 911. Youll need an immediate epinephrine injection to counteract this allergic response. People with known allergies can carry an EpiPen®, a brand of injectable epinephrine.
What Causes The Inflammation

So, what causes your skin to break out in red, itchy patches? Experts arenât exactly sure. But research says things like health, genetics, environment, certain products, and lifestyle may act as triggers. But eczema affects different people in different ways, so the things that cause you to have flare-ups may not bother someone else.
Immune system. When you have eczema, your body has an immune system that reacts too much. It responds easily to something thatâs either inside your body such as genes or outside of it like an allergen or irritant. This reaction damages the skin barrier — the topmost layer of your skin that defends your body from bacteria and keeps it from losing too much moisture. Without this protection, your skin is more sensitive, dry, brittle, and prone to inflammation.
Genetics. Youâre more likely to have eczema if you have:
- Family or personal history of dermatitis.
- Food allergy
Research shows that youâre also more likely to have eczema if you have a gene mutation that makes your body less able to produce enough filaggrin. This is a type of protein that helps your body build a strong skin barrier. If youâre low on filaggrin, your skin may lose a lot of water and become dry. It can also expose your skin to viruses and bacteria and make it more prone to infection.
Thereâs no cure or supplement you can take to fix your filaggrin levels, but keeping your immune system healthy can help ward off skin problems.
They can include:
You May Like: When To See A Dermatologist For Eczema