Which Types Of Face Coverings Are The Most Eczema
Face coverings made from 100% cotton that can be washed regularly are probably the most eczema-friendly type of covering. Cloth ear loops are less likely to irritate the skin than elastic ones. Also consider coverings that tie around the back of the head. Mask headbands or hats with buttons are another option. With these, the elastic loops around the buttons rather than your ears. Neck gaiters, buffsor tube scarfs, which are basically a tube of material, might suit too if 100% cotton.
Make sure the covering fits snugly around your nose and mouth but isnt tight.
Avoid applying ointment emollients to the face shortly before you put on a covering, as they might make the face too hot.
Supplier suggestions:
- Spirit of Nature sells 100% cotton face masks.
- Etsy has lots of different types of face coverings for sale. Search for the type youre interested in.
- Handybands from Seasalt have been recommended to us by a Facebook follower. They can be used as face coverings as well as head bands. Organic cotton face masks are also available from Seasalt.
- There are lots of guides and video tutorials showing you how to make different types of face covering, for example: BBC, .
If you have severe facial eczema that is made worse by wearing a face covering, the Government has exemption badges and cards on its website that you can print out.
Dupixent For Chronic Rhinosinusitis With Nasal Polyps
Dupixent is approved to treat chronic rhinosinusitis with nasal polyps in adults. Its used when the condition is not well controlled by other treatments.
Dupixent is used as an add-on treatment in people with chronic rhinosinusitis with nasal polyps who are already taking another medication to treat it. Rhinosinusitis is when your sinus cavities swell and cause pain or pressure in your face, along with congestion. Rhinosinusitis becomes chronic when it lasts for 12 weeks or longer.
Nasal polyps are tissue growths in the nose that are noncancerous. People with chronic rhinosinusitis usually have an increased number of eosinophil cells in their nasal and sinus cavities. Eosinophils are immune system cells that increase swelling in the area.
Dupixent helps by reducing swelling in the area, which relieves symptoms of chronic rhinosinusitis with nasal polyps.
In clinical trials, Dupixent greatly decreased nasal and sinus symptoms caused by chronic rhinosinusitis. It also helped improve peoples sense of smell. Reduced ability to smell is a common side effect of nasal polyps.
After 24 weeks, people taking Dupixent experienced a 51% to 59% decrease in nasal congestion. In comparison, people taking a placebo experienced a 16% to 18% decrease in nasal congestion.
Egg Allergies And Vaccines
Some vaccines contain egg white proteins, which may be of concern for those with egg allergies. This is cause for concern only if the patient has a history of serious reactions from consuming eggs. In any event, all pediatricians follow protocols in place to make it possible to vaccinate all children, even those with egg allergies, without triggering a reaction.
What happens in the case of a proven allergy to eggs:
- Measles, mumps and rubella vaccine: no problems, even in those with severe allergies, so no precautions necessary.
- Flu: the doctor will choose a brand with the lowest dose of ovalbumin .
- Yellow fever: once again, the ovalbumin content is taken into account. Must be given in a specialist vaccination center.
- Rabies: in France, the rabies vaccine is cultivated on vero cells rather than eggs and can be given to allergic patients without any issues.
- Tick-borne encephalitis : the same precautions apply as with yellow fever.
If you decide against the doctors advice not to vaccinate your child, you are placing their life at risk.
ADVICE CATEGORIES
Recommended Reading: Start Of Eczema In Babies
How To Stay Safe
The best way to stay safe with eczema during the pandemic is to follow public health guidance to lower the risk of catching COVID-19:
- Continue your eczema medication as prescribed.
- Take steps to avoid and manage flares during the COVID-19 pandemic.
- Support your health by reviewing eczema care basics.
- Take steps to reduce stress, manage itching, and improve your sleep hygiene.
- Wash your hands regularly, avoid close contact with others, and socially distance where possible. You can rewash your hands with your usual emollient to protect the skin and use moisturizer after washing hands and when the skin feels dry, cracked, or sore.
- When washing your hands, wash with soap and water for at least 20 seconds.
- If soap and water are not available, use a hand sanitizer containing 60% alcohol. Apply moisturizer to your hands once hand sanitizer is dry if it is causing our eczema to worsen.
- Wear a face mask in public settings and where social distancing is not possible. Once you are fully vaccinated, wearing a face mask is optional.
- Avoid crowded situations.
- Practice self-monitoring.
- Avoid contact with people who are unwell.
- If someone in your home becomes unwell, follow medical guidance and isolation advice to reduce the risk of spreading the virus in your home.
Bottom Line: Staying Healthy With Psoriasis

A 2010 review of vaccinations in people with diseases caused by the immune system, including psoriasis, found that people with these diseases are often not getting all the vaccinations they need. The review noted that people with diseases like psoriasis may be at increased risk for diseases prevented by vaccinations.
In most cases, vaccinations can be given safely to people with psoriasis and the benefits outweigh the risks, said Moore.
A Koebner reaction is best avoided by avoiding any skin trauma, including vaccination, while you have an active psoriasis flare. You should be able to receive killed virus immunizations as long as you are not in the middle of a flare. Live vaccines need to be used with more caution, so talk to your doctor about them. In most cases, vaccines and psoriasis can go together safely.
Recommended Reading: Soap For Sensitive Skin Eczema
Tuberculosis Vaccine Might Help Reduce Eczema In Infants
by Murdoch Children’s Research Institute
A century-old tuberculosis vaccine could help reduce the incidence of eczema in high-risk infants due to its beneficial off-target effects, according to a new MCRI-led allergy study.
Bacille Calmette-Guérin , a vaccine used in Australia until the 1980s to prevent tuberculosis, had been tested in a trial to see if it can reduce the rate of allergies and infections in infants.
The initial findings, which were published in the journal Allergy, showed that the BCG vaccine had a modest beneficial effect in preventing eczema in high-risk infants. At this stage, however, the authors noted there is insufficient evidence to recommend neonatal BCG vaccination for all infants to prevent eczema in the first year of life.
The benefit was greater in infants with two atopic parents, meaning those who have hay fever, asthma or eczema. In these infants, a single dose of BCG soon after birth reduced the incidence of eczema by 25%.
Chief investigators Professor Nigel Curtis, Dr. Laure Pittet, and Dr. Nicole Messina undertook this research as part of the Melbourne Infant Study: BCG for Allergy and Infection Reduction .
MIS BAIR is a randomized controlled trial to assess the effect of neonatal BCG vaccination on clinical allergy and infection outcomes over the first five years of life.
The study is based on the idea that BCG vaccination stimulates the immune system so that it is better at fighting infections and less prone to allergies.
Explore further
Dupixent And Other Medications
Below is a list of medications that can interact with Dupixent. This list does not contain all drugs that may interact with Dupixent.
Before taking Dupixent, talk with your doctor and pharmacist. Tell them about all prescription, over-the-counter, and other drugs you take. Also tell them about any vitamins, herbs, and supplements you use. Sharing this information can help you avoid potential interactions.
If you have questions about drug interactions that may affect you, ask your doctor or pharmacist.
Live vaccines
Its important not to get any live vaccines while taking Dupixent. For live vaccines, youre injected with a small amount of a virus so your body can learn to fight it. Dupixent may weaken your immune system, so a live vaccine could make you sick.
Before starting Dupixent, talk to your doctor or pharmacist about any vaccines you may need. You should get any live vaccines you need before you start taking Dupixent.
Live vaccines you should avoid when taking Dupixent include:
- measles, mumps, rubella
- prickling or tingling feeling like pins and needles in your arms or legs
- fever
Don’t Miss: How To Treat Eczema On Your Face
Skin Reactions And Psoriasis: Tips To Avoid The Koebner Response
Any type of skin trauma can lead to formation of a psoriasis plaque, or Koebner reaction, in the area of the trauma. The Koebner response may occur in anyone with psoriasis. It may sometimes cause the first symptoms of psoriasis or other skin diseases, like lichen planus. Cuts, scratches, tattoos, and vaccinations are common triggers for this response, said Moore.
Other causes may include sunburn, poison ivy, or even a bug bite. These minor traumas can cause a psoriasis plaque to form at the site of trauma within one to two weeks of the injury. About 50 percent of people with psoriasis experience the Koebner response.
Vaccine Side Effects And Adverse Events
Corynebacterium diphtheriae, SEM x3750, artificially coloredCopyright Dennis Kunkel Microscopy, Inc.
A vaccine is a medical product. Vaccines, though they are designed to protect from disease, can cause side effects, just as any medication can.
Most side effects from vaccination are mild, such as soreness, swelling, or redness at the injection site. Some vaccines are associated with fever, rash, and achiness. Serious side effects are rare, but may include seizure or life-threatening allergic reaction.
A possible side effect resulting from a vaccination is known as an adverse event.
Each year, American babies receive more than 10 million vaccinations. During the first year of life, a significant number of babies suffer serious, life-threatening illnesses and medical events, such as Sudden Infant Death Syndrome . Additionally, it is during the first year that congenital conditions may become evident. Therefore, due to chance alone, many babies will experience a medical event in close proximity to a vaccination. This does not mean, though, that the event is in fact related to the immunization. The challenge is to determine when a medical event is directly related to a vaccination.
The Food and Drug and Administration and the Centers for Disease Control and Prevention have set up systems to monitor and analyze reported adverse events and to determine whether they are likely related to vaccination.
Don’t Miss: Essential Oils That Help With Eczema
Complications Of Eczema And Covid
To help prevent the spread of COVID-19, regularly washing hands with soap and water is recommended. However, frequently washing hands with soap can cause problems for people with eczema, worsening symptoms.
To help lessen the effect of handwashing and sanitizing gel on your eczema symptoms, you can apply the following tips:
- Once you have thoroughly washed your hands with soap and water, you can rewash them with your usual emollient to protect the skin.
- Use moisturizer after washing hands and when the skin feels dry, cracked, or sore.
- Pat your hands dry rather than rubbing them to avoid irritation.
- Put an ointment or moisturizer on your hands and cover them with clean cotton gloves overnight to rehydrate hands if they are sore and dry.
- If you need to use a sanitizing gel, apply your usual emollient once the gel is dry.
- If you are using cleaning products, disinfectants, or washing dishes, wear gloves to protect your skin and avoid further irritation.
- If your eczema worsens or you suspect your skin is infected, then contact your healthcare provider for advice.
Stress can also exacerbate eczema symptoms through its effects on immune response and skin barrier function. It’s essential to be aware that the impact of COVID-19 on your life could be increasing your stress levels. Therefore, to help prevent eczema flare-ups, you can practice techniques to reduce stress levels.
Tips for managing stress and eczema include:
Who Needs An Additional Covid
Currently, CDC is recommending that moderately to severely immunocompromised people receive an additional dose. This includes people who have:
- Been receiving active cancer treatment for tumors or cancers of the blood
- Received an organ transplant and are taking medicine to suppress the immune system
- Received a stem cell transplant within the last 2 years or are taking medicine to suppress the immune system
- Moderate or severe primary immunodeficiency
- Advanced or untreated HIV infection
- Active treatment with high-dose corticosteroids or other drugs that may suppress your immune response
Weve included additional guidance below about specific medications you may be taking for your eczema.
Meet the Ecz-perts
- Andrew F. Alexis, MD, MPH, is the chair of the department of dermatology at Mount Sinai Morningside and Mount Sinai West. He is also professor of dermatology at the Icahn School of Medicine at Mount Sinai and Director of the Skin of Color Center.
- Amy Paller, MD, is chair of the department of dermatology at Northwestern University Feinberg School of Medicine and pediatric dermatologist at the Ann and Robert H Lurie Childrens Hospital of Chicago.
- Jonathan M. Spergel, MD, PhD, is director of the Center for Pediatric Eosinophilic Disease and professor of pediatrics at the Perelman School of Medicine at the University of Pennsylvania.
Don’t Miss: What Causes Eczema In Toddlers
Vaccines Are Not Contraindicated
Atopic eczema should have no bearing on your decision to vaccinate your child. Your child should follow the recommended vaccination schedule to ensure they are fully protected. Both mandatory and optional vaccines are recommended to help prevent serious diseases. Vaccinating children with eczema can only help, especially given the fact that they are more vulnerable to infections.
Questions And Answers With A Brief Rationale True & False And / Or Multiple
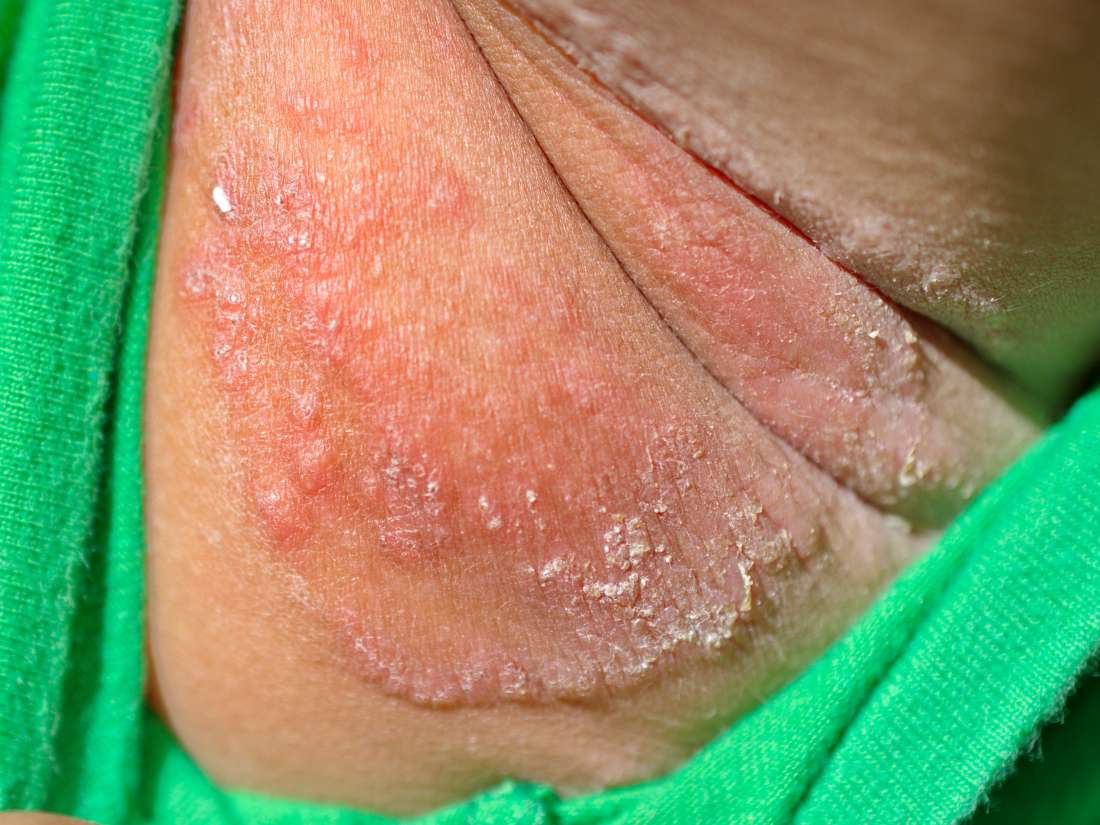
- 1
Given the patient’s presentation, what is the most likely diagnosis?
- a)
-
none of the above.
Correct Answers = C
There is a possibility this rash is drug induced by the patient’s home medication of risperidone however, the patient has been stable on risperidone for several years and less likely to be the cause of a drug-induced erythema multiforme.
Risperidone-induced erythema multiforme have been reported in literature search, however it presents as a mild, self-limiting reaction needing only supportive treatment such as use of topical steroids, fluid and electrolyte replacement, and pain/analgesia management.
The patient denied the addition of any new medications including soaps or detergents.
There is a high probability that the rash is Moderna COVID-19 vaccine induced, given the temporal relationship between vaccination administration and rash development. Within 10 days from the first dose, the patient developed a self-resolving mild rash that subsequently expanded into bullous lesions following four days after second vaccination completed.
This is an FDA reportable adverse reaction through MedWatch, given COVID-19 vaccine is a new entity developed during the pandemic to be administered under Emergency Use Authorization .
- 1
Severe/refractory: Immunomodulator agents for example, rituximab, IV immunoglobulin
Don’t Miss: How To Get Eczema Off Your Face
What Is Atopic Dermatitis
Atopic dermatitis is a chronic skin disorder. It causes dry, itchy, scaly patches on the skin, often on the face and scalp in babies. Its most common in infants or very young children. Most will show signs of the condition in the first year of life. Symptoms may last until the teens or adulthood. It rarely starts in adulthood. Atopic dermatitis is not contagious.
Atopic dermatitis tends to run in families. This suggests a genetic link. Its also associated with asthma and allergies. These are immune hypersensitivity disorders.
Treatment for this condition is aimed at calming the skin inflammation, decreasing the itching, and preventing infections. Good skin care and medicine to control itching and infection are used.
Atopic dermatitis is often called eczema.
What You Need to Know about Eczema | FAQ
Is There A Preventive Treatment That Can Be Taken Just Before Or After The Vaccine
The answer is “no”.
Pain or fever is not that common, so there is no point in taking any medication without any symptoms.
To conclude
An atopic predisposition with its share of food, respiratory, or contact allergies does not represent a contraindication to vaccination
To date, even if vaccination decreases the risk of transmission, protective measures are still necessary.
ADVICE CATEGORIES
Recommended Reading: Eczema Treatment For Babies Home Remedies
How Can I Mitigate The Effects Of Frequent Hand
We recommend that people with eczema follow the government guidance to wash hands with soap and water, rather than an emollient soap substitute, as much as practically possible. Soap is considered to be more effective than emollient at breaking the lipid envelope surrounding coronavirus particles, and removing the virus from the skin.
Frequent washing of hands with soap can, however, cause problems for people with eczema, including dry skin and hand eczema. It is very important people find ways of managing dry skin and hand eczema that may be caused or worsened by frequent washing with soap.
Strategies for this include:
If you feel you need to use sanitising gel , apply your usual emollient afterwards to minimise any irritant effect.
In public places where you cant avoid touching surfaces, try not to touch your nose, eyes or mouth because the virus gets in through mucous membranes.
How To Inject Dupixent
Dupixent is given as a subcutaneous injection . You should take Dupixent according to your doctor or pharmacists instructions.
For your first dose of Dupixent for treating eczema or asthma, you will typically get two injections in two different areas of your body. Usually, the first dose is given at your doctors office. After the first dose, you only need one dose every other week.
For treating chronic rhinosinusitis with nasal polyps, treatment starts and continues with one dose every other week.
Your doctor can teach you how to give yourself injections, or you can go to their office for injections. For children, its recommended that the doctor gives the injections in their office.
Dupixent syringes should be stored in the refrigerator at 36 to 46°F . Before using Dupixent, let the medication reach room temperature, then wait 45 minutes before taking it. Never heat the syringe or put it into sunlight.
Dupixent can be injected into your thigh, upper arm, or stomach. Dupixent shouldnt be injected within 2 inches of your belly button. Use a different area each time you inject, and dont inject into skin thats bruised or scarred.
Be sure to dispose of the used syringe properly in a sharps container.
Don’t Miss: How Do You Treat Eczema On Your Face