How Is Baby Eczema Treated
Treatment varies for baby eczema based on what caused your childs symptoms to flare up and the severity of their symptoms. Treatment for baby eczema could include:
- Eliminating or avoiding triggers: Avoid scented or fragranced soaps, lotions or detergents. These things can cause eczema to flare. Your provider might test your babys skin to identify if theyre allergic to certain things in their environment that they contact regularly. If youre able to identify what causes your babys eczema triggers, avoiding those causes helps your babys skin heal and prevents future eczema flare-ups.
- Using topical corticosteroids: These are prescription-strength ointments that you rub on your babys skin like a lotion. Corticosteroids help reduce itching and swelling. For mild eczema, apply topical OTC 1% hydrocortisone ointment twice a day for no longer than two weeks. For moderate to severe eczema, your healthcare provider may recommend prescription-strength steroid ointments. Any steroid ointment should not be applied for longer than two weeks since it may lead to discoloration by thinning out the skin.
- Applying moisturizer to your babys skin: Keeping your babys skin hydrated can reduce symptoms, soothe their skin, remove discomfort and prevent flare-ups. Choose moisturizers designed for babies and products that dont contain fragrances. The best time to apply moisturizers to your babys skin is after a bath and a couple of times throughout the day when their skin appears dry.
Card11 Gene Mutation May Drive Eczema
Dr. Milner and colleagues singled out eight people from four families that had mutations in the CARD11 gene. This gene encodes the instructions for producing the CARD11 protein, which has a key role in lymphocyte receptor signaling.
Some of the people in the study who had these genetic mutations also had other health problems, such as other infections, while some did not.
This suggested to the researchers that CARD11 mutations can lead to eczema without simultaneously causing comorbidities, as is often the case with immune system conditions.
In an attempt to understand precisely the mechanism through which CARD11 mutations lead to atopic dermatitis, the researchers conducted a series of experiments and studied cell cultures to examine the effect of the mutations on the CARD11 protein.
In each of the four families, the researchers found a different mutation that affected a separate area of the CARD11 protein. However, all of the mutations affected T cell signaling in a similar way.
T cells are a white blood cell type, which are essential for the bodys immune response to infections.
Specifically, the researchers were able to detect two cell-signaling pathways that were disrupted by the mutations. These signaling pathways were no longer activated properly as result of the mutations.
Normally, one of these pathways is partially activated by glutamine, which is an amino acid that is, a building block of protein with key roles in immunity, brain function, and digestion.
What Genes Are Linked To Eczema
According to The Journal of Pediatrics, studies have found that certain inheritable genetic mutations may play a role in the development of eczema. These genes control the immune system as well as proteins that help keep the skin barrier healthy and functioning properly.
Currently, two theories explain how the genes FLG and CARD1 may lead to eczema. Other genes may also be involved. Much more research is needed to clarify the role of these genes and other gene mutations on the development of atopic dermatitis. Atopic dermatitis likely involves multiple genes, with environmental factors affecting the severity of a persons condition.
Don’t Miss: National Eczema Association Seal Of Acceptance
The Skin Biome In Atopic Eczema
The skin of people diagnosed with atopic dermatitis differs from those without it. They have lower microbial diversity, fewer Streptococcus bacteria, and more Staphylococcus aureus, an opportunistic microbe that causes infections.
Interestingly, the skin microbiome of atopic eczema patients varies depending on whether they have skin lesions when swabbed. People with active skin inflammation have significantly disturbed microbial skin communities, especially an overgrowth of S. aureus where the rashes occur.
However, even in the absence of a flare-up, patients with eczema still have disturbed skin microbiomes with more S. aureus than healthy people. Just like in the gut, these findings highlight the importance of microbial diversity in human health.
Whats The Difference Between Dermatitis And Psoriasis
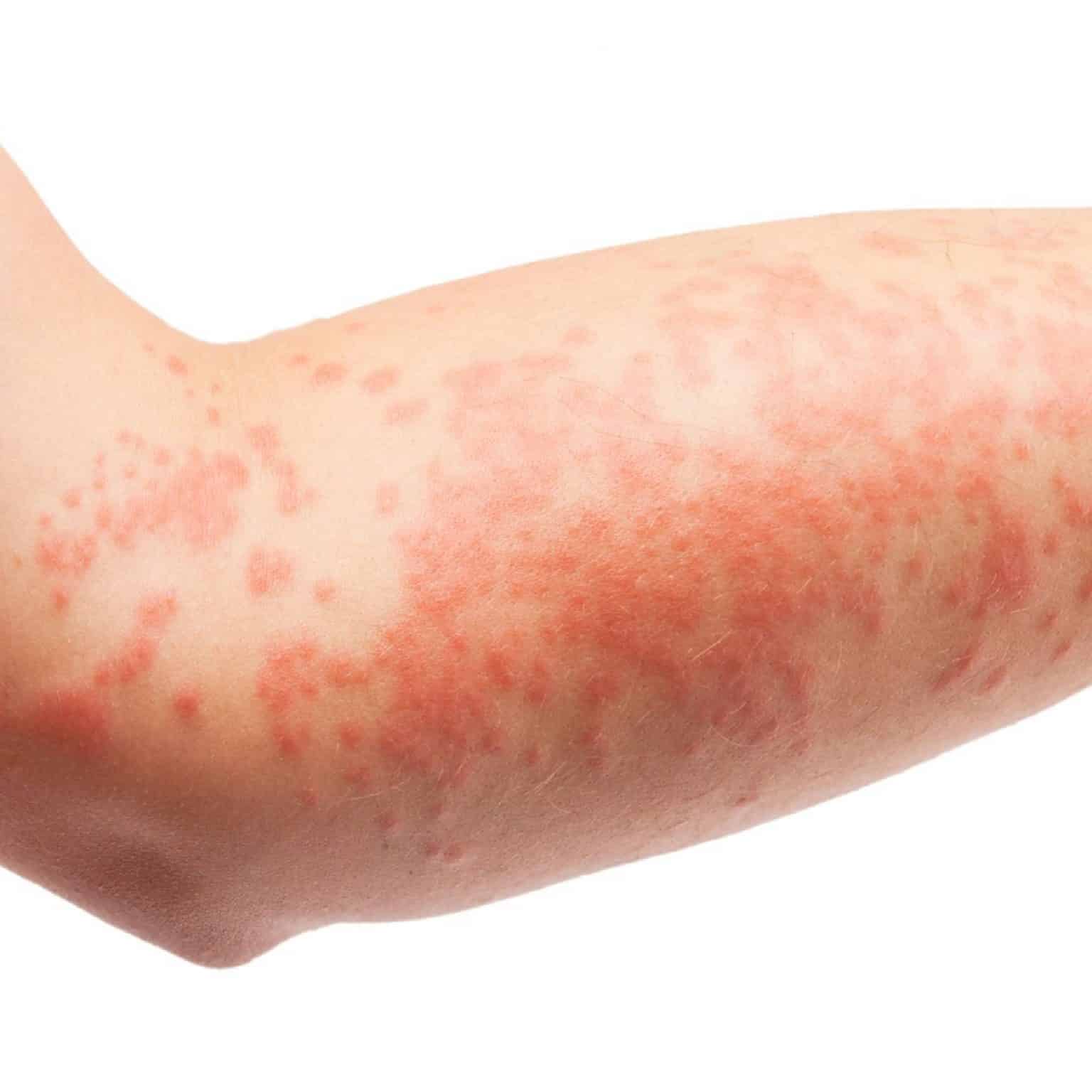
Psoriasis and dermatitis can appear similar. Both cause patches of red skin. However, in psoriasis, the scales are thick and the edges of those scales are well-defined.
Discuss with your healthcare provider your questions about which type of skin condition you have. You can have more than one skin condition at a time. Treatments for one may not work for the other.
Don’t Miss: What Can I Use For Eczema On My Baby
What Causes Eczema Flare Ups
One of the difficult parts of managing eczema is identifying the environmental triggers that cause flare-ups. For a lot of people, simple allergy tests with their dermatologist will do the job.
But for some people, these triggers can be difficult to determine. You move, get a new job, get older, all of which can alter your environment and bring you into contact with things that may trigger eczema. Its an ongoing effort, and sometimes you wont know something is a trigger until the eczema flares up.
Some environmental elements that can make the symptoms of eczema worse include :
- Contact with allergens
- Trimming or covering fingernails
- Avoiding skin irritants
When it comes to finding soothing techniques to help with troublesome triggers, there may be a genetic element. If youre struggling to identify your eczema triggers, your genes might provide some clues to solve the mystery. These triggers differ from person to person and can include certain fragrances, metals or fabrics .
While there isnt a completely clear cause of eczema, genetics seems to play a major role. Whats more, the genetics of eczema, asthma, hay fever, and food allergies are very similar. This means that if you have one, youre more likely to have the others .
Environmental Factors That Are Known To Affect Atopic Dermatitis
There are a wide variety of environmental factors that may trigger your atopic dermatitis symptoms. Some of the common triggers are:
- Irritants: soaps, perfumes, detergents, and shampoos
- Allergens: dry or wet weather, dust, mites, pollen, and molds
- Food allergies: dairy, peanuts, soy, wheat, etc.
- Fabrics: wool, synthetic fibers, etc.
- Hormones: some women notice more severe atopic dermatitis during their period or pregnancy
Recommended Reading: Body Lotion For Eczema Prone Skin
Genetic Testing For Eczema
There is no common test that can tell you whether you have eczema, except a physical examination by the physician who can confirm the disease.
In todays advanced world people are very keen to know how likely they or their child have a chance of developing eczema. Thats very well justified because knowing whether someone has inherited a mutant copy of FLG is important clinical information. Because if a mutation is present in a new-born, then early intervention with proper care and standard moisturizers could help to prevent or delay the onset of atopic eczema which is most common in children.
Currently, there are few DNA testing Companies like 23andMe, AncestryDNA, etc. Which can be used to predict your or your childs risk of developing eczema based on the DNA. Remember these are just predictions and not an exact verdict and conditions in your environment still play a critical role.
Other Genes associated with Eczema In another new study led by Mariana L Stevens, published in the journal Nature Communications, researchers found and delineated the two variations of the gene KIF3A that is said to be responsible for the impairment of the skin barrier that regulates water loss resulting to the onset of Eczema.
What Is It Like Living With Eczema
Many people live with eczema . As many as 15 million Americans may have this skin condition. Living with it can be challenging.
There may be times when your eczema disappears. This is known as a remission period. Other times you may have a flare-up, which is when it gets worse. The goal of treatment is to prevent such flare-ups, preventing your symptoms from getting worse. Be sure to avoid triggers, moisturize, take your medicine and do anything else your healthcare provider recommends.
Recommended Reading: Why Does Eczema Only Affect Certain Areas
The Atopic March And Birth Cohort Studies
Several prospective longitudinal studies have provided evidence for the atopic march from eczema to the development of allergic rhinitis and asthma . A systematic review of the risk of asthma development in children with eczema during the first four years of life reported a pooled odds ratio of 2.14 for asthma , which is lower than originally estimated, but still supports the hypothesis of the atopic march from eczema to asthma.
Given the natural history of eczema, birth cohorts provide an optimum study design to evaluate eczema development and progression in early life. Many birth cohort studies designed to examine asthma and allergic diseases have been implemented in both European countries and the US. Although almost all of these studies aim to evaluate environmental contributions to asthma and allergic diseases, only a few of these cohorts are designed to evaluate both environment and genetics concurrently, which is important given the well-documented genetic contributions to these complex diseases. The birth cohorts discussed in this review are summarized in the Table.
Can Eczema Be Prevented
There is currently no cure for eczema, but there are ways you can prevent flare-ups and treat symptoms. In infants, it is important to treat eczema as early as possible. Applying topical moisturizers routinely and avoiding irritants such as harsh soaps and detergents, dyes and fragrances, itchy fabrics, dust, pollen, and extreme hot or cold temperatures are effective ways to prevent eczema flares.
Avoiding or removing known inflammatory foods from your diet may also help prevent eczema symptoms. These foods may include eggs, dairy, wheat, corn, and soy. It is important to talk with your doctor about identifying food allergies. While many people with atopic dermatitis have food allergies, the role of food in exacerbating the skin condition remains unclear.
Genetic tests and screening may be an option for people with a family history of eczema or atopic diseases. Blood and saliva tests can help identify mutations in the CARD11, FLG, or MTHFR genes. Talk with your doctor about genetic testing options.
Your dermatologist may also prescribe a steroid cream or other topical treatments to help control itching and repair the skin barrier. Antibiotic creams can help to fight bacterial infections from open sores or cracks. It is best to avoid scratching or rubbing the affected area of skin to help prevent infections or worsening of eczema symptoms. A newer medicine called dupilumab can help control more severe forms of the disease.
Read more about treatments for eczema here.
Don’t Miss: Eczema Around Eyes And Mouth
Environmental Factors And The Hygiene Hypothesis
Environmental factors have been implicated in allergic disease, including eczema. The role of environmental tobacco smoke in allergic disease has been an area of extensive study. There is a clear association between lower airway disease and ETS exposures , but the association between ETS and eczema is not as consistent. Studies have reported associations between eczema and the number of cigarettes smoked in the home with urine cotinine , and maternal smoking during pregnancy . A 2008 study of 261 infant mother pairs evaluated the association of eczema at age two with cord and maternal serum cotinine levels . The authors observed that the risk of eczema increased with maternal and cord blood cotinine levels in a dose-dependent manner . Other studies have reported no associations between ETS and eczema . There is some evidence that ETS exposure may impact skin barrier function. In one study, investigators measured TEWL on the cheek area of 100 volunteers that were either active, passive, or non-smokers . The authors observed a lower TEWL measurements in non-smokers compared to both active and passive smokers, independent of age and sun exposure . Thus, ETS exposure may have a role in the breakdown of the skin barrier that is associated with eczema development.
The Role Of The Environmental Risk Factors In The Pathogenesis And Clinical Outcome Of Atopic Dermatitis
Domenico Bonamonte
Abstract
Atopic dermatitis prevalence is rising worldwide. Literature data suggest the incidence of AD in developing countries is gradually getting close to that of developed ones, in which AD affects 20% of the paediatric population. Such an increment, associated with significant variations in prevalence among the various countries, underlines the importance of environmental factors in the disease onset. Among these, great importance is given to hygiene, intestinal microbiota, exposure to bacterial endotoxins, outdoor living with contact to animals, atmospheric pollution, weather, and diet. Genetic as well as immunologic factors concur with the environmental ones. Only the systematical study of all these elements can best elucidate AD epidemiology.
1. Introduction
Atopic dermatitis is the most common inflammatory disease in childhood and poses a great number of problems related to health and quality of life of patients . An increase in the prevalence of AD is seen all over the world and accordingly causes much general interest in the identification of potential risks and protective environmental factors.
Thus, analysis of these data seems to reasonably suggest an important role of environmental factors in the pathogenic mechanism of AD together with genetic and immunologic ones.
2. Environmental Factors
Table 1 shows the risk factors that influence AD, some of them with a preventive effect, others aggravating.
2.1. Climate
2.2. Urban vs Rural Life
Also Check: Does Chlorine Make Eczema Worse
What Can We Do To Prevent An Eczema Flare Up Even If We Are Genetically Prone
- Moisturize and hydrate your skin well
- Use a humidifier at home when using heaters during winter to prevent dehydration of your skin
- Manage your stress well by practicing relaxation techniques such as yoga and meditation
- Identify and avoid irritants which can trigger a flare such as wool, certain chemicals and other irritants
- Avoid using harsh soaps and detergents
Box 1 Epidemiological Observations About Asthma And Allergy
There are tenfold regional differences in the prevalence of asthma and atopic diseases
Allergic disease is more common in clean westernized environments
Asthma and atopy are less common in the children of animal farmers
Asthma and atopy are less common in younger siblings
Asthma and atopy are less common in households with dogs as pets
Recommended Reading: How To Know If Eczema Is Healing
The Nature Of Allergens
The respiratory organs deal with a multitude of airborne particles, yet only a few of these particles from a limited number of sources consistently produce allergic reactions. Disease-associated allergens are usually soluble proteins. Most allergens have an enzymatic function in their natural state, but this is also true of most proteins, and a consistent activity shared by allergens has not been identified. Most allergens form particles of dimensions that allow them to become airborne and to penetrate the respiratory tree. Only a limited range of particle sizes are respirable, and are able to reach into the lung rather than being deposited in the nose and throat. It is still unclear whether the physical facts of allergens ubiquity, respirability and solubility are sufficient to explain why they induce disease.
The allergens that most commonly produce reactions in susceptible individuals are known as major allergens. Allergens are named according to their source and the order in which they were discovered. Major allergens from the house dust mite Dermatophagoides pteronyssinus, for example, include Der p I and Der p II. Other important major allergens are Fel d I from the cat Felis domesticus,Bet v I from pollen of the birch tree and Phl p I and Phl p V from the pollen of timothy grass Phleum pratense. Many other grass pollens, such as rye grass , have allergens that are similar to those of Phleum pratense .
Introduction To Eczema And Genetics
Who here is familiar with the Atopic March? No, its not an obscure piece of music written by an even more obscure composer. Its the unsightly parade of eczema, asthma, and allergies, an event you couldnt be paid enough to attend. The intro to this terrible tune, eczema , plays across the entire lifespan from infancy through adulthood. As you might expect, this would make a genetic connection highly likely, but is eczema hereditary?
If you live with eczema, then you know how tough it can be to soothe your symptoms on a daily basis. Eczema is a condition that causes symptoms like itching and red, inflamed skin. People often wonder if eczema is contagious, because it can turn into what looks like growths on the skin, but its just something in the environment interacting with a persons skin and a dysfunctional immune response.
Eczema is also rather common. Up to 1 in 3 children experience it, usually in the first year of life, but it can last into adulthood. It might vanish for years and then abruptly flare up, because it can be caused by a wide variety of things. Its less common in adults, but still affects millions .
Unsurprisingly, a major player when it comes to eczema is genetics. Genes involved in eczema may influence :
- Skin barrier function
- Immune response
Recommended Reading: Why Do I Have Eczema On My Elbows
Flg Gene Mutation And Fads1 Fads2 And Fads3 Gene Polymorphism Analysis
DNA will be extracted from the buffy coat of the umbilical artery by the Puregene DNA isolation kit . Genotyping will be performed using iPLEX Gold Chemistry and matrix-assisted laser desorption ionisation-time of flight mass spectrometry, with methods to detect allelic differences, as previously described. In brief, locations containing certain SNPs will be amplified by PCR using specific primers. After deactivation by alkaline phosphatase, single base elongation will be performed. In this reaction, primary elongation is performed in accordance to the print order. After salt ion removal by ion switch and elongation reaction, the specimen will be transferred to silicone chip and covered with 3-hydroxypicolinic acid. The differences from specific alleles will be measured by MALDI-TOF. Allele recognition from SNPs will be performed by Mass ARRAY Typer V.4.0.5 . We plan to assess 18 SNPs for the FADS1, FADS2 and FADS3 genes and five SNPs for the FLG gene.,
SNPs for FADS genes were selected based on three criteria: the SNP has been studied in previous publications the SNP candidates in consideration are SNPs that have already been shown to be associated with LC-PUFA status or AD and minor allele frequency is > 10%.