What Is Dermatitis Herpetiformis
Dermatitis herpetiformis is an extremely itchy rash consisting of bumps and blisters. The rash is chronic, which means it continues over a long period. Dermatitis herpetiformis usually begins in people age 20 and older. Children can sometimes be affected. It is seen in both men and women. The cause is unknown. It is thought to be an autoimmune disorder. Dermatitis herpetiformis is also linked to gluten sensitivity in the small bowel. Symptoms of dermatitis herpetiformis tend to come and go. Symptoms include: extremely itchy bumps or blisters, most often on the elbows, knees, back, and buttocks. The rash is usually the same size and shape on both sides. The rash can look like eczema. Some patients may have scratch marks instead of blisters. A strict gluten-free diet will be recommended to help control the disease. Sticking to this diet may eliminate the need for medications and prevent later complications. The disease may be well-controlled with treatment. Without treatment, there may be a significant risk of intestinal cancer.
Is Eczema Caused By A Weak Immune System
Eczema isnt believed to be the result of a weak immune system.
But researchers dont know exactly what causes eczema, according to the National Eczema Association . Experts think genes and a variety of triggers are contributing factors.
When you have eczema, the skin barrier that would normally keep out allergens, bacteria, and other germs isnt working as it should. Instead of keeping unwanted elements out, breaks in your skins barrier allow them to seep in, according to .
Once allergens or other substances are inside your body, your immune system reacts.
It sends out an army of white blood cells that release chemicals and other substances to destroy the invaders. These substances are responsible for your skins inflammation.
Think about when you cut yourself or skin a knee. Your immune system responds to the injury by producing redness, itching, swelling, and pain at the site. This is a good thing proof that your immune system is strong and healthy.
What Foods Should I Eat Or Avoid To Reduce My Risk Of Eczema
The connection between eczema and food allergies is unclear. If you have food allergies, then one of the reasons why you must avoid that food is that it may cause or worsen dermatitis. Examples of common allergies include peanuts, dairy, eggs, sugar, alcohol and gluten. Pay attention to what you eat. If your eczema flares up after you eat a certain food, then you might have an allergy to it.
If you dont have a food allergy then there are no foods, including chicken, that will cause or worsen your eczema.
You May Like: How To Keep Eczema Under Control
Whats The Root Cause Of Eczema
Researchers dont know exactly what causes eczema. Its likely that there isnt one single cause, but rather a combination of factors that lead to eczema.
If you have eczema, its possible youve inherited genes that make your skin more susceptible to irritation. Chances are, one or more of your immediate family members also has eczema, allergies, or asthma.
Differences in your skins barrier is another possible cause of eczema.
Some people with eczema have mutations in the gene that codes for a protein called filaggrin. This protein typically helps the skin barrier stay healthy and strong, and a mutation in this gene is often found in people with eczema, according to 2009 research .
When the skin barrier isnt functioning as it should, allergens and germs seep in and moisture seeps out. Dried-out skin is more likely to react strongly to substances in your environment that are typically harmless.
A number of triggers can also set off eczema symptoms. Everyones triggers are different, but common ones may include:
- soaps, detergents, and other chemical irritants
- allergens such as dust mites, pet dander, pollen, and mold
- allergies to foods such as dairy or wheat
Symptoms Of Atopic Dermatitis
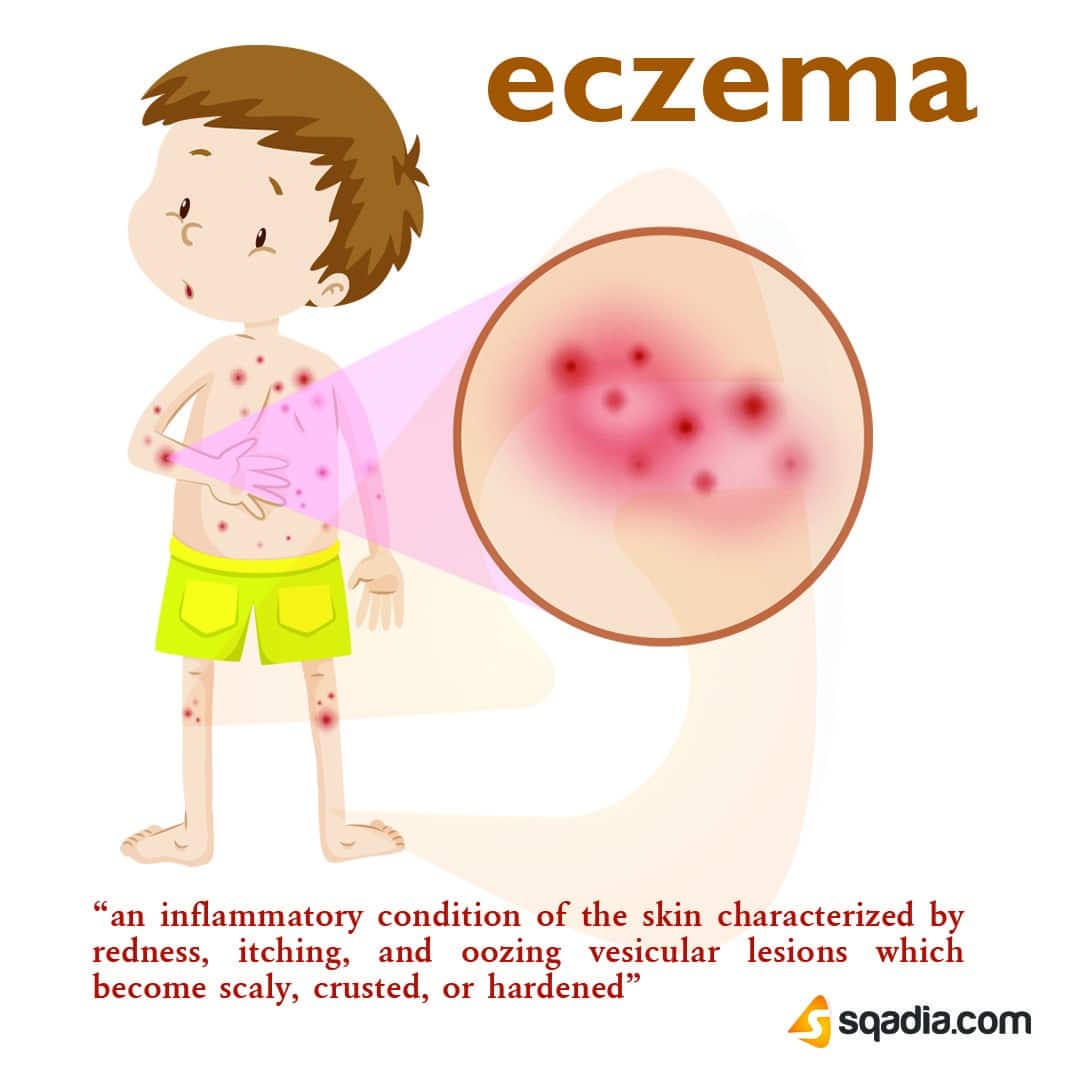
When you have active atopic dermatitis, your immune system releases a variety of substances that trigger itching, sensitize the skin to external irritants and interfere with the skins healthy barrier function and its natural microbiome . These factors lead to chronic inflammation of the skin that produces the dry, itchy, scaly patches that are atopic dermatitis signature. Frequent scratching then causes those spots to discolor, harden and thicken, a process known as lichenification.
There are two main issues people with atopic dermatitis have to address, says Dr. Murase. One is that they dont have an intact skin barrier, so its harder for them to make the oils that they need to coat and protect their skin. The second is that they create a lot of inflammation and that causes their skin to get red and angry. In people with darker skin, the angry lesions may appear brown, gray or purple.
To counter the inflammation and bring quick relief from the itching and rash in the short term, doctors often prescribe topical corticosteroids for mild flares and prednisone, an oral corticosteroid and immunosuppressant that regulates the bodys immune response, for moderate to severe flares.
You have to treat the endogenous inflammation thats causing the skin condition to erupt, says Dr. Murase, referring to the systemic inflammation that results from the bodys flawed immune response.
Recommended Reading: Which Soap Is Best For Eczema
What Is Atopic Dermatitis
Atopic dermatitis , or atopic eczema, is the most common type of eczema in the United States. It’s usually diagnosed in children, making its first appearance between the ages of 3 to 6 months. Itâs less common for AD to appear for the first time in adulthood, but it does happen. When adults have AD , it usually appears on the backs of the knees, crooks of the elbows, back of the neck, and face .
How Common Is Eczema
Eczema affects up to 15 million Americans. Infants are prone to eczema and 10% to 20% will have it. However, nearly half outgrow the condition or have significant improvement as they get older.
Eczema affects males and females equally and is more common in people who have a personal or family history of asthma, environmental allergies and/or food allergies.
Also Check: What Do You Do For Eczema
What Is Eczema What Does It Look And Feel Like
Eczema is a condition that causes your skin to become dry, red, itchy and bumpy. Its one of many types of dermatitis. Eczema damages the skin barrier function . This loss of barrier function makes your skin more sensitive and more prone to infection and dryness.
Eczema doesnt harm your body. It doesnt mean that your skin is dirty or infected, and its not contagious. There are treatments that can help manage your symptoms.
In the word dermatitis, derm means skin and itis means inflammation. The word as a whole means inflammation of the skin. Eczema originates from the Greek word ekzein which means to boil over or break out.
Connection Between Allergic Diseases And Autoimmune Diseases
- Date:
- Childrens Hospital and Regional Medical Center of Seattle
- Summary:
- A new study identifies a connection between allergic diseases such as atopic dermatitis, also known as eczema, and autoimmune diseases.
A new study by researchers at Childrens and the University of Washington identifies a connection between allergic diseases such as atopic dermatitis, also known as eczema, and autoimmune diseases. The study was published in the April 1 edition of Nature Immunology.
Approximately 75 percent of autoimmune diseases occur in women, most frequently during the childbearing years. These diseases also comprise a significant portion of chronic childhood disorders. Autoimmune disease refers to a group of more than 80 serious, chronic illnesses including diseases of the nervous, gastrointestinal, and endocrine systems as well as skin and other connective tissues, eyes, blood, and blood vessel. In all of these diseases, the underlying problem is similarthe bodys immune system becomes misdirected, attacking the very organs it was designed to protect.
Our study implies that allergic and inflammatory diseases may actually trigger autoimmune diseases by relaxing the controls that normally eliminate newly produced, self-reactive B cells. This is important because many autoimmune diseases are caused by self-reactive antibodies produced by such B cells said Dr. David Rawlings lead researcher and section head of Immunology at Childrens Hospital and the UW.
Story Source:
You May Like: What Is The Treatment For Eczema
Other Causes Of And Risk Factors For Eczema
Its likely that a combination of factors precipitate the development of eczema. For example, age seems to play a role. Babies and children are more likely to develop eczema than adults are. Cold, dry climates may also affect the development of eczema.
Many people experience eczema in conjunction with food allergies, allergic rhinitis, and asthma. This combination is called the atopic march or atopic triad.
Common allergens that can make eczema worse include:
- Cleaning products
- Weather changes
An allergist or dermatologist can test you to see if youre sensitive to specific ingredients that might be contributing to your eczema symptoms. Wearing protective gloves, avoiding irritating fabrics, and following treatment advice from your health care providers can help you gain control over your eczema.
What Causes Discoid Eczema
As with any type of eczema, what causes a flare of discoid can vary from person to person. For many people the condition is associated with atopic dermatitis, as well as other conditions such as hay fever and asthma, with which it can co-exist. Flares can be triggered by things like:
- Injury to the skin
- Environmental conditions
- Certain medications
- Contact with irritants
However, even knowing what can trigger or exacerbate a flare doesnt explain the root reason why some people get discoid eczema and others dont. It doesnt seem to have any genetic component, but it is a chronic condition that can persist for months or years once someone has suffered one attack of discoid eczema, theyre likely to have more.
Don’t Miss: Oatmeal Bath For Eczema Recipe
Is Eczema An Autoimmune Disease Spoiler Alert: Nope
According to the National Institutes of Health , autoimmune disease occurs when the immune system makes a mistake and attacks the bodys own cells, tissues or organs and unfortunately the problem seems to be getting more common. Immunity is our bodys defense system: when our immune system is working properly, it fights off infections and cancers, whereas autoimmunity is when this process goes wrong.
In a recent study done by the American College of Rheumatology, researchers demonstrated that the most common biomarkers of autoimmunity have been increasing in the U.S. population since the late 1980s, especially among young people.
What Is Discoid Eczema
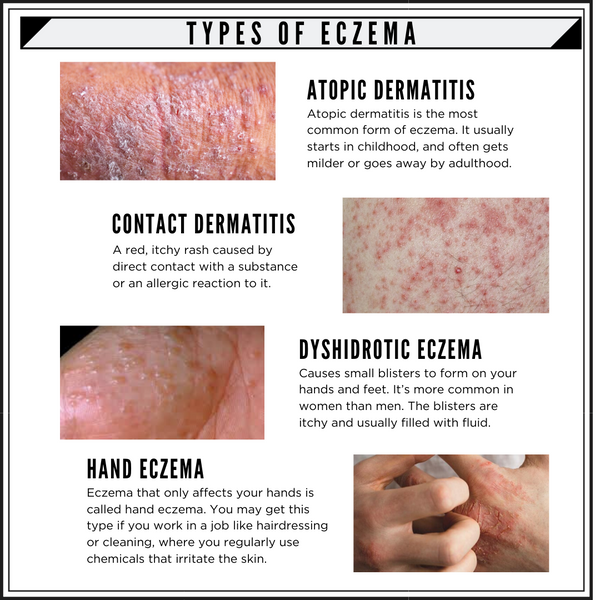
Discoid eczema is a type of eczema or dermatitis. Also known as nummular eczema, the condition is notable for the way its lesions form circular or oval discs. Starting off as bumpy or blistered spots, the eczema grows outward in rings, with the outer edge often being intensely itchy or inflamed, often weeping then crusting over. The condition can affect adults of any age, but is slightly more commonly found in men over 55. Discoid eczema isnt infectious, although it can get infected.
You May Like: Best Store Bought Eczema Cream
What Questions Might My Healthcare Provider Ask To Diagnose Eczema
The conversation with your healthcare provider will need to cover a lot of information. Be sure to be specific about your symptoms.
- Where is your eczema located?
- What have you used to try to treat your eczema?
- What medical conditions do you have? Allergies? Asthma?
- Is there a history of eczema in your family?
- How long have you had symptoms of eczema?
- Do you take hot showers?
- Is there anything that makes your symptoms worse?
- Have you noticed that something triggers or worsens your eczema? Soaps? Detergents? Cigarette smoke?
- Is there so much itchiness that you have trouble sleeping? Working? Living your normal life?
If I Have Eczema Should I Take Drugs To Suppress My Immune System
My opinion differs to many medical professionals but most would agree that eczema is not an autoimmune disease. Some people with eczema also have an autoimmune disease but that is not the rule for everyone with eczema.
I have worked with eczema patients who have had overactive immune systems, which were overactive because they were eating foods they were highly sensitive to and they had nutritional deficiencies.
Long-term use of topical steroids can also cause problems, and often topical steroid withdrawal is involved and causes the eczema to be stubborn and hard to treat.
Their calcium levels were also very low and this caused insomnia . Once these patients changed their diets and took Skin Friend supplements their immune systems gradually normalised. This took about 8 months.
For those with eczema and immune system issues, I find they need to be healthy long-term. For other eczema sufferers who have no autoimmune issues and no topical withdrawal symptoms, their eczema clears a lot faster.
Don’t Miss: How To Treat Eczema In Ear Canal
Is Eczema An Autoimmune Disease
Eczema is an inflammatory condition that affects 10-20% of the population. Its characterized by rough, red, and incredibly itchy patches. Due to a damaged skin barrier, those with eczema suffer from chronically dry skin. When discussing eczema, a common question arises: is eczema an autoimmune disease? Lets find out!
Please keep in mind that although these tips can relieve eczema, we are in no way medical professionals. If youre experiencing severe eczema symptoms like an infection, it is best to seek medical advice immediately.
What is Eczema?
Eczema is an umbrella term for a group of inflammatory skin conditions. There are several different types of eczema such as discoid eczema, dyshidrotic eczema, and the most common type, atopic dermatitis.
Typically developing in childhood or infancy, eczema can be triggered by a number of allergens and environmental changes, including dust mites, pet fur, sweat, stress, contact with irritants such as rough fabrics or soaps, and even food allergies. While itchy patches usually develop on the hands, back, and creases of elbows and knees, it can develop in other places as well.
Eczema Immune Response
So, is Eczema an Autoimmune Disorder?
There is a significant body of research that suggests eczema is an autoimmune disease, similar to psoriasis, lupus and many other immune disorders.
Treating Eczema as an Autoimmune Disease
Stop Scratching
Change up your Diet
Use Natural Skincare Products
Wet or Dry Wrap Therapy
References:
Eczema And Autoimmune Disorders
The researchers looked for 8,112 Danish diagnosed with eczema between 1/Jan/1997 and 31/Dec/2012.12 Significantly associated with atopic dermatitis are:
- Alopecia areata
- Ulcerative colitis
- Rheumatoid arthritis
Atopic dermatitis was also shown to be more closely associated with having three or fewer autoimmune illnesses than with having one or two comorbidities. A smoking history was substantially related to having one or more autoimmune diseases.
According to the researchers, atopic dermatitis and autoimmune diseases may share genetic risk loci and common environmental triggers due to the common occurrence of autoimmune comorbidities and the association of high living standards and urban lifestyles with atopic dermatitis found in previous studies.
Don’t Miss: What Can I Use For Eczema On My Baby
Treating Atopic Eczema With Monoclonal Antibodies
In 2014 a team of researchers at Mt. Sinai in New York showed that dupilumab, a monoclonal antibody, helped resolve symptoms in people whose AD did not get better when they applied topical medications or avoided triggers. Dupilumab blocks specific cytokines involved in allergic inflammation and in 2017 was approved by the FDA for treatment of moderate to severe AD. By 2020, however, reports began popping up of patients developing joint and tendon pain and tenderness after being treated with dupilumab. Study of this and other monoclonal antibodies for treatment of atopic eczema continues.
Atopic Dermatitis Associated With Higher Risk For Autoimmune Disorders
Patients with atopic dermatitis have an increased risk for multiple autoimmune disorders, particularly those who have more severe AD, according to findings from a study published in the Journal of Allergy and Clinical Immunology.
Researchers analyzed data from the Oxford-Royal College of General Practitioners Research and Surveillance Centre primary care database to assess the co-occurrence of common autoimmune disorders and determine whether the risk for autoimmune disease is related to AD severity.
All children and adults with newly diagnosed AD from 2009 through 2018 were eligible for inclusion. The following common autoimmune disorders were included in the analysis: Crohn disease, ulcerative colitis, celiac disease, pernicious anemia, type 1 diabetes, autoimmune hypothyroidism, Grave disease, psoriatic arthritis, rheumatoid arthritis, ankylosing spondylitis, systemic lupus erythematosus, Sjögren syndrome, vitiligo, alopecia areata, and multiple sclerosis.
A total of 173,709 patients with AD were matched with 694,836 control participants . The control participants had at least 1 year of follow-up to minimize the risk for a nonrecorded AD diagnosis.
At their diagnosis, patients with AD had a higher prevalence of autoimmune disorders compared with the control participants . Adjusted analysis demonstrated an association between AD and new onset of any autoimmune disorder .
Reference
Recommended Reading: How To Make Eczema Scars Go Away
Association Between Ad And Celiac Disease
Prevalence of celiac disease in AD and controls was reported in four studies . Meta-analysis showed a higher prevalence of celiac disease in AD compared to controls. The synthesized OR was 1.98 with high heterogeneity . Only one cohort reported an increased incidence of celiac disease in AD, with a RR of 1.41 .
Data Extraction And Quality Assessment

We extracted surname of the first author, publication year, country/region, study design, demographic characteristics in the case and control groups, assessment used for AD and autoimmune diseases, risk estimates with 95% CI and corresponding adjustments for confounders. The methodological quality of selected studies was evaluated using the NewcastleOttawa Scale , which comprised three main items including sample selection, comparability and exposure/outcome. Studies could be awarded a maximum of one star for each numbered item within the selection and exposure/outcome categories and a maximum of two stars for comparability category, with a score of 13, 46, and 79 represented as of low, intermediate, and high quality respectively. Two authors independently conducted quality assessments of the included studies. Discrepancies were discussed and resolved by the authors.
You May Like: Best Way To Treat Eczema On Feet