Who Gets Eczema Coxsackium
Eczema coxsackium most commonly affects preschool-age children with atopic dermatitis . It affects both boys and girls, and typically presents during late spring to early summer . There have been reported cases in adults .
Enteroviral infection can also localise to sites of epidermal barrier breakdown that are not caused by eczema. Reported cases of non-eczematous conditions prone to enteroviral infection include :
- Lacerations/scars
How Does My Child Get Hmfd
Coxsackie virus is spread by unwashed hands, and shed from an infected persons saliva, nasal mucous, and stool. The fluid inside the blistery rash has the virus too, but is a relatively minor contributor to contagiousness. Infants and toddlers spread this infection quickly because they like to touch/explore everything, frequently have their hands in their mouths, and are not yet able to wash their hands well enough to get rid of the germs. Parents and caretakers can get and spread the virus by not adequately washing their hands with soap and water after dirty diaper changes.
NOTE: coxsackie virus is not killed by hand sanitizer. SOAP & WATER must be used!
This Shouldn’t Have Happened
Thankfully, Huxley is instead on the mend with the rash disappearing quickly thanks to the second doctors instructions.
Teala wants to wait until her son is completely better before she tries to contact the first doctor again.
We have another appointment with the second doctor at the end of today and Im hoping we get good results, I will then contact the other service with what has happened tomorrow, she says.
I want to make sure my son is fine before I inform the other clinic.
I most certainly understand that every individual professional makes mistakes – but this shouldn’t have happened.
“I would love for other parents to go with their gut if they think its not right and get a second opinion.”
Telea wants to wait until Huxley returns to his normal, healthy self before she calls the doctor back. Source: Madeline Cox
Also Check: Eczema Therapy Daily Moisturizing Cream
What Causes Eczema Coxsackium
Coxsackievirus A6 and A16 are the most common causes of eczema coxsackium.
The reason why the enterovirus localises to sites with atopic dermatitis remains unclear. It is thought the mechanism is similar to eczema herpeticum, where afflicted patients appear to have impaired immunity to the virus and barrier dysfunction at the affected sites . This mechanism may explain how non-eczematous conditions such as Darier disease have also presented with a widespread viral infection that preferentially erupts at the sites of the skin disease .
What You Need To Know About Hand Foot And Mouth Disease
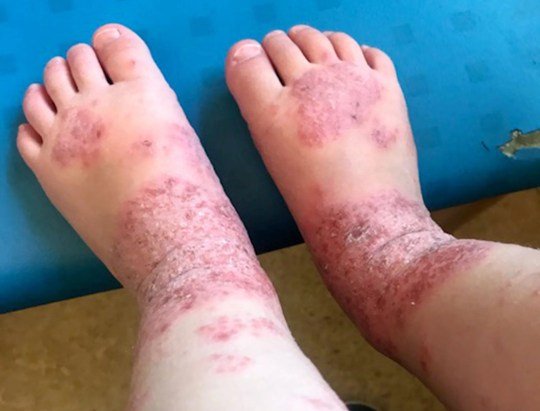
- Hand, foot and mouth disease infections are very common, second only to the common cold.
- It is most common in children under age ten.
- Children who contract hand, foot and mouth disease may display some or all of the following symptoms fever, mouth sores that turn into ulcers, rash on the soles of the feet and palms of the hand, sore throat, joint pain, headache
- Good handwashing and proper hygiene can prevent hand, foot and mouth disease.
- Treat the discomfort associated with hand, foot and mouth disease infections with paracetamol.
Recommended Reading: Eye Cream For Eye Eczema
My Baby Boy’s Eczema Was So Bad People Thought He Had Leprosy
“The barrier in the skin is often broken down due to eczema, especially with young children, meaning the virus will easily get into their system.
“I advise parents I see to keep their children away from those with cold sores or any virus from the herpes family.
“Eczema herpeticum is a medical emergency and anyone with these kinds of symptoms should seek medical help straight away.
“Parents should seek the help of a dermatologist and makes sure to check the child’s eyes as the top layer and cornea can be affected.
“A course of antiviral medication will help to clear up the infection.
“Parents and children should make sure to keep on top of hygiene, make sure they are on an eczema treatment plan to control flair ups and stay well rested and use anti-septic creams.”
We pay for your stories! Do you have a story for The Sun Online news team? Email us at or call 0207 782 4368. You can WhatsApp us on 07810 791 502. We pay for videos too. to upload yours
Hand Foot And Mouth Disease In Pregnancy
Although theres usually no risk to the pregnancy or baby, its best to avoid close contact with anyone who has hand, foot and mouth disease.
This is because:
- having a high temperature during the first 3 months of pregnancy can lead to miscarriage, although this is very rare
- getting hand, foot and mouth disease shortly before giving birth can mean your baby is born with a mild version of it
Speak to a GP or your midwife if you have been in contact with someone with hand, foot and mouth disease.
Page last reviewed: 12 February 2021 Next review due: 12 February 2024
Read Also: Is Eczema A Sign Of Pregnancy
Don’t Miss: Do I Need To See A Dermatologist For Eczema
Enhancing Healthcare Team Outcomes
Eczema herpeticum is considered a medical emergency and should be treated promptly with systemic antivirals, as misdiagnosis and delay in treatment can result in serious complications. An ophthalmologic evaluation is warranted in cases of EH involving the face and eyelids. A dermatology consult may be beneficial to confirm the diagnosis. Clinicians should be aware of the risk factors associated with EH, including severe or poorly controlled atopic dermatitis, food and environmental allergies, asthma, the onset of atopic dermatitis before age five, and history of S. aureus and molluscum contagiosum infections.
Patients with systemic symptoms or widespread involvement should be promptly referred to the Emergency Department. To improve patient outcomes and prevent morbidity and mortality, healthcare providers should have a high index of suspicion for EH in patients with a history of atopic dermatitis presenting with a sudden onset, vesicular, monomorphic rash in areas of pre-existing dermatitis.
Eczema Coxsackium And Unusual Cutaneous Findings In An Enterovirus Outbreak
This work was presented in preliminary form as a poster at the Society for Pediatric Dermatology Annual Meeting July 1114, 2012 Monterey, CA. It was presented as an abstract at the American Academy of Dermatology Annual Meeting March 2, 2013 Miami, FL.
FINANCIAL DISCLOSURE: Christine C. Ginocchio is a consultant, received payment for lectures, and has a grant/pending grant from bioMerieux. bioMerieux makes the enterovirus assay that was used in the diagnosis of enterovirus at North Shore-Long Island Jewish Health System Laboratories. The other authors have indicated they have no financial relationships relevant to this article to disclose.
Pediatrics
Erin F. Mathes, Vikash Oza, Ilona J. Frieden, Kelly M. Cordoro, Shigeo Yagi, Renee Howard, Leonard Kristal, Christine C. Ginocchio, Julie Schaffer, Sheilagh Maguiness, Susan Bayliss, Irene Lara-Corrales, Maria Teresa Garcia-Romero, Dan Kelly, Maria Salas, M. Steven Oberste, W. Allan Nix, Carol Glaser, Richard Antaya Eczema Coxsackium and Unusual Cutaneous Findings in an Enterovirus Outbreak. Pediatrics July 2013 132 : e149e157. 10.1542/peds.2012-3175
To characterize the atypical cutaneous presentations in the coxsackievirus A6 associated North American enterovirus outbreak of 20112012.
Also Check: What Can I Use For Eczema On My Baby
What Causes Hand Foot And Mouth Disease
Hand, foot, and mouth disease is caused by either coxsackieviruses or human enteroviruses. Its found in the digestive tract, including the mouth, esophagus, stomach, small intestine, large intestine, rectum, and anus.
The virus is spread from person to person when a sick person sneezes, coughs, or blows their nose. You can get it if you touch your nose, eyes, or mouth after touching something contaminated with the virus, such as a toy. You can also get it if you touch the stool or blisters of a person who is infected.
What Are The Complications Of Eczema Coxsackium
Common complications during the convalescence phase of eczema coxsackium include desquamation of the palms and soles and nail changes.
Nail changes occur 12 months after the acute infection and include:
- Horizontal ridging that slowly grows out
- Painless nail shedding .
Unlike other enteroviral infections, multiorgan involvement is rare in children with cutaneous coxsackievirus A6/16 infection.
Don’t Miss: How To Make Eczema Scars Go Away
When Should I Call My Childs Primary Care Provider
If you are worried, you are never wrong to call or make an appointment with your childs provider. Call your pediatrician immediately if your child:
- Is dehydrated: Look for dry lips and mouth or decrease in urine output
- Is listless or you are concerned about how sick your child looks, especially if he/she does not perk up after a dose of ibuprofen or acetaminophen
- Has a stiff neck
- Has a fever above 105 degrees, a fever that lasts more than two to three days, or is younger than 3 months old with a fever higher than 100.3 degrees
Remember: if your childs fingernails or toenails seem to be coming off a couple months after having HFMD, dont worry. You dont need to see your doctor for this unless the child is in pain or the skin around the nails looks infected.
Questions To Ask Your Doctor
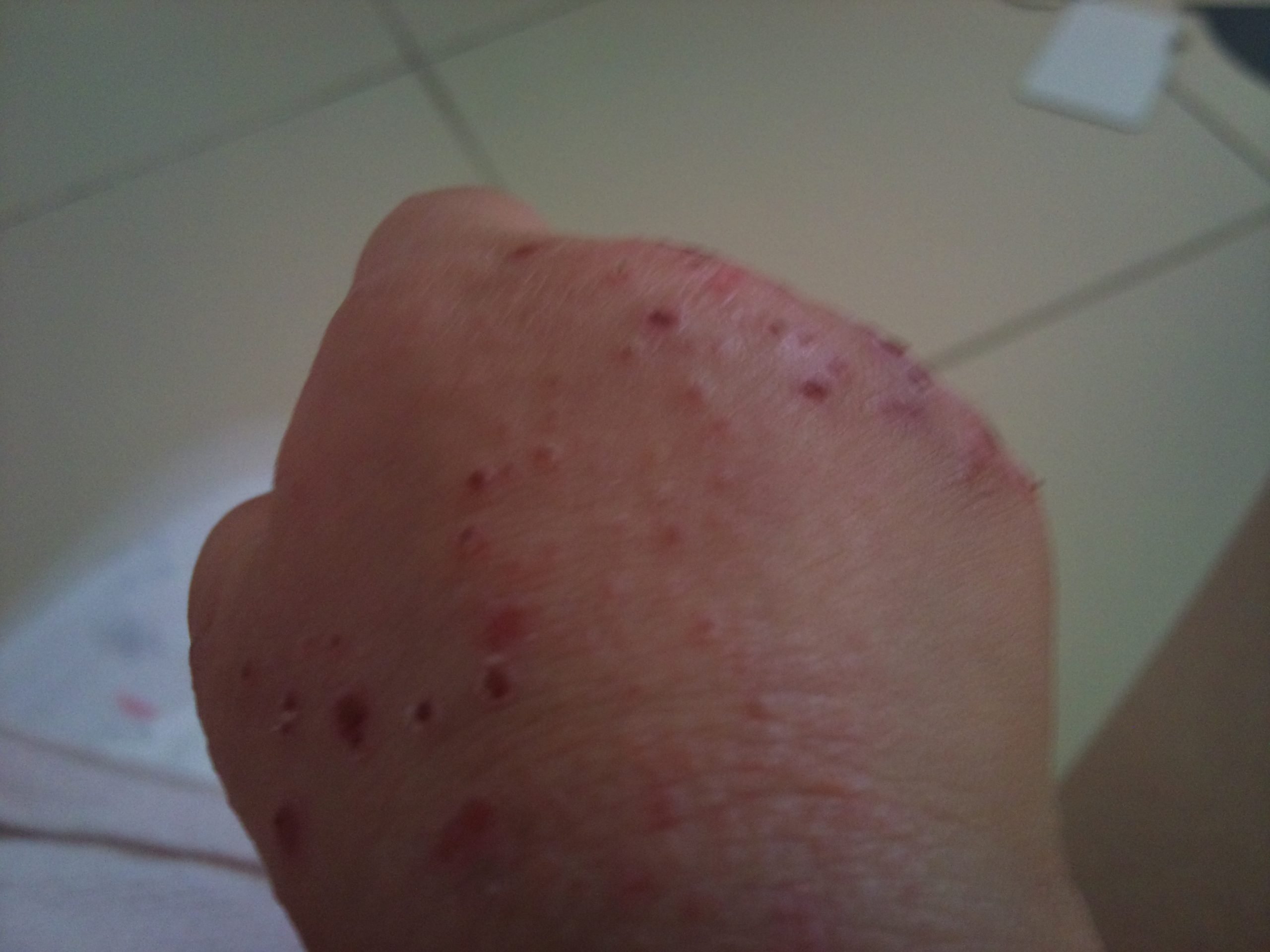
- Does the virus spread by touching the sores or blisters?
- Can you apply an ointment to the sores to relieve the pain?
- Do the sores or blisters leave long-term scars?
- Do the sores inside your mouth take longer to heal than the sores on your hands and feet?
- How long is my child contagious?
- My child has hand, foot, and mouth disease. Do I need to stay home from work, too?
Read Also: What Causes Eczema Flare Ups On Arms
Who Gets Hand Foot And Mouth Disease
HFM most often infects children under the age of 10, and most are under 5 years of age . It can uncommonly affect adults and tends to be more severe in the elderly, immunocompromised, and pregnant women.
Hand foot and mouth disease is very infectious viral infection several members of the family or a school class may be affected. Epidemics are most common during the late summer or autumn months.
What Is Eczema Coxsackium
Eczema coxsackium is an enteroviral infection typically affecting children with atopicdermatitis . It is characterised by an eruption of vesicles, bullae, and erosions affecting areas of active or inactive atopic dermatitis.
Eczema coxsackium is a form of Kaposi varicelliform eruption, and has been described as atypicalhand, foot and mouth disease . Both conditions are caused by enterovirus. However, eczema coxsackium is more widespread than hand, foot and mouth disease, and presents with vesiculobullouslesions that ulcerate and scab. The term eczema coxsackium was coined by Nahmias et al in 1968 .
See Hand foot and mouth disease images.
Read Also: How To Treat Open Eczema Wounds
Hand Foot And Mouth Disease
| Hand, foot, and mouth disease |
|---|
| Other names |
| Based on symptoms, viral culture |
| Prevention |
| As outbreaks |
Hand, foot, and mouth disease is a common infection caused by a group of enteroviruses. It typically begins with a fever and feeling generally unwell. This is followed a day or two later by flat discolored spots or bumps that may blister, on the hands, feet and mouth and occasionally buttocks and groin. Signs and symptoms normally appear 36 days after exposure to the virus. The rash generally resolves on its own in about a week. Fingernail and toenail loss may occur a few weeks later, but they will regrow with time.
The viruses that cause HFMD are spread through close personal contact, through the air from coughing and the feces of an infected person. Contaminated objects can also spread the disease.Coxsackievirus A16 is the most common cause, and enterovirus 71 is the second-most common cause. Other strains of coxsackievirus and enterovirus can also be responsible. Some people may carry and pass on the virus despite having no symptoms of disease. Other animals are not involved. Diagnosis can often be made based on symptoms. Occasionally, a throat or stool sample may be tested for the virus.
Dont Miss: Baby Eczema On Face Natural Treatment
What Are The Clinical Features Of Hand Foot And Mouth Disease
The typical incubation period of HFMD is 3-5 days but has been known to range from, 2-7 days.
Symptoms usually include:
- Lesions on the dorsal and palmar surfaces of the hands and feet. The progression is from flat pink patches to small, elongated greyish blisters, and, within a week, these peel off leaving no scars.
- Small vesicles and ulcers in and around the mouth, palate, and pharynx. These are sometimes painful, so the child eats little, frets, and may complain of a sore throat or mouth sores.
- Red macules and papules on the buttocks and sometimes on the arms. Lesions can also occur on the genitalia.
Atypical hand foot and mouth disease results in a more widespread rash. Features may include:
- Red, crusted papules
- Involvement of unusual sites such as the ear
- In children with atopicdermatitis, lesions may select skin affected by eczema .
Flat pink patches on the dorsal and palmar surfaces of the hands and feet are soon followed by small elongated greyish blisters. These resolve by peeling off within a week, without leaving scars.
Usually, there are also a few small oral vesicles and ulcers. These are sometimes painful, so the child eats little and frets. There may be a few on the skin around the mouth. In young children, a red rash may develop on the buttocks and sometimes on the arms.
Atypical hand foot and mouth disease due to Coxsackie A6 results in a more widespread rash, larger blisters and subsequent skin peeling and/or nail shedding.
Don’t Miss: Is Eczema A Skin Allergy
Girl 2 Left Scarred By Blisters From Hand Foot And Mouth Disease That Medics Thought Was Eczema
Aubrey Weatherall, from Stoke-on-Trent, was left squirming and screaming in agony suffering the “worst case” of the disease one nurse has ever seen
- 14:48, 26 Oct 2016
AT the age of just two, Aubrey Weatherall’s tiny body was covered in painful blisters, her skin peeling off like a snake.
Though medics first feared she was suffering an eczema flare up, the toddler was diagnosed with the “worst case” of hand, foot and mouth disease.
The nurse who spotted the common infection, which causes mouth ulcers as well as spots on the hand and feet, claims it was the most severe case she has seen in her 20 years of nursing.
Such was the severity of her condition, her mum Danielle fears she will be left scarred for life.
The mum-of-two said: “It was horrific.
“She had a temperature but no other symptoms. When I put her to bed at 6pm she suddenly started scratching and itching uncontrollably.
“She has eczema and chronic idiopathic urticaria – where her skin can flare up from an allergen – but she has never scratched like this before.”
How Long Is My Child Contagious
Children are most contagious at the beginning of the illness. Although viruses may last longer, children can go back to child care once the fever has been gone for 24 hours and they dont have open sores. I typically recommend waiting to return to child care until after the rash stops spreading, but it does not have to be completely gone. The rash will slowly fade over the course of a week or so. Hand washing, disinfecting surfaces and shared objects, and limiting close contact with infected individuals are the best ways to help prevent transmission.
Also Check: How To Treat Mild Eczema
How To Treat Hand Foot And Mouth Disease Yourself
You cannot take antibiotics or medicines to cure hand, foot and mouth disease. It usually gets better on its own in 7 to 10 days.
To help the symptoms:
- drink fluids to prevent dehydration avoid acidic drinks, such as fruit juice
- eat soft foods like yoghurt avoid hot and spicy foods
- take paracetamol or ibuprofen to help ease a sore mouth or throat
Check If It’s Hand Foot And Mouth Disease
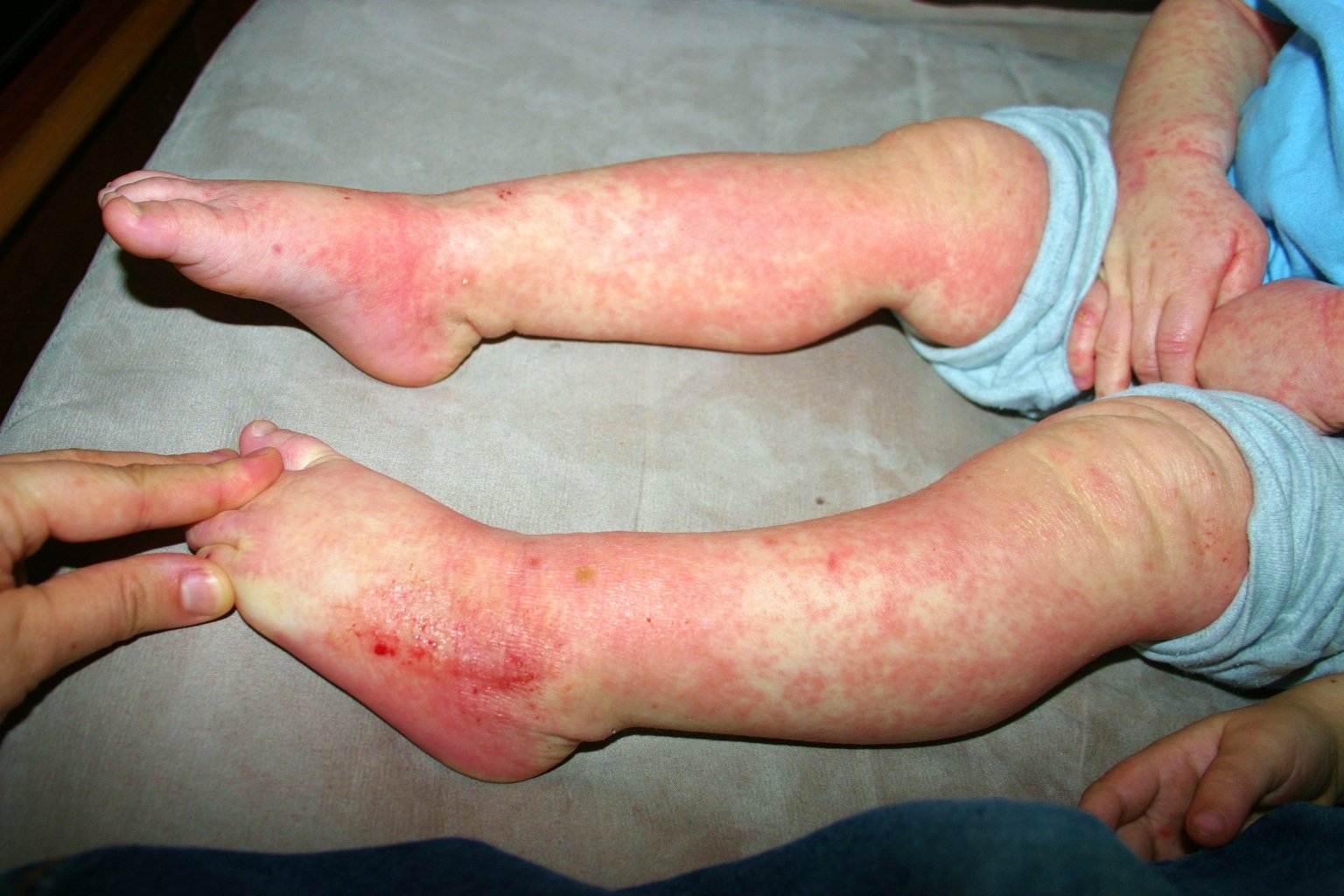
The first signs of hand, foot and mouth disease can be:
- a sore throat
- not wanting to eat
After a few days mouth ulcers and a rash will appear.
The symptoms are usually the same in adults and children, but they can be worse in babies and children under 5.
It’s possible to get hand, foot and mouth disease more than once.
Also Check: What Can Be Mistaken For Eczema
What Does The Rash Look Like
Depending on what virus your child has will determine the rashes appearance:
- Small, oval, white blisters on the palms, soles of the feet, as well as in the mouth.
- A red skin rash with a brown scale on it. The rash appears on the outer arms, hands, legs, feet, around the mouth and upper buttocks. The trunk is usually relatively clear. Sometimes there are blisters present, but they are not usually in the mouth and your child can eat and drink as usual.
Living With Hand Foot And Mouth Disease
Living with hand, foot, and mouth disease is a short-term challenge since the symptoms go away in about a week. As a parent caring for a child who has the virus, your primary goals are to keep your child comfortable and hydrated. It is best to keep them at home to rest and to avoid situations that will infect others.
Don’t Miss: California Baby Eczema Body Wash
What Happens When An Eczema Baby Get Hfmd
- Post author
Since last Friday when my baby girl Marcies teachers called to say they suspected that she has hand-foot-and-mouth disease , my life, my hubbys and Marcies have been miserable. Today is the 6th day of her HFMD, counting from Friday, 1st day where red bumps showed up on her hands and in her mouth. Here are some quick questions answered on HFMD, especially what happens when a baby with eczema has it .
1. How do you know if your baby has HFMD? Will it be confused with eczema rash?
When I brought Marcie to the doctor to verify if she has HFMD, the doctor did seem to take longer to check but made the diagnosis of HFMD when he saw ulcers in the mouth. Below are some pictures taken from the Singapores Health Promotion Boards website, provided by KK Womens and Childrens hospital.
2. What is the difference when HFMD happens to a baby with eczema?
In Marcies case, it didnt look much like the above but instead the HFMD red bumps appear where she has been scratching most frequently, like her hand and her foot. Im not sure if the degree of ulcers got to do with the immune system of the baby, but Marcie, fortunately, did not get red sores on her tongue but her tongue seems to be swollen and she drooled a lot.
3. Did the scratching get worse on the eczema skin patches?
It didnt for Marcie and instead got less scratching, until when the red HFMD bumps subsided, she started scratching again.
4. Will a parent get the HFMD from the child?
a. Hard-boiled egg
c. Yoghurt