Ad May Increase Your Risk For Some Eye Diseases
It seems that the more severe the AD, the higher your risk of developing certain eye diseases. At least, thats the finding from a 15-year study run in Denmark.
During this study, researchers looked at the medical records of adults in Denmark. In doing so, they discovered that those with AD had a higher risk of developing an eye infection called conjunctivitis, also known as pink eye.
Pink eye : Signs that you may have pink eye include:
-
Pink color to your eye
-
Watery, itchy eyes
-
Eyes sensitive to light
-
Wet, sticky or dry, crusty eyes
In this study, adults with AD also had a higher risk of developing the following eye diseases.
Inflamed cornea : This eye disease occurs when the eye becomes infected or inflamed. Warning signs include your eyes feeling:
-
Painful or uncomfortable
-
As if you have something in them
When caught early and properly treated, keratitis can often be cured.
Cornea changes shape
The cornea of the eye is normally round, as shown here.
Frequently rubbing your eyes can change the shape of your cornea. As the cornea starts to change shape, it begins to bulge. It becomes cone-shaped. This change in shape can cause the following warning signs:
- Nearsightedness
- Sensitivity to light, especially when driving at night
- Constantly changing prescription for eyeglasses or contacts
Signs of keratoconus
If you have any warning signs of keratoconus, ask your eye doctor to take a close look at the shape of your cornea.
How Can I Reduce My Risk Of Eczema
There are steps you can take that may prevent eczema outbreaks:
- Establish a skin care routine, and follow your healthcare professionals recommendations for keeping your skin healthy.
- Wear gloves for jobs where you have to put your hands in water. Wear cotton gloves under plastic gloves to absorb sweat, and wear gloves outside, especially during the winter months.
- Use mild soap for your bath or shower, and pat your skin dry instead of rubbing. Apply a moisturizing cream or ointment immediately after drying your skin to help seal in the moisture. Reapply cream or ointment two to three times a day.
- Take baths or showers with tepid rather than hot.
- Drink at least eight glasses of water each day. Water helps to keep your skin moist.
- Try to avoid getting too hot and sweaty.
- Wear loose clothes made of cotton and other natural materials. Wash new clothing before wearing. Avoid wool.
- Avoid sudden changes in temperature and humidity.
- Learn to recognize stress in your life and how to manage it. Regular aerobic exercise, hobbies and stress-management techniques, such as meditation or yoga, might help.
- Limit your exposure to known irritants and allergens.
- Avoid scratching or rubbing itchy areas of skin.
When Should I See A Dermatologist For Eczema
Atopic dermatitis can become overwhelmingly uncomfortable and leave you feeling like you have to scratch all the time. You should schedule an eczema evaluation at Integrated Dermatology of North Raleigh if you or your child experience:
- Overly dry skin
- Thickened or scaly patches
- Raw or severely sensitive skin
Eczema can cause issues anywhere on your body, including your hands, feet, ankles, chest, and bends of your elbows and knees. Scratching at eczema can damage your skin and lead to sores, which can leave you vulnerable to secondary issues, like skin infections.
Fortunately, with the help of the dedicated dermatologists at Integrated Dermatology of North Raleigh, you wont have to worry about eczema taking over your life.
Read Also: Cetaphil Moisturizing Cream For Eczema Review
Am I Entitled To A Referral To A Specialist
You will need to see your GP to ask for a referral to an NHS dermatologist. Some private dermatologists will see you without a referral if you are self-funding, but if you are claiming on a medical insurance policy, a GP referral is usually required. Your GP can decide whether a specialist referral is necessary and, if so, recommend appropriate hospitals or clinics.
Access to NHS specialist services is based on need and your GP will assess your need. Your GP may also have local guidelines or criteria to consider when referring. If your GP does not feel you need a referral, find out why. It may be that your eczema is limited or mild in presentation, and therefore should be controlled by topical treatments that a GP can prescribe.
When referring, GPs need to demonstrate that it is clinically appropriate to do so for example, in cases of an uncertain diagnosis, recurrent bacterial infections, severe uncontrolled eczema or a significant impact on quality of life or psychological wellbeing. Information on referral for children can be found in the NICE guidelines for Atopic eczema in under 12s: diagnosis and management.
How Common Is Eczema
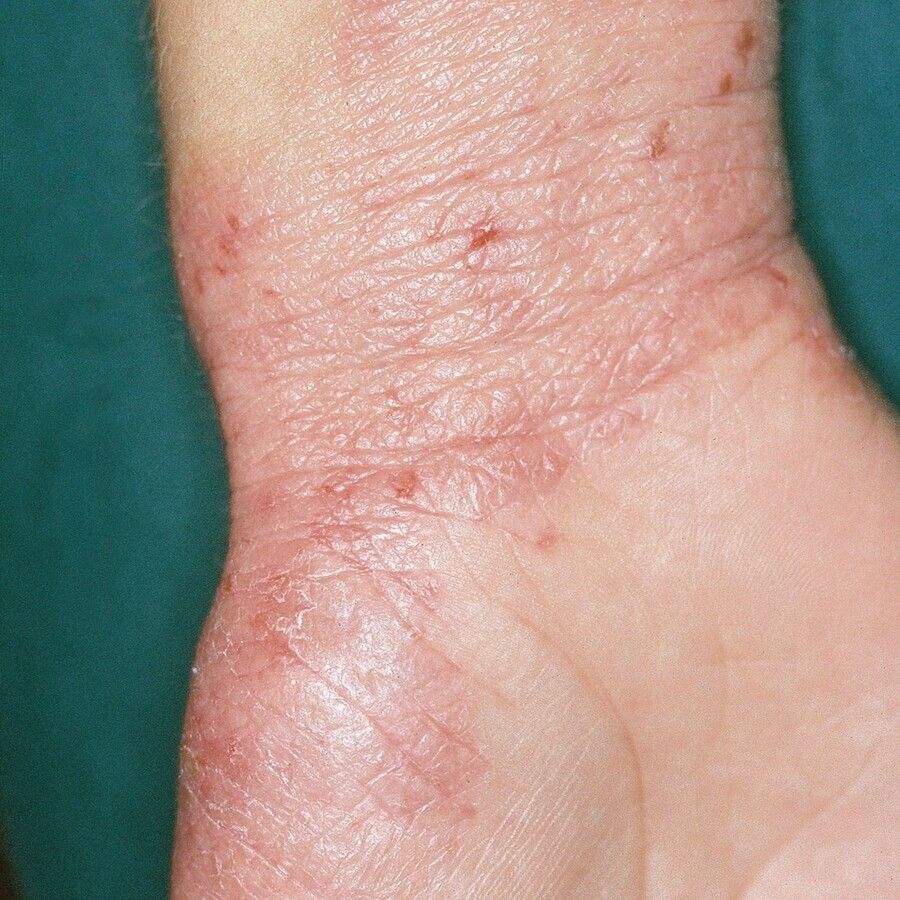
Eczema affects up to 15 million Americans. Infants are prone to eczema and 10% to 20% will have it. However, nearly half outgrow the condition or have significant improvement as they get older.
Eczema affects males and females equally and is more common in people who have a personal or family history of asthma, environmental allergies and/or food allergies.
Recommended Reading: Best Eczema Products For Face
Read Also: How To Get Rid Of Eczema Around Mouth
How These Practitioners Can Help
Both of these doctors can provide allergy testing when necessary. For instance, a dermatologist may perform a skin patch test to determine the cause of your skin reaction. An allergist may also perform a skin patch test and more in-depth allergy testing.
A dermatologist can help you choose products that are less likely to irritate your skin. An allergist may provide medications to help you manage your allergies and even provide immunotherapy to reduce your sensitivity to that substance.
Fortunately, you wont be at a loss regardless of which doctor you choose to see. If you see a dermatologist, and they cannot diagnose or treat the underlying cause of your symptoms, they will simply refer you to an allergist and vice versa.
Avoiding Atopic Dermatitis Triggers
Everyoneâs eczema is different. Common triggers include stress, sweat, certain chemicals, dust, and pollen. Some foods can trigger flares in infants and children. A symptom diary can help you track your or your childâs triggers so you know what to avoid.
Try these tips to limit contact with triggers:
- Protect your skin, especially when the weather is cold and dry.
- Be careful with soaps, shampoos, and other commercial skin care items. Read the labels carefully.
- Rinse laundry twice to remove detergent residue.
View a slideshow to see top eczema triggers to avoid.
Read Also: Can You Have Eczema On Your Scalp
Allergy Doctors In Chicagoland
No one wants to scratch and sneeze every day. If you are starting to get unusual rashes or red patches on your skin, consult with an allergy specialist to receive an appropriate diagnosis and treatment.
Our board-certified doctors here at Oak Brook Allergists can help you resolve your allergy problems once and for all. We have four locations in the Chicago area for your convenience.
To schedule an appointment with one of our caring allergists, contact us today by calling us at 574-0460 or by filling out our online appointment request form now. We look forward to helping you get back in the clear!
Treating Atopic Dermatitis In Infants
About 10% to 20% of infants develop eczema, with the rash usually on the face and scalp. In most cases, this condition improves after age 5 and may disappear for good.
Medical experts believe itâs a genetic condition or passed from parents to their kids. Symptoms can vary depending on the age of the child.
In more severe cases, infants can have eczema on uncommon areas like the torso, elbows, and knees. Children and teens will notice the rash in the inner elbows, behind the knees, on the neck, or on the wrists and ankles. The skin may appear drier and thicker, and develop a scaly texture.
There are some steps you can take to treat your child’s eczema or prevent flare-ups:
- Avoid skin care products with fragrances and other possible irritants.
- Cut your childâs fingernails and encourage them to wear gloves to prevent skin damage from excessive scratching.
- Maintain a routine of bathing, moisturizing, and applying age-appropriate treatments recommended by a pediatrician. Ask your doctor about the âsoak and sealâ method.
- Talk to a pediatrician or dermatologist about the benefits of oatmeal baths or bleach baths to reduce inflammation and discourage bacterial growth.
- Boost the effectiveness of any topical medication and rehydrate the skin by using wet wrap therapy. This can also prevent your child from scratching their skin.
Read Also: Can Eczema Come On Later In Life
Where Eczema Commonly Occurs
Though patches of eczema can occur anywhere on the body, they most often appear on hands and feet, in the front of the bend of the elbow, behind the knees, and on the ankles, wrists, face and neck.
Eczema can also affect the skin around the eyes, including your eyelids. Scratching can cause redness and swelling around the eyes.
How A Dermatologist Can Help With Eczema
Eczemais a skin condition in which symptoms can be managed and prevented with help from a dermatologist.
To start with, they can help conduct patch tests to help identify the trigger of your eczema rash. However, if you are dealing with allergic dermatitis, your dermatologist may refer you to an allergist. To help you manage symptoms of eczema, a dermatologist may recommend lifestyle changes, coping techniques, andnatural skincare remedies.
For example, this Organic Manuka Skin Soothing Cream is dermatologist tested and approved. Made with just 6 natural ingredients, its also EWG Skin Deep 1 Rated. We love it for its soft, buttery texture and ultra-hydrating properties. Its a great choice for dealing with eczema, psoriasis, rosacea, sunburn, cuts and scrapes, and sensitive or dry skin.
Recommended Reading: Baby Has Eczema Only On Face
Chronic Itchy Skin Condition
Eczema also known as dermatitis is a chronic, itchy and inflammatory skin condition. There are two main eczema types:
- Atopic dermatitis: Predominately a childhood disease, although adults may continue to have patches of eczema on the hands, feet and elsewhere.
- Contact dermatitis: Caused by exposure to irritating or allergenic chemicals contacting the skin. Can occur at any time in the patients life.
Our skilled team of dermatologists at Penn State Health are here to help diagnose and treat your eczema. We see more than 40,000 patients each year, so you can rest assured that you are in the very best hands. For your convenience, our team offers evening clinic hours, as well as an innovative open-access clinic for acute situations.
If you or a loved one have eczema, there is good news: with the correct treatment, eczema can be controlled. We are here to help ease your skin discomfort and get you back to your active lifestyle.
How Dermatologists Can Help
Dermatologists are in a unique position to help their patients with psoriasis. They can prescribe medications and ointments to help clear up the skin, as well as recommend lifestyle changes that can lessen the symptoms of psoriasis. Dermatologists can also provide emotional support to their patients, who may feel self-conscious or embarrassed about their condition.
Recommended Reading: Aloe Vera For Babies Eczema
Should I See A Dermatologist For Eczema
Whether or not you should see a dermatologist for eczema largely depends on the severity of your problem. If the condition is fairly mild, you may want to try to handle it yourself. For more severe problems, it is likely in your best interest to have professional assistance managing and monitoring the condition.
Eczema is a skin condition whose cause is unknown. A person can live for decades before the problem suddenly arises, and individuals can suffer from eczema in varying degrees. For some people, the problem is fairly mild and may be contained in a limited area. For others, the itching, swelling, and burning associated with this condition may be severe, and it may occur in multiple sites on the body. Where your problem is located and the severity of it should factor into your decision to see a dermatologist for eczema.
If you feel that your condition is mild, you may want to try over-the-counter remedies before seeking medical attention. As there is no cure, there is generally no reason to go to a dermatologist if you can manage the problem yourself. If you decide later that it may be better for to get professional help, it will not be too late.
What Can A Doctor Do For Eczema
Doctors usually prescribe a topical, not an oral, medication. A prescription topical steroid or a topical nonsteroidal anti-inflammatory such as tacrolimus or pimecrolimus reduce inflammation, relieve itching, and moisturize the skin. Steroids may be safer options for treating babies and children because they are time-tested. A patient with moderate to severe eczema must calm the rashy inflammation down and should not worry too much about using a topical steroid. Patients use it temporarily, twice daily for one to two weeks. With mild eczema normal skin that may have an itchy, dry patch or two a nonsteroidal anti-inflammatory should work fine and would not have steroid side effects such as thinning or atrophied skin.
More About this Book
Don’t Miss: Best Cream For Extreme Eczema
Treatmentfrom Either Type Of Doccan Bring Relief
So, how are Hands hives on her neck right now? After a long period of being clear, theyre making a comeback , so shes returned to rubbing on topical steroids prescribed by her dermatologist. And White has continued to receive Xolair injections from her allergist-immunologist every four to six weeks for the past seven years. Ive never been in remission, she says. But, she adds, the regular shots keep her hives under control.
Systemic Therapy For Atopic Dermatitis
Doctors reserve this treatment for serious flare-ups in people with severe eczema, typically when other treatments fail to work. They donât use them over the long term, but for a few weeks at a time at most.
Thatâs because of side effects, including nausea, vomiting, and an upset stomach. Less common but more serious side effects may include more skin infections, suppression of bone marrow, and raised risk of skin cancer. In addition, you may get another flare-up as your doctor weans you from the treatment.
The treatment delivers drugs in the form of pills, injections, IV infusions, and inhalers to lessen the response of your immune system that causes eczema symptoms. Some common types of these medicines include azathioprine, cyclosporine, and methotrexate.
There are also prescription creams and ointments that treat eczema by controlling inflammation and reducing immune system reactions. Examples include pimecrolimus , which is a cream, and crisaborole and tacrolimus , which are ointments. You should only use these for a short time if other treatments don’t work — and you should never use them on kids younger than 2, according to the FDA.
Systemic therapy is not typically for someone with a compromised immune system or multiple other health issues.
Also Check: How To Treat Eczema Child
What Can I Do To Prevent Scalp Eczema
When scalp eczema flare-ups are managed, its essential to take steps to maintain unblemished skin. According to Dr. Rogers, Maintaining scalp health between flare-ups is just as important as clearing an active flare-up. Once you have scalp eczema under control, its essential to work with your dermatologist to develop a skincare plan to keep your scalp healthy. Your dermatologist can provide specific recommendations to meet your unique needs and skincare goals, but some of the basic recommendations to minimize the risk for flare-ups include:
- Use a gentle, pH-balanced shampoo to keep your hair clean, especially if youve been sweating.
- Apply moisturizer at least once each day. The Avene XeraCalm A.D. Lipid-Replenishing Cream is a great option. It has been proven safe and effective for eczema-prone skin all over the body, including the scalp.
- Review the ingredients on your shampoo, conditioner, and other haircare and styling products. Look for drying ingredients like alcohol and irritating ingredients like perfumes and dyes. Avoid those products that may irritate the scalp and trigger a flare-up.
- Take steps to protect the skin from sunlight, heat, cold, and dry weather conditions that trigger flare-ups. This might mean wearing hats or scarves over the head in cold weather or to protect against sun exposure. You can also apply sunscreen to exposed areas of the scalp.
When Do I Need To See A Dermatologist
When Do I Need To See a Dermatologist? You might not consider talking with a dermatologist when youre dealing with skin-related concerns. Sometimes you can resolve your skin issues through makeup, lotions, or other things you can find at your local drugstore.
But there are often times when you will need to contact a dermatologist for help. Here are some instances of times when you need to talk with such an expert.
Your Skin Becomes Inflamed
You might develop inflamed and itchy skin around certain body parts. The skin will swell and become red, and you might notice slight bumps in some areas.
Your dermatologist can talk with you about what triggers the inflammation and what you have been trying to use to correct the issue. Your dermatologist may find you have rosacea or eczema, or another skin disorder that requires extra assistance.
Such conditions will require different treatments, as some traditional lotions and other products you find at your local market might not work well against rosacea or eczema.
Skin Moles and Growths Appear
People often notice skin growths and moles around their bodies as they age. These arent always appealing, and they can be signs of skin cancer or another severe condition. These features could be signs of cancer if:
Contact your dermatologist immediately if you see any moles or growths that look unusual. You may be referred by your dermatologist to a doctor who can treat the issue before it becomes worse.
Noticeable Veins
You May Like: Side Effects Of Eczema Medication