Causes And Risk Factors Of Eczema
Skin affected by eczema is unable to retain moisture well, possibly because of low production of fats and oils. It is also caused by a disrupted skin barrier, allowing whatever moisture the skin has to freely evaporate into the air. This causes it to become dry and lose its protective properties.
It’s not clear what causes certain people to develop eczema, specifically atopic dermatitis.
Children are more likely to develop eczema if other allergic diseases such as hay fever and asthma run in the family, which suggests that there may be a genetic component to the condition. Read more about conditions related to eczema below.
Though dermatologists dont necessarily consider eczema an autoimmune disorder, the symptoms of atopic dermatitis are thought to be the result of an immune system overreaction or dysfunction.
Indian Journal of Dermatology
In addition to genetic and immune system factors, environmental factors also play a role in worsening or triggering eczema.
Philipp Oscity/Alamy
Allergic Eczema On The Face Or Neck
Contact eczema is caused by an allergy. It occurs when your skin has an allergic reaction after coming into contact with a specific product. You may have been exposed to this product several times in the past without having a reaction. Indeed, one characteristic of contact eczema is that the allergy can appear suddenly.
Ways To Prevent Eczema
If you have allergies, hay fever, hives, or dry, overly sensitive skin, you may also have bouts of eczema, typified by a red and dry rash that itches like crazy. Here are tips and strategies you can use to prevent eczema.
There are about 10 types of eczema, but atopic dermatitis is among the more common kinds.
“The eczema rash typically appears as red, swollen patches or blotches on the face and neck and the folds of the elbows and knees, but it can also affect the hands and feet or the whole body,” says Kristin Leiferman, MD, professor of dermatology at the Mayo Medical School in Rochester, MN. No one knows what causes it, but it’s not contagious.
A Cyclic Phenomenon? Eczema symptoms come and go. One day your skin may be fine, and the next, you may experience a flare-up of redness and itchiness. Triggers include exposure to harsh soaps or household cleaning products, a skin-drying environment like when the furnace comes on in the fall and early winter, coarse or scratchy clothes, and possibly stress.
Many women also report that they experience eczema flare-ups at the same time during their menstrual cycles each month. They experience it either premenstrually or during their periods, says Dr. Leiferman.
Here are some things you can do to help prevent eczema:
Go fragrance-free. “I advise patients to look for bland moisturizers that don’t have a lot of fragrance, color, or additives that could irritate skin,” says Dr. Leiferman.
Treatment
Don’t Miss: Natural Baby Cream For Eczema
Living Well With Eczema
While eczema wont go away on its own, with some know-how and the appropriate care, its possible to live well with eczema. Having an eczema specialist on your side is invaluable. To learn more about managing eczema and to schedule a visit with Dr. Kage, call 860-288-1160 or send your appointment request online using our booking form.
You Might Also Enjoy…
How To Use Emollients
Use your emollient all the time, even if you’re not experiencing symptoms, as it can help prevent the return of discoid eczema. Many people find it helpful to keep separate supplies of emollients at work or school.
To apply the emollient:
- use a large amount
- do not rub it in smooth it into the skin in the same direction that the hair grows
- for very dry skin, apply the emollient every 2 to 3 hours, or more often if necessary
- after a bath or shower, gently dry your skin and then immediately apply the emollient while the skin is still moist
If you’re exposed to irritants at work, make sure you apply emollients regularly during and after work.
Do not share emollients with other people.
Also Check: Tips For Eczema Flare Ups
How Infected Eczema Is Treated
The way you treat infected eczema depends on whether it was caused by a virus, bacteria, or fungi. Viral infections may be treated with antiviral medications or allowed to heal themselves.
Antibiotics are used in bacterial infections. Mild bacterial-infected eczema is treated with a topical antibiotic first. A steroid cream may also be used to reduce inflammation.
Oral antibiotics are reserved for more severe cases of infected eczema. Theyre also used for infections that have spread to other parts of your body.
A fungal infection may also be treated with steroids. Its treated with topical antifungal creams as well.
Some people prefer using natural treatments in addition to prescription medications. This is due to the long-term side effects of steroids, such as thinning skin.
You may consider the following natural treatments, as well as the pros and cons of each:
- herbal supplements for eczema flares, such as primrose oil
- essential oils, such as borage, evening primrose, and tea tree
- probiotics, to offset gastrointestinal side effects from antibiotics
- natural soaps and creams with emollients, to decrease skin inflammation
Be aware that natural treatments for eczema and skin infections havent been widely studied for safety or efficacy.
Make sure you discuss all these options with your doctor first before trying them out.
Infected eczema may lead to the following complications:
You may need to go to the hospital if you start experiencing:
- fever
- low energy
- excessive fatigue
Choose Facial And Body Care Products Carefully
Cosmetics, soaps, hair products, perfumes, scented lotions, and shaving creams can all contain ingredients that irritate the skin and promote eczema flare-ups. Therefore, before using them regularly, we recommend that you patch test these products by applying them to a small area of your skin and waiting 24 hours. This is a great way to check whether the product will cause you to have a skin reaction.
And of course, your pharmacist is always available to help you make an informed decision!
Read Also: How To Clear Up Eczema On Baby’s Face
Ultraviolet Radiation Therapy For Eczema
Exposure to ultraviolet radiation can help reduce the symptoms of chronic eczema. Exposure under medical supervision can be carefully monitored with the use of specially designed cabinets the person stands naked in the cabinet and fluorescent tubes emit ultraviolet radiation.A person with stubborn eczema may need up to 30 sessions. The risks of unsupervised ultraviolet radiation therapy can be the same as for sunbathing faster ageing of the skin and greater risk of skin cancer.
What Causes Eczema Flare
Eczema flare-ups occur when the immune system is overloaded and unable to fight off the things that trigger inflammation for an individual and results in the red, itchy, and dry skin.
A number of factors can contribute to an eczema flare-up, from environmental factors, to internal stresses and reactions.
Don’t Miss: Can You Get Eczema On Your Head
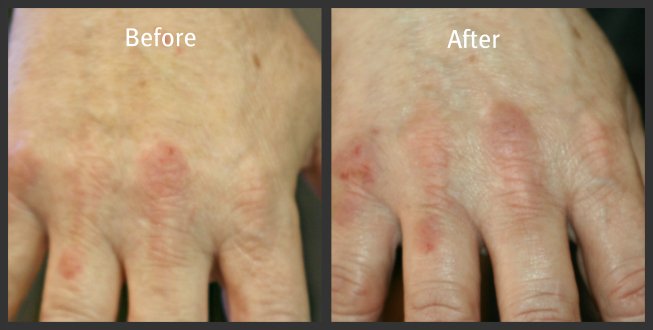
What Type Of Moisturizer Is Good For Hand Eczema
Mild hand eczema on the knuckles
The more water there is in a lotion or moisturizer, the more likely it is to worsen your hand eczema. Moisturizers usually contain more water than oil, and when the water evaporates it can dry out the skin. The best moisturizer for hand eczema is a greasy ointment, such as petroleum jelly. Be sure to read the label to determine which moisturizer has the least amount of water.
The NEA Seal of Acceptance directory has a list of moisturizers specially formulated for eczema skin.
Apply the moisturizer to your hands immediately after you bathe and each time you wash your hands.
Remember that it can take a few months for a flare-up to clear. Even if your hands appear eczema-free, you will sometimes need to take special care with them to avoid a return of symptoms.
Favorite Alternative Medicine Resource
National Eczema Association Alternative Treatment
Our favorite way to take a deep dive into authoritative articles about eczema alternative medicine treatments is to visit the alternative treatment tag page on the NEA website. Learn about how acupuncture, Ayurvedic medicine, natural oils, and other alternative treatments can help to ease eczema symptoms.
The National Eczema Association has an online store of sensitive skinfriendly products that bear the NEA Seal of Acceptance, meaning they are intended for people with moderate to severe skin conditions. Get moisturizers, cleansers, detergents, and other items designed to protect and not irritate your skin.
Recommended Reading: Best Thing For Eczema On Legs
What Causes An Eczema Flare
Triggers arenât the same for everyone, and there may be a lag between the trigger and the symptoms. Sweat, fabrics , pet dander, hot or cold weather, and harsh soaps are common triggers. Others include:
- Dry skin. It could get scaly, tight, and easy to crack, which can lead to a flare-up.
- Stress. For some people, emotional stress can trigger eczema symptoms. Doctors donât know exactly why this is, but there are ways to help lessen the stress in your life, from mind-body and meditation techniques, to lifestyle changes, to therapy approaches like cognitive behavioral therapy. Talk to your health care provider about how to reduce stress if itâs a trigger for your eczema.
- Irritants. These could include household items like hand and dish soap, laundry detergent, shampoo, body wash, or home cleaners and disinfectants. Juice from fruit, vegetables, and even meats can act as triggers in some people. Other common irritants include:
- Cigarette smoke
- Antibacterial ointment like neomycin and bacitracin
- Formaldehyde
- Cocamidopropyl betaine
- Paraphenylene-diamine
- Isothiazolinone (antibacterial in baby wipes and other personal products
Favorite Resource For Diet Advice

Avoiding food allergy triggers may help you manage eczema, but sometimes you need help identifying precisely what the triggers are. This is where an elimination diet may help. This approach involves omitting a food you think is problematic and then reintroducing it to see what happens. We love this article with information from the dermatologist Peter Lio, MD, which delves into some of the misconceptions about the diet, as well as the link between eczema and what you eat.
Recommended Reading: How To Cure Eczema On Hands
Favorite Eczema Tracking App
Eczema Tracker
Information is power when it comes to managing eczema symptoms and flare-ups. Eczema Tracker allows you to take a photo of flare-ups and monitor your condition, as well as track and analyze a wealth of information concerning your triggers, allergies, and skin. The app even provides local pollen, weather, mold, and humidity information to help you manage your symptoms. It uses your data to find trends that may lead to flare-ups. Eczema Tracker is available only for iOS in the Apple Store. It is a free app.
Oral Or Injected Immunosuppressants
Oral immunosuppressant medications prevent the bodys immune system from sending an inflammatory response to the skin, which results in less itching, redness, and rash.
Immunosuppressant medications are available in varying strengths, and doctors determine the dosage based on your age, severity of symptoms, location and extent of the rash, your weight, and whether you have other medical conditions. Typically, these medications are taken once or twice daily, although the dosage can vary.
If eczema or dermatitis is severe, a doctor may recommend immunosuppressant medication that is injected into the skin. Your dermatologist determines the appropriate schedule of injections. He or she may administer the injections in a doctors office or show you how to do it so you can inject the medication at home.
Dermatologists may prescribe immunosuppressant medication for weeks or months or until symptoms of eczema or dermatitis are under control. Often, our doctors may reduce or stop a prescription at that time to see whether symptoms can be managed using topical medication, , or at-home therapies.
In some instances when symptoms cant be relieved by other treatments, therapy with immunosuppressant medications may continue for years. Your doctor can discuss side effects of immunosuppressant medications.
Read Also: Why Is My Eczema Burning
Is A Cure Or Better Treatment For Eczema On The Horizon
Without a cure on the near horizon, we here at Johns Hopkins are creating an Eczema Day Treatment Unit to help our patients with moderate to severe eczema keep their symptoms under control and prevent flare-ups. We anticipate that this novel, multidisciplinary program will include experts from Child Life, behavioral psychology, allergy, dermatology and infectious diseases to provide the comprehensive care these children need care that cannot be provided in an average clinic visit.
A primary goal of the day treatment unit will be education children and their families will learn techniques such as wet-wrap therapy, to help deeply moisturize the skin. This therapy involves coating the skin with a topical ointment, followed by a greasy ointment like petroleum jelly, then dressing in wet pajamas, followed by dry pajamas, allowing the skin to soak in the moisture.
Natural Treatments At Home
Aside from moisturizing your skin, some natural treatments may help heal your skin.
Oatmeal baths are one type of natural treatment that can soothe the itchiness and discomfort of eczema rashes. Be sure to use lukewarm water and follow up with a moisturizer immediately after.
Theres some evidence that both probiotics and prebiotics may stabilize your microbiome to help treat inflammation. However, more research is needed to support this approach in eczema treatment.
Also Check: Is Shea Moisture Good For Eczema
Eczema Coping Tips Beauty Products
Suggestions for using beauty products include:
- Remember that even hypoallergenic cosmetics can irritate your skin. Whenever possible, keep your face free of make-up.
- Avoid perfumes, fragranced skin lotions and strongly scented shampoos.
- When using a new cosmetic, try testing it first on a small, inconspicuous area of skin such as your forearm. If you experience a reaction, dont use the product again.
What Causes The Spread Of Eczema
The condition is non-contagious, so you cannot pass it on to someone else. However, your rash can get bigger and spread to other parts of your body, including your face and scalp. Allergens, germs and scratching an itchy rash can trigger more inflammation that causes eczema to worsen and spread.
1. Scratching
Flare-ups are not the same for everyone. In some people, the itch can be so severe that scratching is simply unavoidable. Scratching can make your eczema worse because it triggers the release of inflammatory substances, which brings in more inflammation.
Furthermore, repeated scratching and rubbing can turn a rash into a plaque of thickened skin. This process is called lichenification.
How to Manage ItAs much as possible, you want to stop the itch-scratch cycle. Oral and topical anti-itch medications are available over the counter. Some are available only by prescription. Creams, gels and ointments with low-grade steroids can reduce inflammation and relieve itching, thus preventing the spread of eczema.
2. Irritants and Allergens
Common triggers for eczema include exposure to allergens, such as pollen, animal dander, mold and dust mites. Skin irritants found in many household products, such as soaps, detergents and antibacterial cleansers, may also trigger a flare.
3. Microbes
4. Stress
Don’t Miss: Acne & Eczema Whipped Shea Butter
Everyday Things That Can Trigger Eczema
The factors are
- Metals like Nickel
- Personal care products.
- Specific fabrics like polyester or wool.
2. Stress Another factor for eczema is stress. Life is incomplete without stress. Each human has stress in their life. But too much stress can lead to eczema.
3. Defects in skin structure that lock the way for the moisturizer to penetrate inside but allow the pathogen to enter inside the skin
4. Children are likely to develop eczema if they
- Live in an urban or polluted area.
- Live in cold climatic conditions.
5. Daily Activity: Sometimes, our daily activities may cause eczema. The activities are
- Prolonged exposure to water.
- Become too hot or too cold.
- Not using proper moisture.
- Living in arid climates all year round.
6. Eczema can also start with certain chronic conditions that affect or weaken our immunity power. For example, the chronic conditions that can worsen an eczema flare are
- The cold or flu infection.
- Bacterial infection.
- Any types of allergic reaction from dust, smoke, pollen, or pets.
Eczema Coping Tips Good Hygiene

Skin affected by eczema is more vulnerable to a range of infections, including impetigo, cold sores and warts. The bacterium Staphylococcus aureus may cause a secondary infection of impetigo, and possibly contribute to the symptoms of eczema.Suggestions for washing include:
- Take lukewarm baths or showers, and avoid really hot showers.
- Dont use ordinary soap, as the ingredients may aggravate your eczema. Wash your body with warm water alone. For armpits and groin, use soap-free products, such as sorbolene cream.
- Bath oils can help to moisturise your skin while bathing.
- When towelling dry, pat rather than rub your skin.
Recommended Reading: What Is Eczema And What Does It Look Like
Diagnosing Food Allergy And Eczema Flare
- Your child’s doctor may suggest the steps listed below:
- Remove the suspected food or foods from your child’s diet for 2 weeks. The eczema should greatly improve.
- Then give your child that food when the eczema is under good control. This is called a “challenge.”
- If the food is causing flare-ups, the eczema should become itchy and red. The flare-up should occur quickly within 2 hours of eating the food.
- If this occurs, avoid giving this food to your child. Talk to your child’s doctor about the need for any food substitutes.
- If the eczema does not flare-up, your child isn’t allergic to that food.
How Can I Reduce My Risk Of Eczema
There are steps you can take that may prevent eczema outbreaks:
- Establish a skin care routine, and follow your healthcare professionals recommendations for keeping your skin healthy.
- Wear gloves for jobs where you have to put your hands in water. Wear cotton gloves under plastic gloves to absorb sweat, and wear gloves outside, especially during the winter months.
- Use mild soap for your bath or shower, and pat your skin dry instead of rubbing. Apply a moisturizing cream or ointment immediately after drying your skin to help seal in the moisture. Reapply cream or ointment two to three times a day.
- Take baths or showers with tepid rather than hot.
- Drink at least eight glasses of water each day. Water helps to keep your skin moist.
- Try to avoid getting too hot and sweaty.
- Wear loose clothes made of cotton and other natural materials. Wash new clothing before wearing. Avoid wool.
- Avoid sudden changes in temperature and humidity.
- Learn to recognize stress in your life and how to manage it. Regular aerobic exercise, hobbies and stress-management techniques, such as meditation or yoga, might help.
- Limit your exposure to known irritants and allergens.
- Avoid scratching or rubbing itchy areas of skin.
Don’t Miss: Vitamin E Good For Eczema