Will Vulvar Dermatitis Go Away On Its Own
Vulvar dermatitis may go away without medication, depending on the cause. If its caused by an allergic reaction or sensitivity, the symptoms will go away on their own after the irritant is removed.
If vulvar dermatitis is caused by an infection or skin condition, medication is usually needed to clear the infection or manage the symptoms.
What Every Clinician Should Know
Vulvar pruritus is the most common symptom of skin disease. In evaluating vulvar pruritus, it is helpful to differentiate women with acute symptoms from those with chronic symptoms. Acute anogenital pruritus often is infectious, with allergic and irritant contact dermatitis playing a role in some cases. Genital infections such as trichomoniasis and cadidiasis as well as dermatitis should be considered in the differential. Chronic pruritus, in general, has a history of gradual onset, examples of which include lichen simplex chronicus as well as lichen scleroses, psoriasis and various manifestations of HPV-related disease.
The term dermatitis describes a poorly demarcated, erythematous and usually itchy rash. Subtypes are numerous and can be classified as either exogenous or endogenous . Dermatitis has been reported to occur in 20-60% of women presenting with chronic vulvar symptoms, with atopic being by far the most frequently encountered. Irritant contact dermatitis has been identified in 5-26% of women with diagnosed vulvar dermatitis, often as a result of exposure to irritants such as detergents, soaps, perfumes, semen, and prophylene glycol, an additive found in many topical medications.
What Relieves Symptoms Of Genital Eczema Quickly
Its always best to speak to a healthcare provider about the best treatment for genital eczema. However, if you need relief from itching quickly, there are steps you can take at home, including having an oatmeal bath or applying a cool compress to the affected area. Taking an antihistamine wont treat eczema, but it can help relieve the itchiness that you feel.
Recommended Reading: Type Of Eczema That Looks Like Ringworm
Vulvar Skin Conditions And Their Treatment
Several vulvar skin conditions are familiar from other areas of the body but may be difficult to recognize when they appear on the vulva. These include the following:
Eczema. This inflammatory skin condition disrupts the skin’s surface, causing red patches and thin cracks, weeping, and crust formation. On the vulva, crusts are less likely, but eczema may initiate a cycle of vulvar itching and scratching that leads to lichen simplex chronicus thickened and intensely itchy skin. If eczema affects an area of the vulva called the vestibule, it may cause stinging and burning. Sometimes eczema appears in early childhood and its cause is unknown. More often, it begins with exposure to an irritant or allergen .
|
Many things can cause an allergic reaction or irritate vulvar skin. Here are some of the leading suspects: Irritants
Allergens
Adapted from The V Book, by Elizabeth G. Stewart, M.D., and Paula Spencer . |
To diagnose vulvar eczema, the clinician will ask about your symptoms your history of eczema, allergy, and related conditions your vulvar cleansing habits and any products the vulva has been exposed to. During the exam, she or he will look for redness, scaling, cracking, and thickening.
Other Rashes In The Vaginal Area
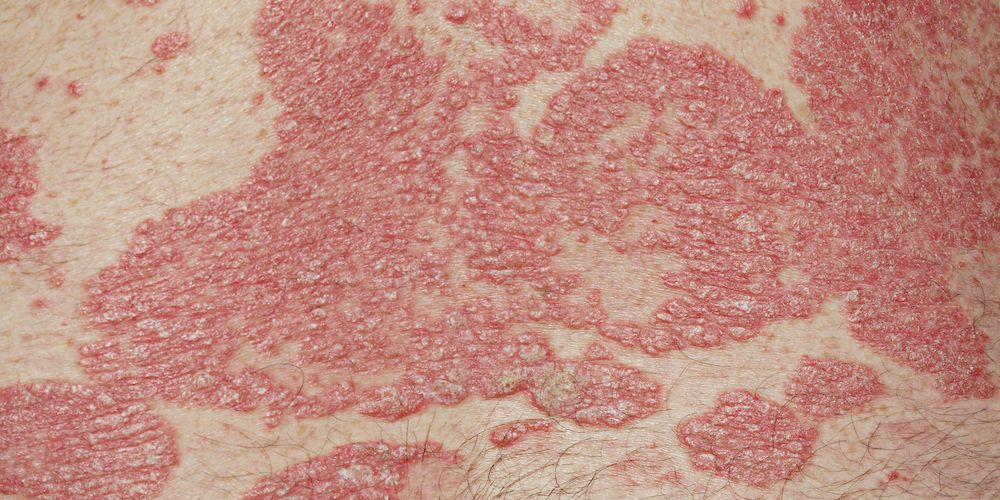
Other conditions that may cause a rash in the vaginal area include:
- Scabies, which is an itchy skin condition caused by tiny mites that burrow into the outer layers of the skin.
- Pubic lice, which are small insects that live on humans and survive by feeding on blood.
- Yeast infection , which may cause a rash in the moist skin folds of the vaginal area.
- Psoriasis, which causes raised red or white patches topped with silvery, scaling skin. The patches are most common on the knees, elbows, scalp, tailbone, and back, but may appear anywhere on the body .
Also Check: Zinc Oxide For Eczema On Face
When To See A Doctor About Vaginal Itching
Many people get a bit of vaginal itchiness from time to time. However, in addition to the advice given about specific conditions above, you should speak to your doctor if:
- youre itchy or sore
- the itching doesnt go away
- it keeps coming back
- you get bleeding between periods or after having sex
- it hurts when you pee
- you have pain in the area between your tummy and thighs
- you notice changes in your vaginal discharge in colour, smell or texture
- you are getting more discharge than usual
An itchy vagina can also be caused by a sexually transmitted infection like trichomoniasis or chlamydia. Other symptoms include yellow, green or smelly discharge and pain when peeing or having sex. If you do not want to see your doctor, go to your local genitourinary medicine clinic, where they will be able to test and treat your infection.
How Long Does It Take Vulvar Dermatitis To Heal
The amount of time it takes vulvar dermatitis to heal will depend on the cause.
For example, if caused by irritation from a product or clothing, the symptoms will likely resolve within one to two weeks after removing the irritant.
If caused by an infection, symptoms should start to get better within one to two weeks of treatment. However, symptoms could remain for a month or longer.
Recommended Reading: Tips For Eczema Flare Ups
If Your Swelling Is Painless But Growing Slowly You Probably Have A Bartholins Cyst
A Bartholins gland cyst begins as a bit of swelling inside your labia, next to the opening of your vagina.
One of the glands that keeps you lubed up can get infected, slowly filling with pus almost like cystic acne, but down in your lady bits instead of on your face.
Bartholins cysts dont usually hurt much except during sex. As the infection grows, youll notice more discomfort and redness.
Depending on the severity, cysts can be treated with pain relievers or outpatient removal procedures.
Why Is My Gynecologist Not Recognizing It As Vaginal Eczema
Because gynecologists arent trained to be dermatologists. It is really as simple as that. They lack training in diagnosing for skin-related conditions and instead will often try to find the diagnosis in relation to your sexual health.
What happens is that many women walk away with the diagnosis of vulvodynia , when in reality they are suffering from vaginal eczema.
Read Also: Can Apple Cider Vinegar Help With Eczema
If Your Labia Or Vagina Is Red And Raw You Might Have Lichen Planus
Lichen planus happens when your immune system freaks out and attacks your mucous membranes.
Though the painful redness, whitened skin patches, and burning during sex might make you think theres something seriously wrong, lichen planus is treatable. Its also not contagious.
Most doctors prescribe topical steroids for lichen planus. Since the condition can cause scarring and damage over time, its important to get treated ASAP.
Theres a tiny risk of squamous cell carcinoma with this condition, so keep your doctor in the loop if the rash gets worse.
How To Prevent Vulvar Dermatitis
Vulvar dermatitis cannot always be prevented, but there are some things you can do to decrease your chances of getting it.
- Avoid irritating products such as harsh laundry detergents, fragranced soaps, scented bath products, bath bombs, scented tampons or pads, douches, fragranced lube, spermicide lube, and condoms with harsh lubricants.
- Practice safe sex to lower your risk of contracting an STI.
- Wear loose-fitting, breathable, or moisture-wicking clothing.
- Avoid washing your vaginal area too frequently aim for once a day, and use a mild soap and warm water.
- Remove wet or sweaty clothing and change into dry clothing quickly after swimming or working out.
You May Like: How To Get Rid Of Skin Eczema
Getting A Diagnosis For Genital Eczema
The genital region is at risk of the scope of skin issues, many of them accidentally self-caused. You may routinely spoil your face and strive to keep it hydrated, youthful, and eczema-free, yet what have you done of late for the more touchy skin of your genitals.
Many people think no more than itch is just yeast infection. But with age and the decrease in collagen production, men and women are progressively inclined to an assortment of conditions that aggravate the genitals, including eczema. And genital eczema isnt getting the consideration it needs and people arent getting the help they should be getting.
Genital skin conditions are very treatable however, the treatment relies upon a particular reason. Whats more, recognizing the fundamental cause can be exceptionally difficult.
Inform your clinician concerning some other past or present medical problems and any skin issues somewhere else on your body. For instance, psoriasis in any place on the body raises the danger of a genital condition known as lichen sclerosus. Lichen, as a term connected to skin issues, alludes to skin sores that look like lichen on rocks.
Crohns disease, an extremely irritating intestinal issue, may cause abscesses or depleting fistulas in the genital region, and vulvar skin issues, including eczema, is regularly one of its initial indications.
What Is Vulvar Dermatitis

Vulvar dermatitis is when the folds of skin around the vagina become inflamed and irritated. The area can be painful, itchy, and red. The inflammation is sometimes called vulvitis. The soft skin folds of the vulva are designed to stay moist and warm, making them susceptible to irritation or infection.
Dermatitis can develop anywhere on the body. It is caused by irritants, such as hygiene products, clothing, bacteria, yeast, or viruses, coming into contact with the skin.
Your symptoms could also be caused by another condition or simply be your body’s response to exposure to an irritant.
Vulvar dermatitis can affect people of any age. However, young people who have not started their periods yet and people who are postmenopausal are more likely to develop it.
You May Like: Best Face Sunscreen For Eczema
How To Treat Eczema In The Genital Region
- Post author:Cameron Pell, PhD, RD
Ive experienced irritating skin in the genital region for a good part of my life. Eczema was most common and was extremely uncomfortable. I know the pain if you are going through it also. With this post, I hope to help you heal it and prevent it from coming back for life. How to treat eczema in the genital region?
To treat eczema in the genital region, first, see a doctor who will confirm whether it is eczema or a different issue. The doctor should then prescribe a mild topical steroid or emollient to reduce inflammation. Shower or bathe each morning or night, pat dry after, apply the topical steroid leaving no excess.
Theres much more to take into consideration when treating eczema in the genital area. For example, do not overuse steroid cream or ointment to avoid thinning the skin. The skin in the genital region can be quite sensitive and thin, so you dont want to use a strong steroid cream.
Your doctor will prescribe a mild dose as the genital region is so sensitive. Be wary of self-treating. And watch out for the many, many harmful everyday products that may be causing the inflamed skin.
Read on to learn more about how to treat eczema in the genital region and prevent it from recurring!
Diagnosis And Treatment Of Vulvar Dermatitis
If you think you may have vulvar dermatitis, schedule an appointment with your doctor. During your visit, theyâll ask you about your symptoms, if you have a history of eczema, any allergies you have, what your vulvar cleaning habits are, and what products you use around your vagina.
Then, your doctor will do an exam of the skin around your vagina. Theyâll look for skin changes such as cracking, thickening, redness, or scaling. They may also test a sample of your vaginal discharge to rule out infection.
If your doctor finds that you have eczema on your vulva, theyâll suggest the next steps for treatment. Itâs best to go with your doctorâs recommendations rather than over-the-counter methods since these might have additional allergens or irritants in them.
Your doctor might prescribe a cream to treat your eczema. You should apply the cream to your vulva as often as instructed by your doctor. While you use it, youâll want to keep stronger soaps and cosmetic washes away from your vaginal area.
Your doctor may also give you a topical steroid. The skin on your vulva will absorb this medication quickly, so itâs important that you use it carefully and as directed. Usually, you should only use these medications once or twice a day. Sometimes your doctor will prescribe an antibiotic with your steroid cream as well. Make sure you follow the directions to avoid further eczema flares.
Read Also: How To Control Baby Eczema
Cancerous Conditions Of The Vulva
Vulvar intraepithelial neoplasia is a pre-cancerous condition of the vulva. The affected cells divide quickly and erratically, but could stay benign for many years. Vulvar cancer is classified according to its cell of origin. This can include:
- squamous cell carcinoma originating in the skin cells. This type accounts for about 90 per cent of cases
- melanoma originating in the pigment cells deeper in the skin. This type accounts for about five per cent of cases
- adenocarcinoma originating from the Bartholins glands, the structures that supply lubricant. This type accounts for less than one per cent of cases
- sarcoma originating from fat cells. This type is very rare
- lymphoma originating from the immune cells. This type is very rare
- basal cell carcinoma a form of skin cancer. This type is very rare.
Is It An Sti Or Genital Eczema
Although the symptoms of genital eczema are similar to those of some sexually transmitted infections , there are some signs that an infection is to blame for the itching and irritation. If you notice any odor, discharge, bleeding, or signs of infection such as a fever or body aches, its more likely that you have an STI, not genital eczema.
Also Check: Eczema Treatment For Babies Home Remedies
Stress And Vulva Dermatitis
img source: alighahary.ca
Stress is known to trigger many skin condition eczema not excluded. Stress can lead to a decrease or increase in levels of certain hormones and this can trigger it. To many people, the symptoms of eczema usually aggravate when they have stress. Some people also get stressed if they discovered they have this skin condition and this can worsen the situation. See your GP to discover how to manage stress.
If You Cant Stop Scratching An Invisible Rash You Probably Have Neurodermatitis
Neurodermatitis isnt your run-of-the-mill rash. It starts with a normal patch of skin like a spot on your labia, for instance that itches like mad.
Eventually, your skin gets thick and leathery because of nonstop scratching. Scratching irritates your nerve endings, which makes your skin itch all over again. Its a vicious, invisible cycle.
Doctors arent sure what causes neurodermatitis, but it might be triggered by something as simple as a bug bite or mild jock itch.
Sometimes an OTC drugstore cream is enough to kick neurodermatitis to the curb, but you should see your dermatologist if the itching doesnt let up.
You May Like: Best Shampoo For Eczema Child
What Are The Signs
- Mild to severe burning and/or itching of the vulva
- Vulvar redness and swelling
- Raw feeling due to the vulvar irritation
- Damp or wet feeling due to weeping of the irritated skin surface
- Some women mistake this dampness as vaginal discharge.
What Causes Vulva And Vagina Irritation
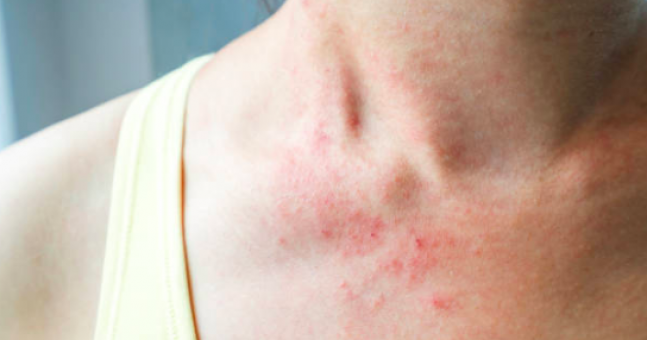
Many things can cause irritation including:
- an imbalance of the bacteria and microorganisms that normally live inside the vagina
- lubricants and spermicides and latex products used during sex, such as condoms
- hormonal changes, such as after having a baby or during menopause
- a skin condition such as dermatitis or eczema
- excess washing or vaginal douching
- allergy or a reaction to hygiene products such as soaps, shower gels, shampoos, or hygiene sprays
- disinfectants, antiseptics and ointments
- sanitary pads or tampons, condoms
- sweating
- swimming in a chlorine pool
- wearing new underwear, especially if it is not made of cotton
- very rarely, vulval cancer
Groin irritation can also be due to a build-up of sweat from not washing and drying your groin properly, or from over-washing or scrubbing the area.
You May Like: How To Lighten Eczema Scars
Hot And Cold Temperatures
Weather is another major factor that can lead to dermatitis vulvar. To many individuals, extreme cold can cause breakouts since the skin gets too dry. When your skin gets too dry, it can easily become brittle, scaly, rough, or tight, which can lead to an eczema flare-up.
On the other side, hot weather can lead to vulva sweating and sweat can easily irritate the vulva skin. In both cases, moisturizers and humidifiers are very significant.
What Is Contact Dermatitis Of The Vulva
It is a skin problem that causes:
- Vulvar or vaginal burning
- Irritation
- Itching
It happens when the vulvar skin becomes sensitive to products called contact irritants. This can be sudden or get worse slowly with repeated exposure to irritants, such as:
- Laundry detergents
- Fabric softeners and dryer sheets
- Body soaps
- Feminine products
Recommended Reading: Ultraviolet Light Therapy For Eczema
If Your Vulva Is Swollen And Itchy Its Probably Vaginitis
Ever had a yeast infection? Congrats, that was vaginitis! Vaginitis is an umbrella term for infections or inflammation around your lady parts.
The American College of Obstetricians and Gynecologists reports that your vaginas lining gets swollen and irritated when your bodys yeast and bacteria gets out of whack.
Antibiotics, douching, and spermicide all up your risk factor since they mess with your bodys delicate balance. Once things swell up and start to itch, youll probably notice other symptoms such as:
- fishy-smelling discharge
- yellow, grey, green, or lumpy discharge
- pain during sex and peeing
- vaginal bleeding
Most vaginitis episodes can be treated with over-the-counter creams, but sometimes prescription antibiotics or antifungals are necessary.