Edema And Blister Formation
Eosinophils may contribute to edema by releasing eosinophil granule proteins, as well as by the production of leukotrienes that have direct vasodilatory effects on blood vessels or indirectly via stimulation of mast cells and basophils . Eosinophil infiltration in the skin and lining along the dermal-epidermal junction are observed in bullous pemphigoid , an autoimmune-bullous disease. In the presence of BP autoantibodies eosinophils upon activation by IL-5 were shown to directly contribute to blister formation using an ex vivo skin model . Adhesion, Fc receptor activation, elevated ROS production, and EET formation by eosinophils have been shown to be involved in dermal-epidermal separation . Furthermore, ECP and EDN have been reported to exert cytotoxic effects on keratinocytes and cause cell-matrix detachment .
Study Design And Data Source
In this cross-sectional study conducted from 1 January 2018 to 30 September 2020, blood test results, including the WBC count, peripheral eosinophil count, peripheral basophil/WBC percentage, and IgE level, were collected from patients diagnosed with the 4 diseases of AD, BP, DRESS, and HES . The AD patients were diagnosed according to the criteria of Hanifin , and the BP patients were diagnosed by pathological biopsy. When the peripheral eosinophil count exceeded 1,500 and other diseases were excluded, patients were considered to have HES . The DRESS patients were selected based on the Japanese Consensus Group diagnostic criteria . The healthy controls comprised 621 randomly selected volunteers and were compared with 115 AD patients, 75 BP patients, 55 DRESS patients, and 119 HES patients. The sample size was decided by the number of cases in the area.
Eosinophilic Asthma Diagnosis Tests Used
- Blood Eosinophil Count Test: A blood test used to measure levels of eosinophils in your blood. Its a simple blood draw and there is no need to fast before this blood test. Also, it can only measure the eosinophil count in blood and not in lungs.
- Sputum Eosinophil Count Test: This test is to measure eosinophils in your sputum, a mixture of coughed mucus and saliva. The practicality of the test is bit deniable as few people have trouble generating a sample however the accuracy of this test is unquestionable.
- Bronchial Biopsy Test: This test is more invasive than the others and less likely to be used for the initial diagnosis.
You May Like: Eczema Dos And Don Ts
Box : Primary Eosinophilias
Idiopathic hypereosinophilic syndrome: sustained peripheral eosinophilia at greater than 1500 cells/µL with associated end-organ damage.
Lymphoproliferative hypereosinophilic syndrome: sustained peripheral eosinophilia at greater than 1500 cell/µL, often associated with rash, aberrant T-cell immunophenotypic profile, often steroid responsive.
Myeloproliferative hypereosinophilic syndrome: sustained peripheral eosinophilia at greater than 1500 cell/µL, often features of splenomegaly, heart related complications, and thrombosis. Can have associated FIP1L1-PDGFRA and other mutations and are often steroid resistant. Patients can be considered to have a diagnosis of chronic eosinophilic leukemia.
Episodic eosinophilia associated with angioedema : cyclical fevers, swelling, hives, pruritus, marked eosinophilia, and IgM elevation. Aberrant T-cell phenotypes often associated.
Be Prepared For A Doctors Appointment Beforehand:
Sufferers with a suspected asthma or asthma will be referred to a pulmonologist or an allergist. So, we have prepared a list of tips that may prove helpful to get you prepared for the doctors appointment:
- Dont forget to keep a proper record of the symptoms you are having, even if they are seemingly unrelated.
- Remember to maintain and bring a list of medications you are taking be it vitamins, over the counter medications, or the supplements.
Prepare list of questions that you have in your mind like:
- What tests can be performed For Eosinophilic Asthma?
- How should I use my medications?
- What are the triggers for asthma flare ups?
- Can I do anything to reduce the risk of having an asthma attack?
- Do I need to change my diet?
- Can I restrict the use of inhalers?
- Is there any elimination diet?
- How often do I need follow-up care?
Recommended Reading: Is Tea Tree Good For Eczema
How To Treat Eosinophilia
Usually, if you have a high eosinophil count, the specific cause of eosinophilia is treated. For example, asthma is treated with medications that help prevent flare-ups and symptoms. Inflammatory diseases are often treated with immunosuppressants, and cancer is often treated with chemotherapy or other interventions, such as a bone marrow transplant.
And, in some situations, you might also need treatment to reduce your eosinophil count. Treatment of eosinophilia can include steroids, myelosuppressive medications, and immunomodulators. These treatments reduce inflammation.
There are also medications that can specifically target eosinophilia to reduce the effects of these white blood cells. These include the monoclonal antibodies, mepolizumab, reslizumab, and benralizumab.
Evaluation Of Possible Pid In A Patient With Eosinophilia
Many patients with eosinophilia will be explained by secondary causes such as parasitic infections, allergies, or hematological problems which are well reviewed elsewhere . If PID is being considered as a potential cause of eosinophilia, a wide range of PIDs have been associated with eosinophilia including disorders of Tcell development and signalling, cytokine signalling, cytoskeletal formation, autoimmunity, thymic development, innate immunity, humoral immunity and phagocytic function.
The history and physical examination may reveal clues which lead to likely diagnoses and further immune evaluation. Despite lack of sensitive and or specific signs and symptoms in respect to PIDs, many red flags including specific patterns of infections, autoimmunity, need for intravenous antibiotics, and prolonged oral antibiotics use with little effects have been previously reviewed . Additionally, a detailed practice parameter for the evaluation of PID was recently published . A patient history including infections, autoimmunity, malignancy and a review of systems including the presence of constitutional symptoms, allergies, and diarrhea may assist in deciding the likelihood of an immunodeficiency. A family history including consanguinity, early deaths and malignancy will also assist in evaluating for serious causes. The physical exam may note growth parameters, dysmorphism, skin abnormalities, thrush, lymphatic tissue, skin/nail abnormalities and neurological features.
Fig. 1
Read Also: What Is Eczema Prone Skin
When To See A Healthcare Provider
You would not know that you have eosinophilia or any other sign of a blood abnormality unless you have a blood test.
You should see a healthcare provider if you begin to:
- Feel sick, run down, or excessively tired
- Notice a lump or swelling on your body
- Experience symptoms of an allergic reaction, such as coughing, wheezing, or a rash
Get urgent medical attention if you have swelling of your throat or mouth, or if you have trouble breathing.
Causes Of Low Eosinophil Levels
1) Infections
When there is an acute infection, several substances are secreted to attract eosinophils from blood to affected tissues. This causes blood eosinophil levels to drop rapidly. A complete absence of eosinophils is also seen in serious infections such as sepsis .
2) Cushings syndrome
Cushings syndrome occurs after a person is exposed to high cortisol levels for a long time, either due to an underlying health condition or long-term cortisol therapy. Cortisol suppresses the immune system and lowers eosinophil levels in the blood .
3) Drugs
Glucocorticoids are anti-inflammatory drugs related to cortisol. They diminish the production, survival, and function of eosinophils .
Some drugs, including glucocorticoids, used to suppress the immune system, and theophylline, used to prevent and treat wheezing, shortness of breath, and chest tightness caused by asthma, chronic bronchitis, and other lung diseases .
Read Also: Baby Eczema On Legs Treatment
Parameters And Disease Severity
Basophils and IgE
The basophil/WBC ratio and IgE levels were measured only twice, once before admission and once 1 week after discharge. There were no sufficient data collected in the BP, DRESS, and control groups to support the analysis. Using the related-samples Wilcoxon signed rank test, IgE and basophil/WBC ratio of 3 samples from the AD group, IgE of 4 samples from the HES group, and the basophil/WBC ratio of 5 samples from the HES group were calculated. The IgE level and basophil/WBC ratio did not change significantly after discharge.
Eosinophils and WBCs
Eosinophils and WBCs were measured 3 times: before admission, 1 week after discharge, and 2 weeks after discharge. There were 62 samples from the AD group, 61 from the BP group, 52 from the HES group, and 15 from the DRESS group at 1 week post discharge, but at 2 weeks post discharge, there were only 10 from the AD group, 3 from the BP group, 26 from the HES group, and 8 from the DRESS group. When all of the data collected from 3 repeated measurements were considered together, both eosinophils and WBCs count did not satisfy the requirements for spherical symmetry, and the multivariate tests demonstrated no significant difference, which may be the result of the limited sample size.
How Do You Reduce Eosinophils
Glucocorticoids are the most effective current therapy used to reduce eosinophil numbers in the blood and tissue , but the pleiotropic effects of corticosteroids can result in potentially harmful side effects and limit their therapeutic use.
Is eosinophilia infectious or non-infectious?
Keywords: Eosinophilia, infection, fever, travel, immigrant, refugee I. Introduction Eosinophilia can be caused by both infectious and non-infectious processes, many of which may be clinically indistinguishable.
Read Also: Dr Aron Eczema Treatment Discussion Group
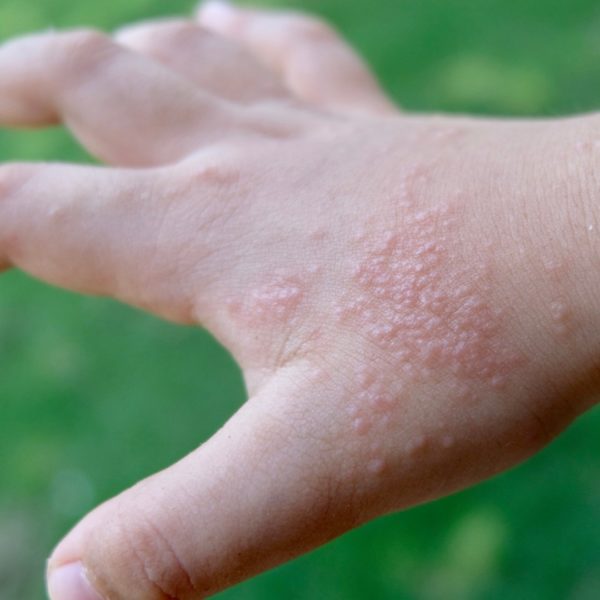
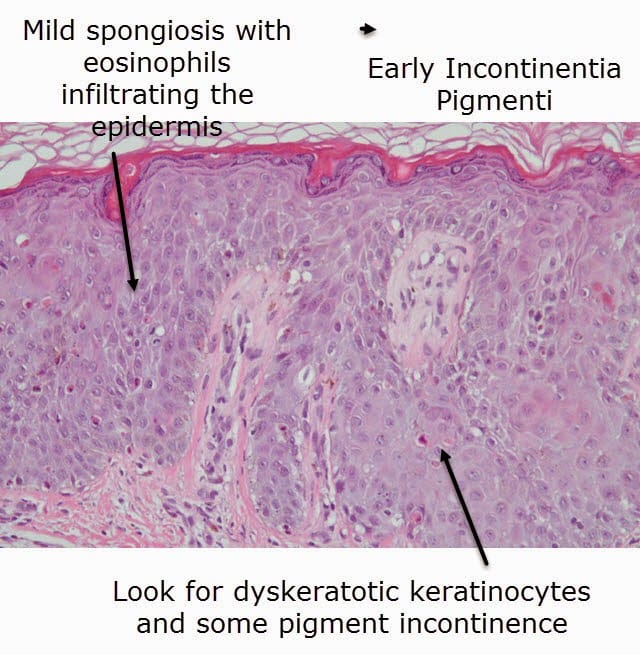
Clinical Patterns Of Eosinophilic Dermatoses
Next, we will present the spectrum of eosinophilic dermatoses based on their clinical presentations and provide current knowledge on the pathogenesis with special focus on a role of eosinophils.
Fig. 2
In DRESS, T cells recognizing drug-derived haptens expand, a process that can be associated with reactivation of certain viruses such as HHV6, herpes virus 1, EBV and cytomegalovirus . IL-5 is considered the main driver of eosinophil expansion and activation leading to organ damage and dysfunction in DRESS . The efficacy of antibodies targeting the IL-5 / IL-5 receptor axis in severe DRESS are an evidence for the key role of eosinophils in the pathogenesis .
Attack Of The Eosinophil
Several immune diseases involve inappropriate activation of immune cells called eosinophils. These include a form of allergic eczema , a form of asthma , a set of gastrointestinal disorders , and chronic rhinosinusitis .
These are not considered autoimmune diseases, because autoimmune disease involves the production of antibodies against the patients own tissues. Instead, eosinophilic diseases are more like exacerbated allergies or an atypical allergic response to molecules that most people do not find harmful. Unfortunately, these molecules tend to be ones encountered routinely and are present in food or the environment.
Eosinophils are a type of white blood cell. They are especially important for fighting parasitic infections, but they also participate in fighting bacteria too. In a healthy person, normally less than 1% of the white blood cells are eosinophils. If eosinophils exceed 500 per microliter of blood, then the doctor will look for a condition causing the increase. It could be an indication of an infection, a reaction to a drug, or an eosinophilic disease. Often diagnosing a tissue-specific eosinophilic disease requires taking a biopsy of the affected tissue, like biopsies of the esophagus to diagnose eosinophilic esophagitis.
Figure 1. Types of white blood cells. Credit: OpenStax College . More details
Don’t Miss: Best Sheets For Eczema Sufferers
Not Classified By Iuis
PGM3-deficiency
PGM3 deficiency presents with hyper-IgElike features, atopy, autoimmunity and neurocognitive impairment . PGM3 is involved in posttranslational alterations necessary for functioning of many proteins and lipids . Eosinophilia, inverted CD4/CD8 ratio, and increased IgE level were described .
Roifman syndrome
Roifman syndrome is characterized by bone dysplasia, growth retardation, retinal dystrophy and humoral immunodeficiency . In the original description of Roifman syndrome 3/4 patients had eosinophilia .
Parameters In Different Groups
WBC
The control group had a significantly lower peripheral WBC count than the other groups , with no significant difference among the 4 disease groups .
Figure 2
Eosinophils
Both the peripheral eosinophil count and eosinophil/WBC ratio were compared among the groups. These 2 parameters showed almost the same tendency among groups, with slight differences. The control group had the lowest eosinophil count and eosinophil/WBC ratio, similar to the BP group. Participants with DRESS had significantly higher levels than the control group and similar levels to the BP group. In contrast, the HES and AD groups had significantly higher levels than the other 3 groups .
Basophils
Both the peripheral basophil count and the basophil/WBC ratio were calculated. The control group had a significantly higher basophil count than the other groups, with no significant difference among the 4 disease groups .
Although the 4 disease groups seemed similar in terms of both peripheral WBC and basophil counts, the basophil/WBC ratios were different. Only the pairwise comparisons NâAD, ADâHES, HESâDRESS, and DRESSâBP presented no significant difference. This finding, combined with the information from the box plot, indicated that the disease groups can be ordered from highest to lowest as NâADâHESâDRESSâBP, with only the adjacent 2 groups showing similar values .
IgE
Eosinophil/basophil ratio
Figure 3
Recommended Reading: Do Kids Grow Out Of Eczema
Symptoms Of High Eosinophils
Symptoms of higher than preferred eosinophils are likely what will cause an individual to seek medical treatment in the first instance.
The range of possible symptoms and their severity varies, in harmony with the vast array of underlying causes for eosinophilia.
Many of these symptoms, such as weight loss, fevers or night sweats, cough, chest pain, skin rashes or itching, swelling, stomach aches, diarrhea, fatigue, pain, and weakness, can likewise be indicative of other disorders unrelated to eosinophils.
Thus, while symptoms are vital indications that indicate a person should seek medical guidance, they are not reliable indicators of high eosinophil levels.
What Is Eosinophilic Asthma
Eosinophils are a type of disease-fighting white blood cells in your blood. These are the natural part of your bodys immune system. They fight against the attacks of invading bacterias and other infections.
People who are suffering from eosinophilic asthma have high number of these white blood cells that are responsible for the inflammation and swelling in the respiratory system.
Due to the factors stated above, eosinophilic asthma i.e a type of asthma may also develop in certain individuals. It is considered as the subtype of asthma marked by elevated levels of eosinophils in the blood, tissues or the mucus that generally causes spasms in the bronchial tubes, making it difficult to breathe.
Eosinophilic Asthma is a rare medical condition. As per the researchers approximately 5 percent of all adults with asthma are suffering from EA . It is difficult to treat it but proper measures can be taken to manage the respiratory condition.
Also Check: Dandruff Or Eczema On Scalp
What Are Eosinophils And What Do They Do
Eosinophils are a type of white blood cell. They play a key role in the immune system. They act to defeat pathogens, such as bacteria, viruses, fungi, and parasites. They also react to perceived threats, for example, during an allergic reaction. While essential for defending the body, their activity can cause inflammation. This can sometimes lead to further issues.
Descriptive Analysis By Age And Gender
Except for BPâHES, all other pairwise comparisons demonstrated significant differences in age . All of the figures in this article were created by Prism 8 .
Figure 1
The majority of our healthy controls were young people. To test the possible interference caused by the age of the controls, the data were divided by age into 5 groups from 0 to 100, with each group representing a span of 20 years. There was no difference in the distribution of age groups within each group, indicating that age had little impact on the results of this study.
Pearsonâs chi-square test showed that only the HES group had a significantly larger proportion of male participants .
Also Check: How To Get Rid Of Black Eczema Marks
What Does High Eos Mean In A Blood Test
Eosinophils are a type of disease-fighting white blood cell. This condition most often indicates a parasitic infection, an allergic reaction or cancer. You can have high levels of eosinophils in your blood or in tissues at the site of an infection or inflammation .
What autoimmune diseases cause high eosinophils?
Specific diseases and conditions that can result in blood or tissue eosinophilia include:
- Acute myelogenous leukemia
- Easy bruising or bleeding, such as nosebleeds or bleeding gums.
What are the symptoms of leukemia in a child?
Miscellaneous Entities Associated With Eosinophilia

Rejection of transplanted solid organs including liver, pancreas, kidney, and heart have been associated with peripheral and organ-specific eosinophilia. The eosinophilia can be moderate to severe.28
Chronic graft-versus-host disease after hematopoietic stem cell transplantation has also caused peripheral eosinophilia. Level of skin involvement and severity of graft-versus-host disease could not be reliably predicted based on the presence of eosinophilia in 1 cohort of patients.29
Kimura disease, a disease of mostly Asian males, is defined as masslike lymph node or subcutaneous tissue swelling mainly in the head and neck, peripheral eosinophilia, IgE elevation, and eosinophilic pathologic infiltrates with follicular hyperplasia and proliferation of postcapillary venules in biopsies. Surgical excision and steroid therapy is often used.30
Epithelioid hemangioma, also known as angiolymphoid hyperplasia with eosinophilia, also most often affects the head and neck, especially on and around the auricles. It is seen in all races and both sexes, affects the dermis or epidermis, and is thought of as a benign vascular proliferative disease. Excision and laser therapy seem to be the most often used treatment modalities, often undertaken for cosmetic reasons.31 Peripheral eosinophilia is variable and IgE elevation is not common.
Recommended Reading: Do You Have To Be Born With Eczema
Common Causes Of High Eosinophils
Eosinophilia, or the recruitment of a disproportionate number of eosinophils to a specific body site, can be caused by various factors.
Allergic reactions, adrenal conditions, parasites, fungal diseases, toxicity in the body, tumors, and autoimmune and endocrine disorders, can all result in elevated eosinophil levels.
The comprehensive list of conditions that can lead to eosinophilia includes asthma, cancer, atopic dermatitis or eczema, acute myelogenous leukemia , allergic rhinitis or hay fever, and Crohns disease, Hodgkins lymphoma, and roundworm infections such as trichinosis and ascariasis.
Parasitic diseases and infections like lymphatic filariasis, and allergic reactions to medications, are two of the more common causes of high eosinophils.
Eosinophilia can also be from an undeterminable origin, with studies confirming a high level of unproven etiology, or manner of causation, in patients with eosinophilia symptoms.