If You Are Able To Confirm That The Patient Has Eczema Herpeticum What Treatment Should Be Initiated
Treatment with systemic antiviral agents should be initiated as soon as a diagnosis of Kaposi varicelliform eruption is suspected.
Oral acyclovir is the preferred first-line treatment in otherwise healthy, immunocompetent pediatric patients, at a dose of 30 mg/kg/d divided five times daily for 7-10 days.
Intravenous acyclovir is recommended for patients with systemic involvement or in patients who are immunocompromised . Foscarnet should be used in patients with acyclovir-resistant infection. Valacyclovir is efficacious and can be dosed only twice daily, an advantage over daily multiple dosing of acyclovir. However, it is cost-prohibitive for some patients.
Two topical ophthalmic preparations, trifluridine and vidarabine, are available for use in patients with ophthalmic involvement. Immediate opthalmologic consultation is recommended for any patient with potential ocular infection.
How Can Eczema Herpeticum Be Prevented
Patients with a known preexisting dermatosis should be counseled about the signs and symptoms of Kaposi varicelliform eruption. In cases of recurrent herpes labialis or herpes genitalis, prophylactic therapy with daily systemic antiviral agents may be indicated. These patients should also be treated with preprocedure systemic antiviral therapy before scheduled dermabrasion or other cutaneous procedures that will disrupt the epidermal barrier.
Vaccination is not available for HSV, and genetic counseling for potential fillaggrin or other gene mutations is not currently available.
What Laboratory Studies Should You Request To Help Confirm The Diagnosis How Should You Interpret The Results
Evaluation of blister fluid or infected keratinocytes confirms the diagnosis. If keratinocytes are being sampled, they should be obtained by vigorous scraping of the base of a fresh or recently developed lesion to increase the sensitivity of the test. If there is overlying crust, it should be removed before sampling so that the base of the erosion can be accessed.
There are several diagnostic tests available:
Direct fluorescent antibody testing is accurate can distinguish between HSV 1, HSV 2, and varicella and results can be obtained rapidly
Viral culture is also diagnostic. Results are accurate and reliable, and can distinguish between different viruses. However, results are slow .
Tzanck smear requires a skilled observer to interpret, but results are immediate on examination of the smear. A Tzanck preparation is performed by placing scrapings from the base of a blister or erosion on a glass slide, staining with Wright or Giemsa stain, and examining under light microscopy for characteristic Tzanck cells . Tzanck cells can be seen in herpes, varicella, and cytomegalovirus infections.
Polymerase chain reaction may be helpful in when the cutaneous lesions are old or atypical and viral particles are few in number.
Read Also: Clear Up Eczema On Face
Severe And Immunocompromised Cases
People with severe eczema herpeticum or those with compromised immune systems are hospitalized for monitored treatment.
During hospitalization, intravenous injections of acyclovir are administered every eight hours. The individual is then transitioned to oral acyclovir, once symptoms have improved and their lesions have started to heal into crusts.
While still under professional care, emollients and cool compresses are applied to help relieve the symptoms of eczema herpeticum.
What Are The Clinical Features Of Eczema Herpeticum
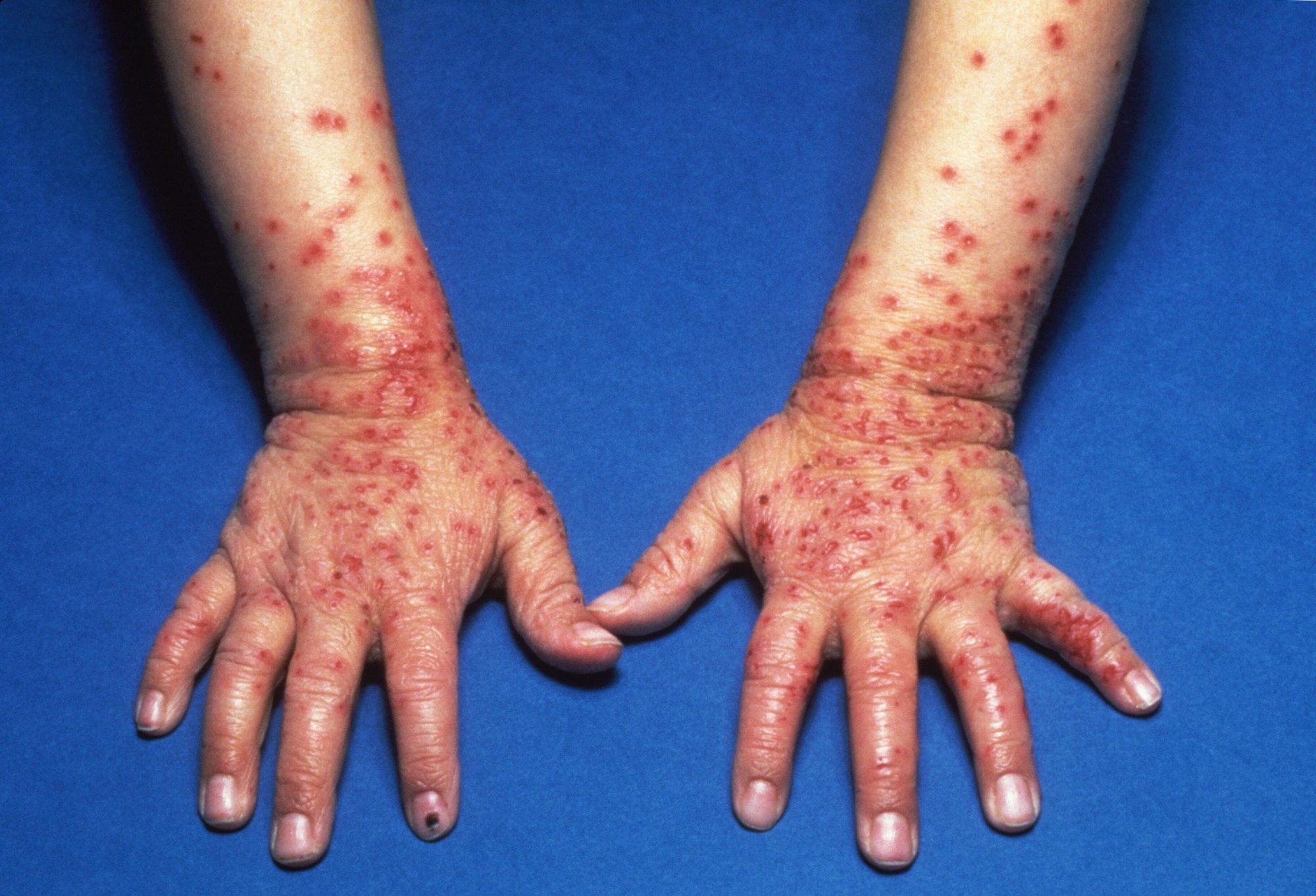
Eczema herpeticum starts with clusters of itchy and painful blisters. It may affect any site but is most often seen on face and neck. Blisters can occur in normal skin or sites actively or previously affected by atopic dermatitis or another skin disease. New patches form and spread over 710 days and may rarely be widely disseminated throughout the body.
The patient is unwell, with fever and swollen local lymph nodes.
- The blisters are monomorphic, that is, they all appear similar to each other.
- They may be filled with clear yellow fluid or thick purulent material.
- They are often blood-stained i.e., red, purple or black.
- New blisters have central dimples .
- They may weep or bleed.
- Older blisters crust over and form sores
- Lesions heal over 26 weeks.
- In severe cases where the skin has been destroyed by infection, small white scars may persist long term.
Secondary bacterial infection with staphylococci or streptococci may lead to impetigo and cellulitis.
Severe eczema herpeticum may affect multiple organs, including the eyes, brain, lung, and liver. It can rarely be fatal.
Eczema herpeticum
Recommended Reading: Diet And Eczema In Toddlers
For People Who Are Hospitalized
At the hospital, certain precautions are taken to prevent spreading the virus, including isolation. Health care providers use face masks and gowns when caring for hospitalized individuals. Individuals are constantly monitored for secondary bacterial superinfection, and systemic antibiotics are administered as required.
What Complications Might You Expect From The Disease Or Treatment Of The Disease
Kaposi varicelliform eruption is considered by many to be a true dermatologic emergency because of the potential for irreversible ocular scarring . It can also lead to multisystem organ involvement in patients who are immunocompromised or have severe primary infection. Patients with Kaposi varicelliform eruption are also likely to experience secondary staphylococcal infection of the affected skin.
Read Also: Best Body Moisturizer For Eczema
Etiology Of Eczema Herpeticum
| The safety and scientific validity of this study is the responsibility of the study sponsor and investigators. Listing a study does not mean it has been evaluated by the U.S. Federal Government. Read our disclaimer for details. |
| First Posted : February 1, 2017Last Update Posted : January 14, 2021 |
- Study Details
Atopic dermatitis, also called eczema, is a disease with dry, scaly, itchy skin. Those with atopic dermatitis may have complications from skin infections such as eczema herpeticum after herpes simplex virus infection. Symptoms of eczema herpeticum include fever and clusters of itchy blisters which crust over and form sores. Although exposure to HSV is widespread, most people clear the virus and only a subset of individuals with atopic dermatitis develop eczema herpeticum.
The purpose of this study is to determine why some individuals with atopic dermatitis are at higher risk for recurrent skin infections with HSV. The study team will compare how people with atopic dermatitis with a history of recurrent eczema herpeticum, people with atopic dermatitis without a history of eczema herpeticum, and people without atopic dermatitis respond to HSV.
| Eczema Herpeticum |
| Group/Cohort |
|---|
| Discovery Cohort |
The study will learn from this cohort:
Eczema Or Herpes: How Can You Tell The Difference
Its often easy to distinguish between eczema and herpes because of their distinctly different symptoms. While herpes triggers defined blisters that burst and scab over, usually around the mouth or genitals, eczema causes rough, dry rashes in other areas of the body.
To distinguish between herpes and severe eczema that has produced open sores, consider the symptoms that occurred before the sores appeared and the location of the sores.
You May Like: How To Heal Eczema Without Steroids
Complications Of Eczema Herpeticum
Eczema herpeticum is potentially a very serious condition. Complications of this infection may include:
- Scarring from blisters
- Infection in the cornea of the eye known as herpetic keratitis, which left untreated, can lead to blindness
- In rare cases, organ failure and death if the virus spreads to the brain, lungs and liver
Immediate treatment for eczema herpeticum can reduce the risk of complications from the virus.
- National Eczema Association | 505 San Marin Drive, #B300 | Novato, CA 94945
- 415-499-3474 or 800-818-7546
NEA is a qualified 501 EIN 93-0988840
NEA is a qualified 501 EIN 93-0988840
Get the latest eczema news delivered to your inbox.
- Advances in research and treatments
- Lifestyle tips and hacks
Is Eczema Herpeticum Contagious
Eczema is not contagious like the flu or a cold, but it is often inherited or passed through genes. The most common type of eczema, called atopic dermatitis, occurs in about 8 in 10 children where both parents have the condition and in about 6 in 10 children where one parent has the condition. However, if the raw, irritated skin of eczema becomes infected, the infecting agent may be contagious. The exact cause of atopic dermatitis is not known, but because it often occurs in family members, it is felt that a persons inherited genes may play a role in its development.
Recommended Reading: Why Does My Eczema Itch So Bad
What Is Herpes Simplex Virus
Most people refer to herpes simplex viruses as herpes. These viruses transmit from one person to another and can cause painful or itchy blisters or open sores.
When sores or blisters appear, this is called a herpes outbreak. Many people have herpes but do not have symptoms or outbreaks, so they are unaware that they have the virus.
There are several types of herpes, but the two common ones are herpes simplex virus types 1 and 2.
Ongoing Controversies Regarding Etiology Diagnosis Treatment
Some authors have postulated that chronic topical corticosteroid or calcineurin inhibitor use in patients with atopic dermatitis may lead to increased risk of Kaposi varicelliform eruption, but this has not been proved.
No sponsor or advertiser has participated in, approved or paid for the content provided by Decision Support in Medicine LLC. The Licensed Content is the property of and copyrighted by DSM.
Also Check: Dr Richard Aron Eczema Treatment
Signs And Symptoms Of Eczema Herpeticum
- Clusters of small watery blisters that are itchy and painful
- Blisters that look red, purple or black or that ooze pus when they break open
Other symptoms:
- General malaise
- Swollen lymph nodes in the areas of the rash
In severe cases of infection, you can get complications from eczema herpeticum. Some people can get scarring from all of their blisters. If the virus gets near the eye, you can get an infection of the cornea of the eyeherpetic keratitis. Herpetic keratitis can lead to scarring and blindness if it is not recognized and treated. In people with a weak immune system, eczema herpeticum can be life-threatening the infection can spread via the bloodstream and lead to organ failure and death .
How Is Eczema Herpeticum Treated
Eczema herpeticum is considered an emergency. This is because it can spread quickly. So it must be treated correctly and quickly. If you or your child are diagnosed with eczema herpeticum you will normally be sent to hospital that day for advice from a specialist. In children it is quite common to be admitted to hospital while having the first few days of treatment. In adults, particularly if the infection is mild, it may be sufficient to take tablets and be reviewed by your doctor.
It is important not to be tempted to put a steroid cream on the eczema herpeticum. This will probably make it a lot worse. Many people have steroid creams at home, or have used them for their eczema in the past: you shouldn’t use them for a painful skin condition unless advised by your doctor.
Antiviral medicine such as aciclovir is usually very successful for treating eczema herpeticum. It may be given as a liquid or a tablet. For people who are too unwell to take it as a liquid or a tablet, it can be given by a drip .
Sometimes an antibiotic may be needed as well. This is because the damage to the skin makes you more likely to become infected by the bacteria normally harmlessly present on the skin as well. This is called a secondary bacterial infection.
Recommended Reading: Best Diaper Rash Cream For Eczema
What Are The Possible Outcomes Of Eczema Herpeticum
Kaposi varicelliform eruption has in past decades led to significant mortality. With widespread use of acyclovir, current mortality is estimated at approximately 10% and is most common in immunocompromised patients. Significant morbidity results from cutaneous scarring, keratoconjunctivitis, and subsequent ocular scarring and, rarely, multisystem organ involvement. For these reasons, treatment with systemic antiviral agents is recommended. The risks of complications from Kaposi varicelliform eruption far outweigh the risks from antiviral therapy, which is generally safe and well tolerated.
Causes Of Eczema Herpeticum
An eczema herpeticum happens when the herpes virus infects large areas of the skin. People with atopic dermatitis are more susceptible to skin infection in general, including eczema herpeticum. Eczema herpeticum can also appear in people who have contact dermatitis or seborrheic dermatitis. It is more common in infants and young children and those with severe atopic dermatitis.
The herpes simplex 1 virus is spread through skin-to-skin contact.
Recommended Reading: What’s The Best Remedy For Eczema
How Is Eczema Herpeticum Diagnosed
Eczema herpeticum is often confused with other skin infections. As it starts with just a few small red spots, it is often confused with chickenpox. The key difference to chickenpox here is that eczema herpeticum has lots of tiny red spots very close together, whereas chickenpox often has slightly larger red spots that are a bit further apart.
As eczema herpeticum is often on the face or around the mouth, it is often confused with impetigo . The difference is that a child with eczema herpeticum will often be generally unwell, with a fever, whereas with impetigo they don’t usually feel ill.
Sometimes the rapid appearance of the red spots of eczema herpeticum is confused with a simple flare-up of eczema. The key difference is that normal eczema is itchy whereas eczema herpeticum is painful.
If you think you or your child have eczema herpeticum it is vital that you see a doctor to check the diagnosis: eczema herpeticum needs to be treated correctly and promptly, otherwise it can become very serious.
Hospital specialists may take a small sample of the fluid in one of the spots and send it to the laboratory for testing. Specialist tests can show the herpes virus, which confirms the diagnosis. Most general family doctors do not have access to these tests: they are usually only available in hospital.
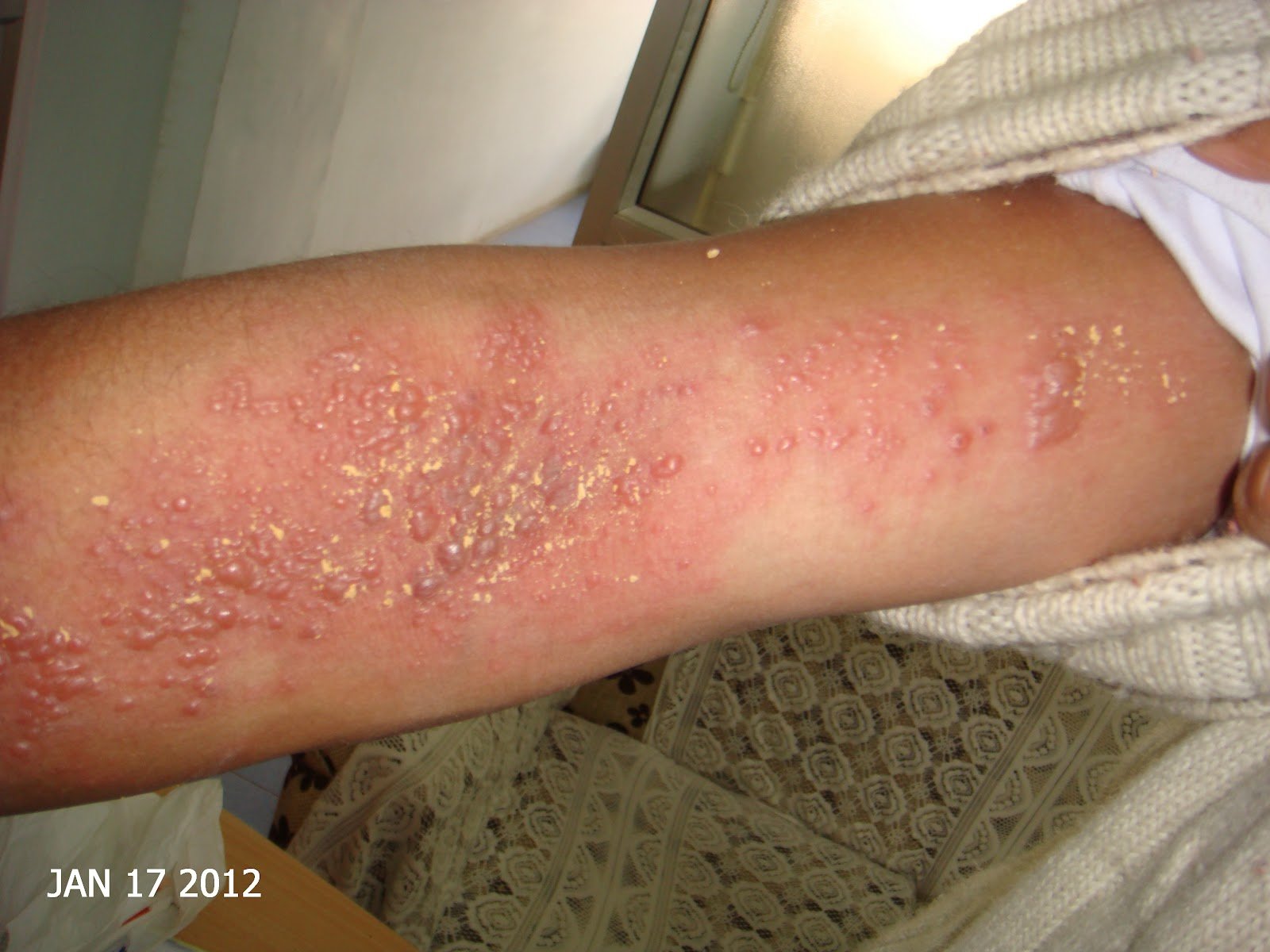
This photo shows the typical appearance of eczema herpeticum in a young child:
Enhancing Healthcare Team Outcomes
Eczema herpeticum is considered a medical emergency and should be treated promptly with systemic antivirals, as misdiagnosis and delay in treatment can result in serious complications. An ophthalmologic evaluation is warranted in cases of EH involving the face and eyelids. A dermatology consult may be beneficial to confirm the diagnosis. Clinicians should be aware of the risk factors associated with EH, including severe or poorly controlled atopic dermatitis, food and environmental allergies, asthma, the onset of atopic dermatitis before age five, and history of S. aureus and molluscum contagiosum infections.
Patients with systemic symptoms or widespread involvement should be promptly referred to the Emergency Department. To improve patient outcomes and prevent morbidity and mortality, healthcare providers should have a high index of suspicion for EH in patients with a history of atopic dermatitis presenting with a sudden onset, vesicular, monomorphic rash in areas of pre-existing dermatitis.
Don’t Miss: Prescription Strength Hydrocortisone Cream For Eczema
What Is The Evidence
Freyschmidt, EJ, Mathias, CB, Diaz, N. Skin inflammation arising from cutaneous regulatory T cell deficiency leads to impaired viral immune responses. J Immunol. vol. 185. 2010. pp. 1295-302.
Frisch, S, Siegfried, EC. The clinical spectrum and therapeutic challenge of eczema herpeticum. Pediatr Dermatol. vol. 28. 2011. pp. 46-52.
Gao, PS, Rafaels, NM, Hand, T. Fillaggrin mutations that confer risk of atopic dermatitis confer greater risk for eczema herpeticum. J Allergy Clin Immunol. vol. 124. 2009. pp. 507-13.
Goodyear, HM, MeLeish, P, Randall, S. Immunological studies of herpes simplex virus infection in children with atopic eczema. Br J Dermatol. vol. 134. 1996. pp. 85-93.
Hata, TR, Kotol, P, Boguniewicz, M. History of eczema herpeticum is associated with the inability to induce human beta-defensin -2, HBD-3 and cathelicidin in the skin of patients with atopic dermatitis. Br J Dermatol. vol. 163. 2010. pp. 659-61.
Symptoms Of Eczema Herpeticum
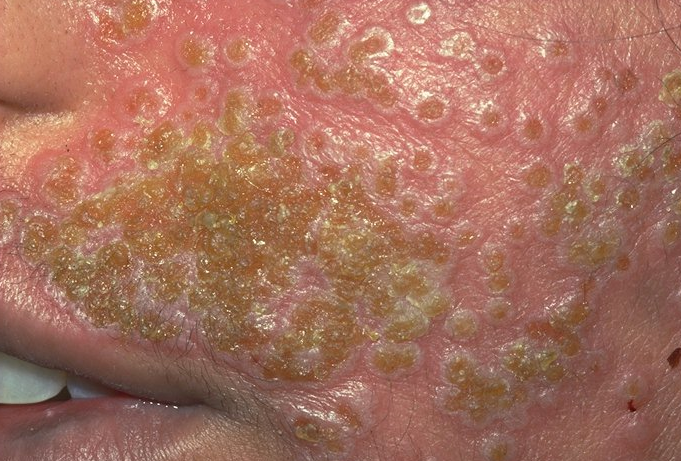
Symptoms of eczema herpeticum include red, fluid-filled blisters on the face and neck. Image courtesy of DermNet New Zealand
Eczema herpeticum usually appears on the face and neck. It can also appear on other places on the body such as the hands. It can take up to two weeks for symptoms to appear after the first contact with the herpes simplex virus.
Skin symptoms of eczema herpeticum include:
- Cluster of small blisters that are itchy and painful
- Blisters that look red, purple or black
- Blisters that ooze pus when broken open
Other symptoms of eczema herpeticum include:
- High fever and chills
- Swollen lymph glands
- Not feeling well overall
If you suspect you may have eczema herpeticum it is very important that you see a doctor immediately.
You May Like: Lotion For Children’s Eczema
Other Manifestations Of Herpes Simplex Virus Infection
HSV infections can occur elsewhere and can present manifest with life-threatening infection in some cases. Eczema herpeticum is a term used for disseminated cutaneous infection by HSV in patients with other chronic dermatologic conditions, including atopic dermatitis. Herpes gladiatorum is a unique cutaneous infection with HSV seen in individuals who wrestle. Transmission of virus occurs from infected individuals to susceptible persons during contact. Lesions usually develop on the lateral neck, face, and forearms, areas in direct contact with the face of the infected wrestling partner. Herpetic whitlow refers to infection of the digits, often the index finger. Whitlow caused by HSV-1 was more common before the widespread use of protective gloves in dental and medical personnel. Most cases of herpetic whitlow now are caused by HSV-2 infection, presumably acquired from sexual activity.
HSV-1 may also infect and reactivate in the cornea. There are about 25,000 new cases of ocular herpes per year in the United States with a total case burden of about 400,000. These cases are particularly problematic in that ocular recurrences are difficult to prevent, treatment is not entirely satisfactory, and frequent ocular reactivations can overwhelm the natural antiinflammatory capacity of the cornea, leading to blindness.
James G. MarksJr MD, Jeffrey J. Miller MD, in, 2019