How Is The Rash Treated
Treatment will depend on what has caused the rash. However, the recommended treatment for all individuals with HIV is antiretroviral therapy , which consists of medicines used for the purpose of controlling the virus, according to HIV.gov.
An individual may be prescribed three medications or a combined medication to take during the initial stages of ART. A person also might be able to switch to HIV medicine injections that would be given every two monthsbut only after meeting the following criteria indicated by the CDC:
- A level of viral load that is undetectable or achievement of viral suppression
- No history of failed treatment
- No known allergies to the medications within the injection
Of note, the ability to switch from pills to injections would be determined by the person’s healthcare provider.
Ultimately, as soon as you are aware of your HIV diagnosis, you should start ART immediately and adhere to the prescription guidelines for the medications exactlydoing so “reduces the amount of HIV in your body and helps you stay healthy,” the CDC said.
Additionally, healthcare providers will look for potential underlying causes like infections, alcoholism, severe sunburns, or emotional stress to further inform treatment. Thus, to get relief, you might be directed to use “moisturizers, lotions, baths, cortisone creams that relieve swelling, and antihistamines,” according to MedlinePlus.
How Do I Treat An Hiv Rash
If your HIV doctor diagnoses you with an HIV rash it is important to keep the affected areas clean and dry as possible which will help prevent the rash from spreading.
Also, do not take hot showers or hot baths as these have been shown to exacerbate the condition.
The typical treatment for HIV rash is topical creams and ointments that may help relieve the rash.
If your HIV rash becomes severe or does not respond to topical medications, then you will need to start taking HIV meds that don’t cause an HIV skin reaction such as Prezista or Isentress .
If you suspect or know that a medication for HIV has caused an HIV rash, than talk with your healthcare provider about changing medications. HIV rashes usually disappear within a few weeks after HIV medications are changed.
If your HIV rash has not responded to medication changes or the rash is severe, it may be caused by another condition and you should see your doctor right away for further diagnosis.
Noninfectious And Nonmalignant Cutaneous Manifestations Of Hiv Infection
For xerosis, emollients and dry skin care regimens are effective. For seborrheic dermatitis, coal tar, sulfur, and salicylic acid shampoos topical corticosteroids topical tacrolimus and 2% ketoconazole cream may be effective.
For psoriasis and Reiter syndrome, ultraviolet B and psoralen with UV-A may be useful. Systemic corticosteroids, methotrexate, and cyclosporine may increase the immune suppression and must be considered only with careful monitoring. Zidovudine is also reported to be useful in the treatment of HIV-associated psoriasis.
For pruritic papular eruption, topical steroids, UV-B, PUVA, and pentoxifylline have been reported to be effective. Eosinophilic folliculitis may respond to UV-B, isotretinoin, or zidovudine treatment. For severe aphthous stomatitis, tacrolimus is reported to be effective.
You May Like: Remedios Naturales Para El Eczema
Hiv/aids And Skin Conditions
Skin conditions are common in people with HIV/AIDS. Many, including Kaposi sarcoma, thrush, and herpes, are caused by germs that take advantage of a weakened immune system. That’s why they are called “opportunistic” infections. Others, like photodermatitis, may be linked to inflammation caused by an overactive immune system as it revives during antiretroviral drug therapy or due to the drugs themselves.
Here are some of the more common skin conditions related to HIV/AIDS.
Spectrum Of Skin Conditions
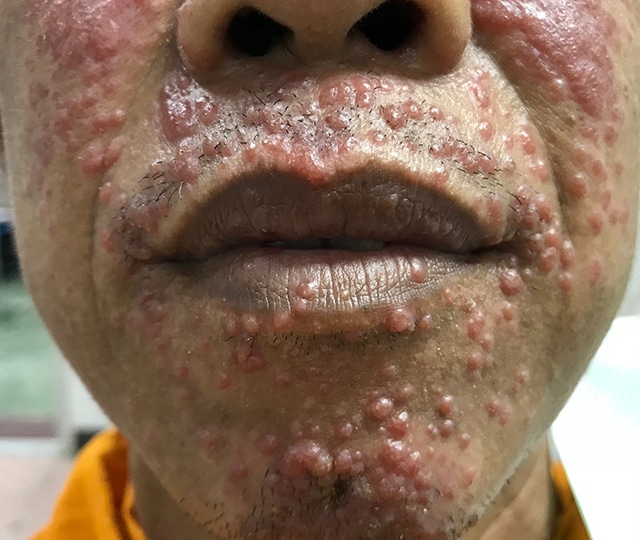
Primary HIV infection
Acute seroconversion syndrome is very much like Epstein-Barr virus infection. The patient presents with fever, sore throat, cervical adenopathy and exanthem which occur in 70% of the cases. The exanthem is an erythematous maculopapular eruption that may become confluent. This eruption distributes over the trunk and sometimes the palms and soles resembling secondary syphilis. Oral and genital erosions have also been reported. The histology is non-specific. It shows mononuclear cell infiltrates in the upper dermis.
Penicilliosis
Cutaneous manifestation is an important clue of Penicilllium marneffei infection as it presents in more than 75% of the cases. The characteristic skin lesions of disseminated P. marneffei are umbilicated papules with or without central necrosis. Nevertheless, penicilliosis can manifest as ulcers, nodules, maculopapules, acneiform lesions or folliculitis. Wright, Giemsa or PAS stain demonstrates intracellular and extracellular yeast-like organisms that are spherical to elliptical shape. The basophilic organisms have clear transverse septa.
Bacillary angiomatosis
Mycobacterial disease
The skin lesions of these mycobacterium species may take the form of nodules, plaques, papulonecrotic lesion, pustules, abscess or erythema nodosum. In practice, skin lesions of mycobacterial infection are rare even in the commonly encountered M. tuberculosis and MAI infection.
Herpes simplex virus
Varicella zoster virus
Molluscum contagiosum
Also Check: Cream To Stop Itching Eczema
Common Cutaneous Complications Of Hiv Disease
Instructor, Department of Dermatology,College of Physicians and SurgeonsClinical Instructor, Department of Dermatology,Mount Sinai School of MedicineSummary by Theo Smart Robert Warner, MDJames F. Braun, DO
From warts to scabies to malignancies, skin disorders are more common and more aggressive in HIV-positive patients than others, Dr. Jeffrey Roth told members of PRN. Dr. Roth presented a slide-show overview on the clinical manifestation and diagnosis of the cutaneous complications of HIV disease . At the same meeting, Dr. Charles Farthing reviewed the dermatologic procedures most useful for primary-care providers working with HIV-positive patients.
Stronger Houston: Houston Logging Some Of Nations Highest Hiv Diagnoses Health Officials Hoping For Vaccine In Near Future
HOUSTON The southern part of the U.S. accounts for 51% of new HIV cases each year, according to the Centers for Disease Control and Prevention. Some regions throughout the south also lag in providing HIV prevention services and care.
Space City, the fourth largest metro in the U.S., is known for reaching new heights. H-town is also logging some of the nations highest rates of HIV diagnoses and infection.
The idea that we have most of the burden of HIV, unfortunately in the south really speaks to other system issues, healthcare, and healthcare for people who are uninsured and not easily able to get access to care, there are the implications, theres more disease here, when those conditions are in existence. We actually average about 1,200 new HIV diagnoses each year.
McNeese said the covid19 pandemic caused disruption and reduction in access to HIV testing and at times treatment.
A Houstonian who does not want to be identified spoke to KPRC 2 about his personal story with HIV. He was diagnosed in during the pandemic and said he had no idea he was positive at the time he was tested.
September of last year. My advice to everyone out there, get tested immediately. You want to know your status. If more people would get tested, we could slow down the spread, he said.
The man who identifies as straight said his HIV diagnosis has changed his life for the better.
Read Also: Body Wash For Severe Eczema
Rashes Caused By Reactions To Medication
Another possible cause of a rash that develops when someone has HIV is a reaction to a medication. In fact, a rash is one of the most common side effects of antiretroviral medications used to treat HIV.
Rashes that develop due to HIV medications are usually not serious. Monitor the rash for several days to see if it goes away without treatment. If it does not, you may need to switch to a different type of medication or be tested for other possible causes of rash, such as a bacterial infection.
While most of the rashes that develop from taking ARV meds are harmless, its very important to be aware of a condition called Stevens-Johnson Syndrome . This is a rare but potentially fatal skin rash that may develop when taking certain HIV medications. The symptoms of SJS include:
- Fever, headache, and other flu-like symptoms
- Painful, itchy skin
- A skin rash consisting of red, blistered spots
- Peeling skin that develops into painful sores
- Blisters in and around the mouth, nose, eyes, genitals, or mucous membranes
If you experience symptoms of SJS, seek immediate medical care by visiting an emergency room or calling 911.
Of course, other medications besides HIV meds have the potential to cause a reaction like a rash. If you start taking any new medications, be sure to watch for the development of rashes or other unusual symptoms. In addition, you should work closely with your doctor to make sure any medications you take will not interfere with your HIV treatment.
Manifestations By Hiv Disease Stage
During acute primary HIV infection, a transient, generalized, morbilliform eruption may develop on the trunk and the arms. In the early asymptomatic stage of HIV disease, which may last from a few years to a decade or longer, no signs of infection other than lymphadenopathy are present. In a survey of 165 children in India with HIV infection, cutaneous manifestations were evident in 100 of them. Papular pruritic eruptions were evident in 16%, the most common condition, with highest prevalence in severe CD4 category. In one survey of 106 West African patients, the pruritic papular eruptions of HIV infection were mainly on the exposed parts of the body, especially the upper and lower limbs.
Kaposi sarcoma can occur prior to the onset of immunosuppression. With the onset of immunosuppression, nonspecific skin changes occur, such as common disorders with atypical clinical features, including recurrent varicella zoster, numerous hyperkeratotic warts, treatment-resistant seborrheic dermatitis, and oral hairy leukoplakia. However, Kaposi sarcoma of skin and/or oral cavity may develop in HIV patients with well-controlled HIV disease and may be a significant factor in their morbidity and mortality.
Also Check: Essential Oil Blend For Eczema
When To Be Worried About Rashes
Per MedlinePlus, rashes can be a sign of several medical conditions, but in general, rashes can be alleviated or eliminated with little issue. However, the American Academy of Dermatology Association identified conditions where seeing a dermatologist or emergency room staff would be highly warranted:
- full-body rashes
- sudden rashes that spread quickly
- blistering rashes
How A Weak Immune System Affects Your Skin
For some people with HIV, skin conditions are one of the most obvious signs of infection. Skin conditions can appear in the earliest stage of HIV, but may increase in frequency as the disease progresses.
HIV weakens your immune system, so your body is more likely to develop infection since it cant fight disease effectively. Common skin conditions that people with HIV experience include:
- Bacterial infections
- Inflammatory dermatitis
Inflammatory dermatitis can take many forms, and its common for people with HIV. Dermatitis can appear like areas of dry skin or red and itchy patches. Some examples of skin infections that people with HIV may contract include syphilis, oral thrush, and shingles.
Another condition that can develop if you have HIV is lipodystrophy. HIV can cause fat distribution in the body to change, resulting in fat loss around the face or fat buildup between the shoulder blades or elsewhere.
Taking antiretroviral medications for HIV generally helps reduce the number of skin conditions that people with HIV develop. Along with taking medication, getting regular skin exams and seeking treatment for specific skin conditions can help them from getting worse. For patients bothered by fat loss from HIV lipodystrophy, Sculptra® Aesthetic at Z-Roc Dermatology is an injectable filler to fill contours and improve your appearance.
Trust our team for all your skin care needs. Make an appointment at Z-Roc Dermatology online or call our office today.
You Might Also Enjoy…
You May Like: Best Way To Heal Eczema
Stage : Clinical Latency
In this stage, the virus still multiplies, but at very low levels. People in this stage may not feel sick or have any symptoms. This stage is also called chronic HIV infection.
Without HIV treatment, people can stay in this stage for 10 or 15 years, but some move through this stage faster.
If you take HIV medicine exactly as prescribed and get and keep an undetectable viral load, you can live and long and healthy life and will not transmit HIV to your HIV-negative partners through sex.
But if your viral load is detectable, you can transmit HIV during this stage, even when you have no symptoms. Its important to see your health care provider regularly to get your viral load checked.
Symptoms With An Hiv Rash
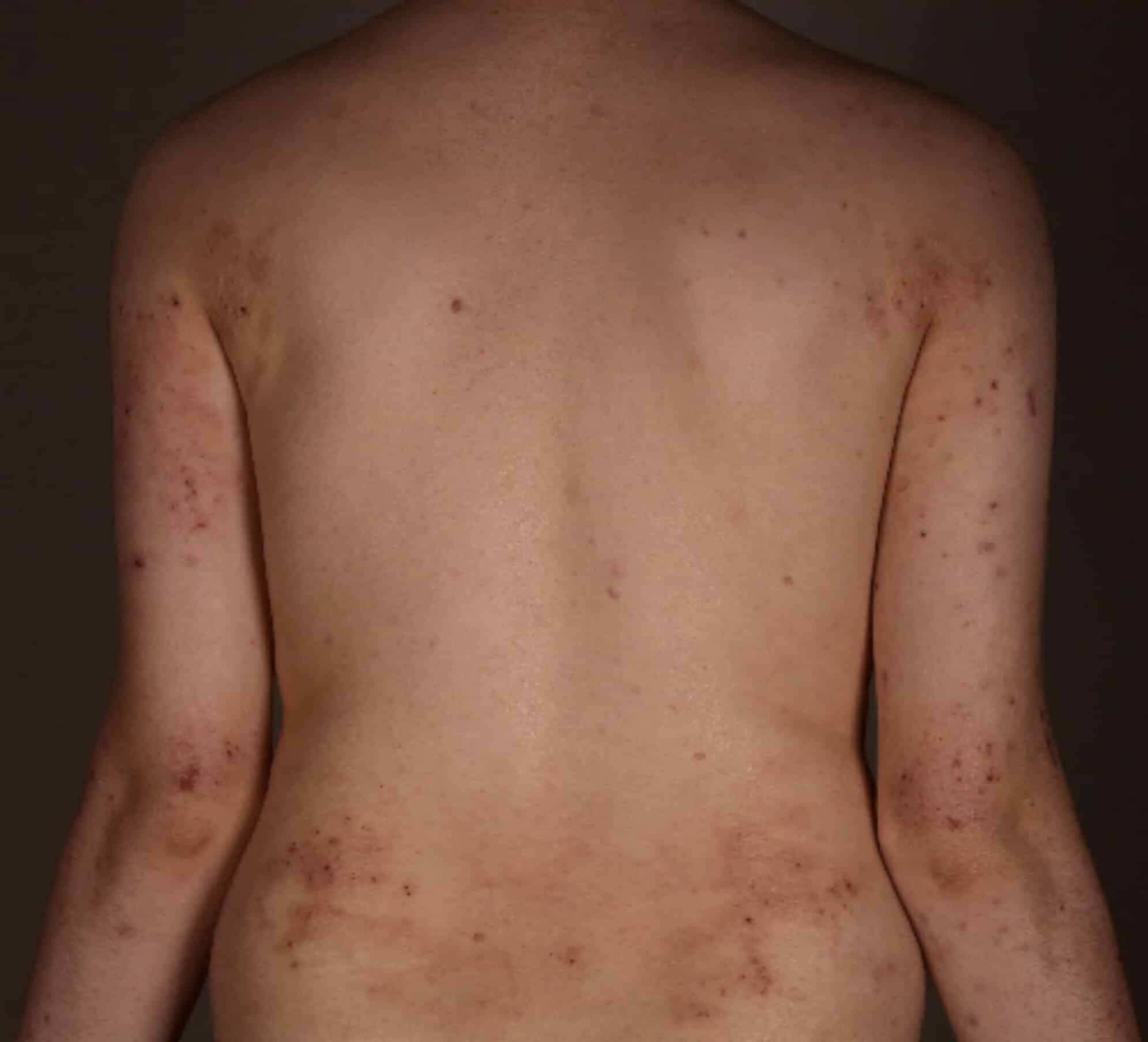
A rash can be an early sign of HIV, occurring as a result of seroconversion. This is the acute, or early stage of HIV, which occurs within 12 weeks of exposure to the virus.
During the seroconversion or acute HIV stage, the body produces antibodies to the virus. Between half and 8090% of all people with HIV experience flu-like symptoms at this stage and some people may develop a rash.
Sometimes, a rash is the only symptom of HIV, but because HIV impacts the immune system, there are often other symptoms, too.
Early of an HIV infection that can occur alongside a rash include:
after exposure and last between a few days and several weeks.
Anyone who experiences these symptoms after possible exposure to HIV should seek advice about testing.
Read Also: Eczema At Base Of Scalp
What Is Human Immunodeficiency Virus
HIV is a blood-borne virus, a member of the Retroviridae family that can be transmitted by sexual intercourse, intravenous drug materials contaminated by the virus, mother-to-child during birth or breastfeeding and cause immunodeficiency in the person infected. Diagnosis is done by having a positive lab test for HIV. There is no cure for HIV but antiretroviral treatment can control the virus so patients can live long and healthy lives.
Hiv Weakens Your Immune System
HIV attacks your white blood cells. White blood cells are the cells in your body that fight infection and keep you healthy. If you have HIV, your white blood cell count gets low and your body cant fight infection effectively.
HIV generally has three stages. The first stage is an acute HIV infection. Symptoms develop two to four weeks after infection occurs, and can appear like the flu. During the first stage, theres a high amount of the HIV virus in your blood and the virus is very contagious.
The second stage is HIV inactivity. This stage can last anywhere from 10 years to several decades if youre taking medicine to treat HIV. There may not be many symptoms during this stage, but you can still transmit the disease to others.
Stage three of HIV is AIDS. People with AIDS have extremely weakened immune systems and suffer an increasing number of illnesses and infections.
If left untreated, HIV can progress quickly and develop into AIDS in just a few years. There are a number of medications that can slow the progression of HIV, improving your health and quality of life for many years.
Don’t Miss: Eczema On Eyelids And Under Eyes
Skin Problems Caused By Infections
Infections are generally divided into three main groups: bacterial, fungal or viral infections. Some people will experience skin problems unrelated to their HIV diagnosis, as these are a common health issue. Some of the conditions described here are most common in people with a low CD4 cell count. Starting HIV treatment will help reduce the likelihood of them occurring.
Eczema has many causes and may be treated with antihistamines. To relieve any dry skin condition, moisturise frequently to stop the skin drying out further. Avoid long baths and the use of soap, shower gels and other potential irritants. Instead, use aqueous cream or moisturiser to wash with. Corticosteroid creams can reduce swelling and redness, and antihistamines can reduce itching. Try not to scratch, as this can make eczema worse and cause scarring.
Dermatitis is identified by red patches and a flaky rash. It may be caused by contact with an irritating substance or by eczema. Seborrhoeic dermatitis often occurs in hairy parts of the body. It causes red, itchy, flaky, inflamed skin. Mild cases cause dandruff. Its common in symptomatic HIV, and it can be harder to treat in people living with HIV. Dermatitis may be treated with steroid ointments or tablets, or with anti-fungal creams or tablets. Some scalp problems can be treated with anti-dandruff or anti-fungal shampoos.
human papilloma virus
A Sexually Transmitted Infection
Katie Salerno/Flickr Creative Commons
If you have a sexually transmitted infection , there is a chance you may have HIV as well.
Some STIs like syphilis and herpes cause open sores that make it easier for HIV to get inside the body.
STIs like gonorrhea and chlamydia cause inflammation in the genitals that attract the immune cells that HIV likes to target and infect.
Having syphilis can increase your risk of HIV by as much as 500%. Other STIs can also raise your risk for HIV. You should be tested for HIV if you test positive for any STI.
Recommended Reading: Zinc Oxide For Eczema On Face
Management Of Skin Conditions In Hiv/aids
Classification of HIV dermatosis
Skin diseases of HIV-infected persons can be systematically classified by their pathogenesis . Selected skin diseases are discussed in this chapter.
Diagnosis
The drug history, morphology of primary lesion and CD4 count, are important clues to skin diagnoses. In many cases, HIV-associated skin diseases can be easily recognised on clinical grounds, especially in the early HIV disease where clinical atypia is less frequent.
When diagnostic difficulty is encountered, skin biopsy should be considered for both histologic and microbiological evaluation. As HIV-infected persons frequently have more than one dermatosis, several biopsies may be necessary.
Treatment
Skin diseases are rarely life-threatening, but many of them are life-ruining. While the lifespan is prolonged by the use of HAART, many HIV-infected patients are troubled by drug-induced facial lipoatrophy. Not only can there be cosmetic disfigurement, the intense pruritus due to eosinophilic folliculitis may severely impair the patients’ quality-of-life. Therefore, management of these apparently minor conditions should not be overlooked.