When To See A Healthcare Provider
If you’re worried you may be experiencing symptoms of an autoimmune condition, be sure to see a healthcare provider for a comprehensive evaluation, which will include a thorough physical examination, blood tests, and possibly imaging tests.
If your primary care or family healthcare provider suspects an autoimmune process, you will likely be referred to a specialist, such as a rheumatologist , an endocrinologist , or a gastroenterologist .
Things To Know About Autoimmune Disease
Chronic illnesses can be challenging. Those affecting the liver, like Autoimmune Hepatitis , Primary Sclerosing Cholangitis and Primary Biliary Cholangitis are no exception. While research advances daily, theres still much to learn. Here are eight things to know about autoimmune diseases:
Association Between Ad And Celiac Disease
Prevalence of celiac disease in AD and controls was reported in four studies . Meta-analysis showed a higher prevalence of celiac disease in AD compared to controls. The synthesized OR was 1.98 with high heterogeneity . Only one cohort reported an increased incidence of celiac disease in AD, with a RR of 1.41 .
You May Like: Best Cream For Dyshidrotic Eczema
How Are These Autoimmune Diseases Diagnosed
Because conditions such as lupus and scleroderma have symptoms that can resemble many other diseases, they can be difficult to diagnose initially. Lupus, for instance, can have symptoms that include fatigue and fever. Symptoms of scleroderma can include heartburn.
When you notice the first symptomsgenerally some form of skin rash that doesnt go away or that worsens over timeyou may seek treatment from a primary care doctor or dermatologist. An examination with a doctor can include discussion of symptoms, personal medical history and family history, as well as blood and other laboratory tests . The patient may then consult with a rheumatologist, who will have more experience working with the internal symptoms of the disease. Over time and depending on his or her symptoms, a patient may work with either a dermatologist or a rheumatologist, or both.
Sexspecific Association Between Atopic Dermatitis And Autoimmune Disease
In the overall analysis, men had a stronger association between AD and autoimmune diseases than women . However, this sex difference was only statistically significant between AD and RA and between AD and coeliac disease. In addition, AD in men, but not in women, was associated with DM1. Moreover, in sexstratified analyses, AD only in women was associated with dermatomyositis, systemic scleroderma, SLE, Hashimoto disease, Graves disease, multiple sclerosis and polymyalgia rheumatica.
You May Like: Steroid Ear Drops For Eczema
What Type Of Blood Tests Are Used To Diagnose Autoimmune Diseases
Several different blood tests may be used to diagnose an autoimmune disease. In addition to a regular complete blood count and metabolic panel, other tests that are likely to be included are anti-dsDNA, anti-RNP, anti-Sm, anti-Sjogren’s SSA and SSB, anti-scleroderma, anti-Jo-1, anti-CCP, antibody against cardiolipin, and an antinuclear antibody test. A rheumatoid factor test, which looks for rheumatoid arthritis, is also usually included during the diagnostic phase. The antinuclear antibody test looks for antibodies that could cause an autoimmune response.
The Link Between Celiac Disease And Hives
According to one study, people with celiac disease were 1.5 times more likely to develop hives. In some cases, people may even be diagnosed with hives first, before being diagnosed with celiac disease. Researchers found that about a third of the cases of chronic hives could be attributed to the underlying celiac disease. Celiac disease is also more common among women.
Recommended Reading: Eucerin Eczema Relief Cream Walgreens
Autoimmunity In Atopic Dermatitis
- Division of Immunodermatology and Allergy Research, Department of Dermatology and Allergy, Hannover Medical School, Hanover, Germany
Atopic dermatitis , one of the most frequent inflammatory skin diseases worldwide, is believed to result from a disturbed skin barrier as well as aberrant immune reactions against per se harmless allergens. Starting mostly during childhood with a chronic, remitting relapsing course, the disease can persist into adulthood in about one fifth of patients. Immune reactions to self-proteins have been observed in AD patients already in the beginning of the Twentieth century, when human cellular extracts were shown to provoke skin lesions. However, the term autoimmunity has never been claimed, since AD is first and foremost an atopic disease. In contrast, this IgE-hallmarked autoreactivity was termed autoallergy and is ongoing discussed regarding its impact on the disease. Since severely affected patients tend to develop IgE-hypersensitivity reactions to numerous environmental allergens, the impact of immune responses to self-proteins is difficult to determine. On the other hand: any autoreactivity, irrespective of the magnitude, implicates the potential of driving the chronification of the disease while shaping the immune response. This review article revisits the observations made on autoallergy from an actual point of view and tries to approach the question whether these still point to a contribution to the disease.
Does A Unique Immune Pathway Dysfunction Occur In A Subset Of Patients With Atopic Dermatitis
In a cross-sectional study of hospitalized adults and children in the United States, patients with atopic dermatitis were found to have higher rates of various autoimmune disorders, including those affecting the skin, endocrine, gastrointestinal, hematologic, and musculoskeletal systems, than patients without AD1
Take Note
- Pediatric and adult AD patients hospitalized in the United States suffer higher rates of both cutaneous and extracutaneous autoimmune diseases than patients without AD.
- Autoimmune disorders were particularly increased among children of Asian race/ethnicity with AD, as well as among patients of all ages without asthma.
- Clinicians should increase screening for autoimmune disorders in AD patients.
While AD, which affects as many as 10% of adults and 13% of children in the US, has long been associated with other atopic conditions including asthma and food allergies, the relationship between AD and autoimmune disorders is not as well recognized.1 Proposed mechanisms for AD include epidermal disruption, decreased cutaneous antimicrobial peptide expression, aberrant toll-like receptor signaling, and dysfunction of the innate immune system, which could contribute to development of other inflammatory disorders, including autoimmune disease.1
Clinical findings shed light on the pathophysiology of AD
Don’t Miss: What Is Eczema And Psoriasis
Data Extraction And Quality Assessment
We extracted surname of the first author, publication year, country/region, study design, demographic characteristics in the case and control groups, assessment used for AD and autoimmune diseases, risk estimates with 95% CI and corresponding adjustments for confounders. The methodological quality of selected studies was evaluated using the NewcastleOttawa Scale , which comprised three main items including sample selection, comparability and exposure/outcome. Studies could be awarded a maximum of one star for each numbered item within the selection and exposure/outcome categories and a maximum of two stars for comparability category, with a score of 13, 46, and 79 represented as of low, intermediate, and high quality respectively. Two authors independently conducted quality assessments of the included studies. Discrepancies were discussed and resolved by the authors.
For The First Time Study Proves Eczema Is An Autoimmune Disease
An experimental drug that works by blocking the immune response that causes unsightly, itchy skin patches looks promising for treating atopic dermatitis , also known as eczema.
Atopic dermatitis , or eczema, affects 10 percent of adults in the United States and about 25 percent of children worldwide.
AD is an inflammatory disorder in which the skin becomes covered in itchy, scaly lesions. These lesions cause cracks in the skins outer barrier, exposing patients to infection. AD is always accompanied by activation of the immune system.
Learn the Difference Between Psoriasis and Eczema »
A new study shows that dupilumab, a type of drug called a monoclonal antibody , can reverse the immune response that causes AD skin lesions. Many of the scientists who conducted the study are employed by Regeneron Pharmaceuticals, the makers of dupilumab. The study was published in the Journal of Allergy and Clinical Immunology.
You May Like: The Best Medicine For Eczema
Is Eczema A Sign Of A Weak Immune System
No, having eczema doesnt automatically mean you have a weak immune system. It does mean that your immune system is sensitive, often overreacting to things that arent real threats to your body.
Some people with eczema have a primary immunodeficiency disorder that may make them more likely to get infections. But eczema can also affect people with healthy immune systems.
What Are The Blood Tests For Autoimmune Diseases
There are some blood tests one can do that can reflect how active the immunological disease is inside our bodies in diseases like rheumatoid arthritis, lupus, and scleroderma. These tests are routinely ordered by doctors who are treating such patients. This information can be very helpful at times both in the diagnosis of the specific problem and in guiding treatment of the problems over time.
Recommended Reading: Palmar Psoriasis Vs Hand Eczema
Is Eczema Caused By A Weak Immune System
Eczema isnt believed to be the result of a weak immune system.
But researchers dont know exactly what causes eczema, according to the National Eczema Association . Experts think genes and a variety of triggers are contributing factors.
When you have eczema, the skin barrier that would normally keep out allergens, bacteria, and other germs isnt working as it should. Instead of keeping unwanted elements out, breaks in your skins barrier allow them to seep in, according to .
Once allergens or other substances are inside your body, your immune system reacts.
It sends out an army of white blood cells that release chemicals and other substances to destroy the invaders. These substances are responsible for your skins inflammation.
Think about when you cut yourself or skin a knee. Your immune system responds to the injury by producing redness, itching, swelling, and pain at the site. This is a good thing proof that your immune system is strong and healthy.
Skin Conditions Linked To Lupus
Lupus is known to cause a number of skin problems, including hives, cutaneous vasculitis , photosensitivity, alopecia, and purpura . About 10 percent of all people with lupus will experience hives. Most individual hives will fade and disappear within hours, while new welts flare. Individual hives lasting more than 24 hours may be due to inflammation in the blood vessels that could be due to lupus.
Don’t Miss: How To Get Rid Of Eczema On Your Face
Hyperthyroidism Hypothyroidism And Chronic Hives
Autoimmune thyroiditis may cause hyperthyroidism or hypothyroidism. Chronic hives may be linked to either. Hyperthyroidism, or an overactive thyroid gland, can cause irritability, muscle weakness, sleep problems, a fast heartbeat, heat intolerance, diarrhea, hand tremor, and weight loss. Hypothyroidism is caused by an underactive thyroid, which can cause sensitivity to cold, as well as fatigue, constipation, depression, weight gain, hair loss, and dry skin.
How Are These Autoimmune Diseases Treated
While there are currently no curative treatments for these autoimmune diseases, there are courses of action that can lead to periods of remission or a reduction in flare-ups. Depending on the symptoms, there is a range of options that may be used singularly or in conjunction with each other. The symptoms that affect the skin are often the first and sometimes the only ones that appear and are often comparatively easier to treat than those that affect internal organs.
- Lupus: Over-the-counter anti-inflammatory drugs such as Motrin may be used in some patients to treat swelling and pain. Another option to treat inflammation is corticosteroids, though side effects can include a higher risk of contracting infections. Anti-malarial drugs including Plaquenil are often used to treat the symptoms of lupus because theyve been shown to alleviate joint pain, improve skin rashes and help reduce flare-ups significantly. Doctors may also prescribe immunosuppressants such as Azasan , which suppress the immune system to prevent it from attacking the cells it shouldnt be attacking.
Additionally, because ultraviolet light can cause flare-ups, patients are advised to be very careful with sun exposure, wearing sun-protective clothing, hats and sunscreen with a high SPF. There are certain local treatments that can be helpful but number one is sun protection, says Dr. Ramachandran.
Recommended Reading: Medicated Eczema Cream For Babies
Rheumatoid Arthritis And Chronic Hives
Rheumatoid arthritis has been found to be the second most common autoimmune disease in patients with chronic hives.Rheumatoid arthritis is when the bodys immune system mistakenly attacks the joints, causing the tissues that line the inside of joints to thicken. People with this inflammatory autoimmune disease can be prone to different skin conditions, including chronic hives. One study found that female patients with chronic hives were more likely to be diagnosed with rheumatoid arthritis.
Chronic Autoimmune Illnesses Linked To Chronic Hives
by Health Writer
Chronic hives can be a formidable foe, especially when its not clear whats causing the itchy, red welts or wheals that can appear anywhere on the body and recur for six weeks or more. Sometimes a hidden illness may be an underlying cause. Studies have found a strong association between chronic hives and autoimmune diseases such as thyroid disease, rheumatoid arthritis, celiac disease, type 1 diabetes, Sjögren syndrome, and lupus.
Don’t Miss: How To Treat Vulva Eczema
Association Between Ad And Rheumatoid Arthritis
Five studies reported the prevalence and three cohort studies reported the incidence of rheumatoid arthritis in patients with AD. The prevalence of rheumatoid arthritis was higher in AD compared to control . The incidence was also higher in AD compared to control, with an average RR of 1.38 , which meant AD could increased the risk of developing rheumatoid arthritis.
Is Dyshidrotic Eczema An Autoimmune Disease
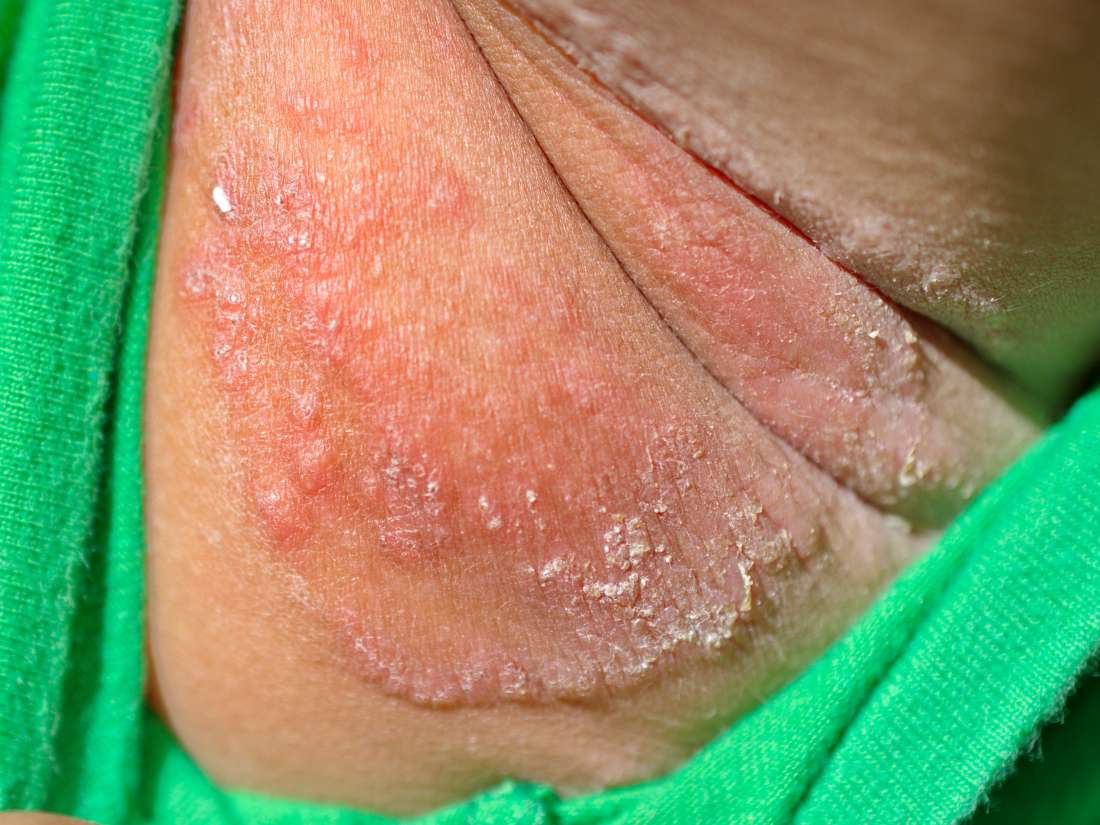
Dyshidrotic eczema, or pompholyx, causes small, itchy blisters on the soles, palms, and edges of the fingers and toes. The cause is unknown, but many people living with the condition also have another form of eczema. In addition, doctors have noted that dyshidrotic eczema can run in families.
Some common triggers for flare-ups include:
- seasonal allergies, such as hay fever
- heat and humidity
- stress
Few studies have looked at the immune response in people with dyshidrotic eczema, so it is unclear if it has an autoimmune component.
Nummular eczema causes coin-shaped patches that are often itchy and sometimes oozing. The patches can appear anywhere on the skin. Experts do not know what causes nummular eczema, but they think it has links with:
- having dry or sensitive skin
- having other types of eczema
- metal allergies
- cuts, insect bites, or chemical burns
- low blood flow in the legs, if the patches appear there
No research has looked at whether nummular eczema could be an autoimmune disease.
Read Also: Does Shea Butter Help With Eczema
Can Eczema Be A Sign Of Other Conditions
Eczema isnt a sign that you have other illnesses. However, it can look similar to or happen alongside other conditions.
Symptoms like itchy and red skin are also common with other skin conditions that are easy to mistake for eczema. These conditions are:
- Psoriasis: an autoimmune disease that causes your skin cells to multiply too fast
- Hives: large red welts on the skin caused by an allergic reaction
- Cutaneous T-cell lymphoma: a cancer of the white blood cells that starts in the skin
- Scabies: a skin infestation by a type of mite
- Ringworm: a skin infection caused by a fungus
Eczema is sometimes part of a cluster of allergic conditions that healthcare professionals call the atopic march. These include:
- asthma
- allergic rhinitis
- food allergies
If you have one of these three conditions, youre more likely to have another one.
In addition, your eczema may be more severe if you have one of these primary immunodeficiency diseases:
- Wiskott-Aldrich syndrome
2020 research . Stress can trigger eczema flare-ups and make symptoms worse.
When youre feeling overwhelmed or threatened, your body releases certain chemicals, including stress hormones like adrenaline and cortisol. These substances suppress your immune system, boost inflammation, and weaken your skins barrier even more.
Stress and eczema may become connected in a cycle. The more your eczema flares, the more stressed you may become. And the more stressed you are, the more your eczema flares.
What Is Cdc Doing About Psoriasis
In 2010, CDC worked with experts in psoriasis, psoriatic arthritis, and public health to develop a public health perspective that considers how these conditions affect the entire population. The resulting report is Developing and Addressing the Public Health Agenda for Psoriasis and Psoriatic Arthritis pdf icon. You can read a short article about the agendaexternal icon in The American Journal of Preventive Medicine.
CDCs National Health and Nutrition Examination Survey , an intermittent source of national psoriasis data, has included questions about psoriasis as late as the 2013-2014 cycle. A recent analysis of NHANES data estimates that 7.4 million adults had psoriasis in 2013external icon.
- Psoriasis causes patches of thick red skin and silvery scales. Patches are typically found on the elbows, knees, scalp, lower back, face, palms, and soles of feet, but can affect other places . The most common type of psoriasis is called plaque psoriasis.
- Psoriatic arthritis is an inflammatory type of arthritis that eventually occurs in 10% to 20% of people with psoriasis. It is different from more common types of arthritis and is thought to be related to the underlying problem of psoriasis.
- Psoriasis and psoriatic arthritis are sometimes considered together as psoriatic disease.
Who is at risk for psoriasis?
Anyone can get psoriasis. It occurs mostly in adults, but children can also get it. Men and women seem to have equal risk.
Can I get psoriasis from someone who has it?
Don’t Miss: White Spots On Skin Eczema